To the Editor:
Lipodystrophy is a rare disease characterized by loss of adipose tissue that can be associated with metabolic disorders and autoimmune diseases, primarily juvenile dermatomyositis. Lipodystrophy in association with adult-onset dermatomyositis, however, is very rare.
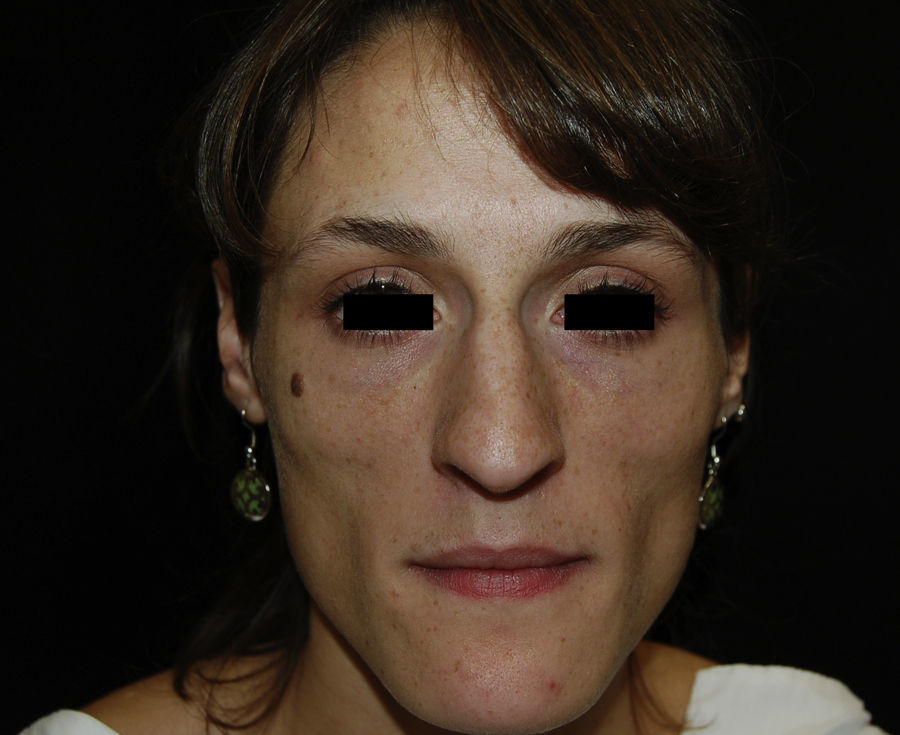
A 23-year-old woman consulted for erythema and bilateral palpebral edema that had appeared 1 year earlier and skin lesions on the dorsum of the interphalangeal joints of both hands. The patient reported that she had experienced muscle pain and weakness over the last 6 months, as well as joint pain in her hands, wrists, elbows, and knees. She also mentioned a progressive loss of fat in the facial region and arms over the last 2 months. The patient had no past history of interest and was not taking any medication. She also reported no family history of connective tissue disease.
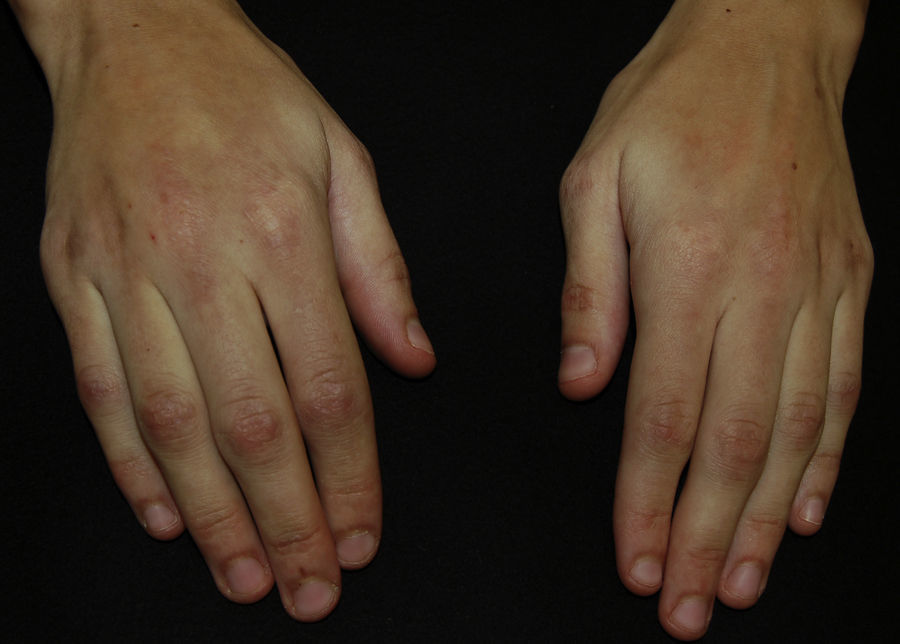
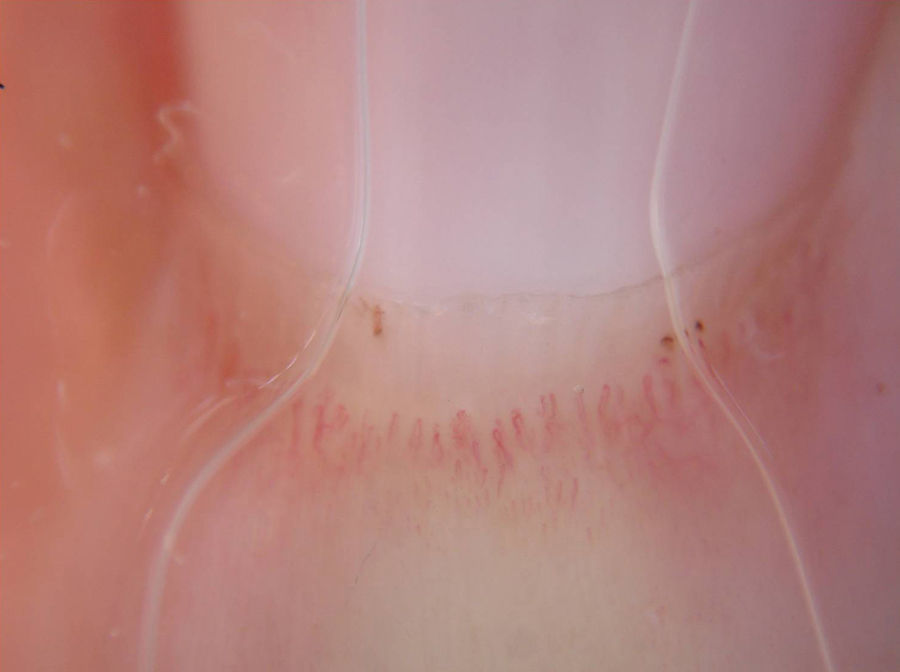
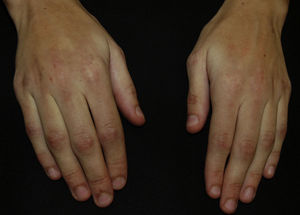
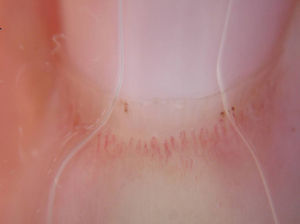
In the physical examination, we observed a marked loss of adipose tissue in the face and arms; the trunk and lower limbs were unaffected by this loss (Fig. 1). There were atrophic erythematous lesions on the skin of the elbows and interphalangeal joints of the fingers (Fig. 2). We also detected the presence of periorbital erythema and periungual telangiectasia (Fig. 3). The patient had rigidity in the joints of the hands, with no signs of arthritis, and proximal muscle weakness (grade 4-5 according to the Medical Research Council scale).
The blood tests showed normal levels of creatine kinase and aldolase. The results of the antinuclear antibody test were positive, with a titer of 1:320 and a granular pattern. The C3 and C4 fractions of the complement were within normal limits. The anti-Jo1, anti-Ro, anti-La, anti-nRNP, anti-Sm, anti-ssDNA and anti-dsDNA antibody test results were negative. We detected no abnormalities in serum lipid or glucose levels.
Biopsy of the hand lesions showed lichenoid dermatitis with hydropic degeneration of the basement membrane and upper dermal edema. There were no immunoglobulin (Ig) G, IgA, fibrinogen, or complement deposits in the direct immunofluorescence assay. An electrophysiological study showed no abnormalities. We therefore performed a muscle biopsy, which revealed muscle fiber necrosis and a lymphoplasmacytic inflammatory infiltrate. Magnetic resonance imaging showed thickening of the perimuscular fascia of the arms, shoulders, buttocks, and thighs. Based on the above findings, we arrived at the diagnosis of dermatomyositis. Given this diagnosis in an adult, we followed up with positron emission tomography, which ruled out underlying neoplastic disease at the time of the visit and 2 years later.
Lipodystrophy is a rare disease characterized by the loss of subcutaneous adipose tissue. It is classified as inherited or acquired and, depending on its location, as generalized, partial (relatively extensive but not generalized), or localized.1 When lipodystrophy is generalized or partial, it is often associated with metabolic disorders, such as insulin resistance and hypertriglyceridemia.1
Acquired lipodystrophy has been associated with infections, antiretroviral therapy for the treatment of human immunodeficiency virus infection and with autoimmune diseases such as rheumatoid arthritis, systemic lupus erythematosus, Sjögren syndrome, and dermatomyositis.2 Dermatomyositis (specifically, juvenile dermatomyositis) is the autoimmune disease most frequently related to the development of lipodystrophy.3 The prevalence of lipodystrophy in juvenile dermatomyositis varies among studies from 10% to 40%. In the only study performed with a large number of patients, acquired lipodystrophy was observed in 8% of patients with juvenile dermatomyositis, while only 1 of the 692 adult patients with dermatomyositis had lipodystrophy.4 To date, only 2 cases of lipodystrophy associated with adult-onset dermatomyositis have been published.5,6 The reasons for this lack of association are unknown.
One study has shown that a number of manifestations of dermatomyositis, such as joint rigidity, muscle atrophy, panniculitis, and calcinosis, could be related to the development of lipodystrophy.4 Of all these signs, our patient had only joint rigidity in the hands.
The etiology and pathogenesis of lipodystrophy associated with autoimmune disease remain unclear. Patients with partial lipodystrophy often have low C3 levels, which may trigger the alternative complement pathway and promote development of the disease.2
The majority of patients described in the literature developed lipodystrophy years after the onset of dermatomyositis, as a late complication of severe, chronic disease; our patient, however, developed symptoms of dermatomyositis and lipodystrophy practically simultaneously. In contrast to what occurs in most cases of partial lipodystrophy, there were no metabolic abnormalities in our patient. We were also unable to demonstrate etiologic or pathogenic mechanisms associated with immunologic abnormalities such as low levels of C3. In agreement with reports from similar cases in the literature,5,6 treatment with oral prednisone and mycophenolate mofetil did not improve the facial lipoatrophy in our patient.
We have presented a very rare case of adult lipoatrophy simultaneously associated with dermatomyositis.
Based on published data, it would be prudent to closely monitor all patients with dermatomyositis who develop a loss of subcutaneous fat in order to progressively rule out abnormalities in the metabolism of lipids and carbohydrates.
Please cite this article as: Pretel M, et al. Dermatomiositis del adulto asociada a lipodistrofia. Actas Dermosifiliogr. 2013;104:724–5.