The genetic skin disease known as Brooke-Spiegler syndrome (BSS) is a rare autosomal dominant condition with more than 50 cases reported to date.1 BSS predisposes to benign adnexal tumors that generally first appear in adulthood and involve the folliculo-sebaceous-apocrine unit. It is characterized by multiple cylindromas, trichoepitheliomas, and, occasionally, spiradenomas.2 The tumors appear simultaneously, as in BSS, or in isolation, as in familial cylindromatosis and multiple familial trichoepithelioma. Consequently, they seem to have a common origin in a pluripotent cell in the folliculo-sebaceous-apocrine unit, with several phenotypic variants.3,4
Various mutations have been identified in the tumor suppressor gene CYLD on chromosome 16q12-913, thus indicating an association with BSS. CYLD inhibits the tumor necrosis factor α pathway, diminishing expression of nuclear factor κB (NF-κB), a transcription factor that in turn regulates various antiapoptotic genes involved in the proliferation of adnexa. A loss of the suppressive function of CYLD leads to greater resistance to apoptosis and, consequently, the appearance of these tumors.3–5
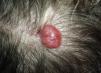
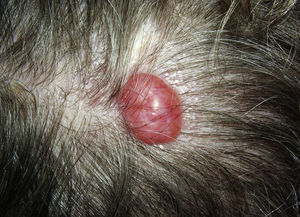
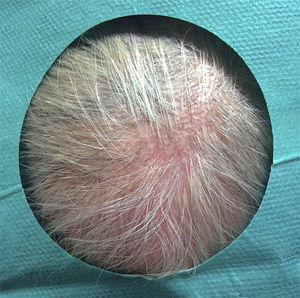
Clinically, cylindromas present as pink nodules on the scalp and behind the ears (Fig. 1). Trichoepitheliomas appear as papules or small translucent or flesh-colored nodules and are located mainly in the center of the face, especially in the nasal region. Spiradenomas, on the other hand, usually present as solitary bluish or flesh-colored nodules that are often painful.2
The emotional impact of recurrence of these lesions on the face and scalp makes treatment essential. Our literature search revealed various options, such as electrocautery, dermabrasion, radiofrequency, cryotherapy, CO2 laser,6 radiotherapy (in special cases),7 and, recently, enucleation.8 The treatment recommended for solitary cylindromas is surgical removal, whereas partial or total skin grafting has been proposed for multiple lesions.9 NF-κB inhibitors, such as acetylsalicylic acid and its derivatives, may prove useful both for prevention and for treatment of cylindromas when applied locally.10 Therefore, treatment should be tailored depending on the patient, size of the lesion, number of lesions, therapeutic options available, and the dermatologist's experience.
We report the case of an 80-year-old woman with BSS who presented with multiple cylindromas on the scalp that had recurred since adolescence, together with occasional spiradenomas. Her family history was remarkable in that one of her daughters, aged 49 years, had had numerous facial trichoepitheliomas since puberty. She has been followed regularly in our department for the last 10 years, and several lesions have been removed using elliptical excision and direct closure. Given the high number of lesions and the excisions performed, we sought an alternative that would make for more efficient surgery and benefit the patient by reducing the number of trips to the hospital. Five years ago, we began to perform a technique that combined cytoreduction and subsequent curettage of the growths. Our technique is minimally invasive and efficacious.
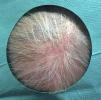
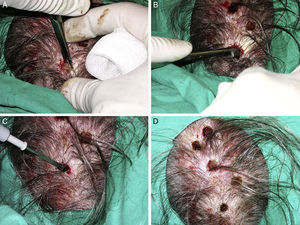
After administration of local anesthetic (mepivacaine 2%), an incision is made with a scalpel or scissor cut to enable resection of most of the tumor mass and create a portal of entry for the next step. After debulking, the remaining lesional tissue is removed by intense curettage, and bleeding is stopped using electrocautery. The resulting wound heals by secondary intention (Fig. 2). Complete scarring is achieved within approximately 14 days based on daily dressing with antiseptic and antibiotic ointment. The wound progresses without complications after surgery, and the cosmetic outcome is favorable at the 12-month visit (Fig. 3). Regular follow-up has revealed a reduction in the number of cylindromas and a rate of recurrence of the lesions removed lower than 25%. When the lesion did relapse, the growth was always smaller than the original lesion, thus facilitating surgery.
Our technique enables us to reduce the volume of the lesions by eliminating several growths during the same procedure. This is particularly advantageous in patients who must undergo repeated procedures. It also enables us to concentrate on the emergence of new lesions, since cylindromas rarely recur after removal using this technique. This is because elimination of the lesions by combining several techniques in one procedure (eg, debulking with scissors, followed by curettage of the wound bed, and subsequent use of an electric scalpel) enables almost total necrosis of any remaining cells and destruction of the hair follicles, which are a potential source of new tumors.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Lucas-Truyols S, Lloret-Ruiz C, Millán-Parrilla F, Gimeno-Carpio E. Método simple y efectivo para el tratamiento de los cilindromas en el síndrome de Brooke-Spiegler. Actas Dermosifiliogr. 2017;108:692–694.