Telangiectasias due to drugs or iatrogenic damage are very rare. Some of the responsible drugs are lithium, interferon-alfa, and isotretinoin.1 However, when telangiectasias appear in sun-exposed areas, they are usually related to the use of calcium channel blockers (CCB), although this has also been reported in association with other drugs such as venlafaxine and cefotaxime.2,3
In these cases, lesions appear in sun-exposed areas a few months after starting the treatment. The prognosis is good, as a correct diagnosis followed by a change of treatment to a drug from another group, will lead to a rapid improvement and complete or almost complete disappearance of the lesions.
We present a patient with photodistributed telangiectasias associated with treatment with amlodipine. The lesions disappeared a few weeks after discontinuation of the treatment.
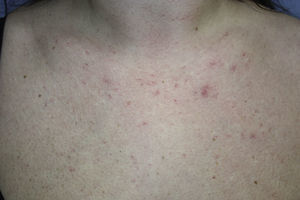
A 36-year-old woman consulted for the appearance of erythematous lesions that had arisen on the face and in the presternal region approximately 10 months earlier and for which she had received no treatment. A relevant finding in her past history was systemic hypertension on treatment with amlodipine for the previous year. She denied any history of rosacea or the use of topical corticosteroids. On examination, numerous erythematous-purpuric lesions and reticulated blood vessels were observed in the anterior thoracic region. All the lesions measured less than 1cm in diameter and they blanched on pressure (Fig. 1). A few similar lesions were observed on the dorsum of the nose. Histology showed slight dilatation of the capillaries of the vascular plexus of the superficial dermis and a minimal lymphohistiocytic perivascular infiltrate; there were no signs of vasculitis and no increased presence of mast cells. Blood tests, including complete blood count, biochemistry, and basic autoimmune studies, were normal or negative.
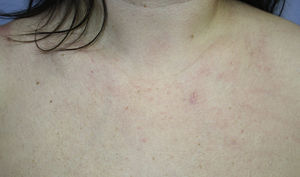
Given the chronologic correlation between the initiation of treatment and the subsequent appearance of the lesions, the patient was diagnosed with amlodipine-related photodistributed telangiectasia, and this treatment was therefore substituted by enalapril. Six weeks later a significant improvement was observed, with disappearance of the majority of the lesions (Fig. 2).
CCBs are a group of drugs widely used for the treatment of cardiovascular diseases such as systemic hypertension and ischemic heart disease.4 Adverse skin reactions associated with these drugs are rare. Pruritus, urticaria, alopecia, Stevens-Johnson syndrome, and toxic epidermal necrolysis are the forms most frequently reported.1,4,5
Cases of CCB-related photodistributed telangiectasia published in the literature are due to drugs of the dihydropyridine group (amlodipine, nifedipine, felodipine). Among these, amlodipine is the most common culprit.1,4,6 The review by Bakkour et al.4 described 8 cases (3 women and 5 men) between 33 and 85 years of age. The incidence is very low, although the condition is probably underdiagnosed.
Its etiologic and pathogenic mechanism has still not been elucidated. It has been suggested that sunlight may be an important constitutive factor in its appearance. The condition may be related to the vasodilator action of these drugs on vessels of the dermis or to the action of photoproducts and reactive oxygen species generated after the absorption of UV radiation, particularly UV-A, and visible light.1,4
Clinically, the reaction is characterized by the appearance of telangiectasias in sun-exposed areas such as the face, neckline, upper half of the back, and upper part of the arms. The lesions are usually asymptomatic and appear a few months after starting the treatment.1,4,6–9
The differential diagnosis must include other causes of telangiectasias, such as liver disease and hyperestrogenic states, autoimmune diseases such as scleroderma, dermatomyositis, and lupus erythematosus, and telangiectasia macularis eruptiva perstans.1 A detailed medical history and physical examination, and improvement of the manifestations on discontinuation of the implicated drug enable us to reach the diagnosis.
Treatment is based on withdrawal of the responsible drug. The prognosis is good, with improvement or disappearance of the lesions within a few weeks after discontinuing treatment.
In conclusion, telangiectasia is a common cause of consultation in dermatology. Photodistributed lesions associated with CCBs are a rarely reported side effect, and targeted questions about these drugs must therefore be included in the history. The clinical course after starting treatment with the drug is the key to diagnosis, and management consists of drug withdrawal. Dermatologists must be aware of this entity to avoid unnecessary investigations.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Mora ER, Sánchez DM, Hernández-Núñez A, Martínez JB. Telangiectasias fotodistribuidas asociadas a amlodipino. Actas Dermosifiliogr. 2017;108:76–77.