Leishmaniasis, a sandfly vector-borne protozoan infection, encompasses a wide spectrum of clinical presentations. The most common form of Leishmaniasis is cutaneous leishmaniasis.1 It affects primarily adults between the third and 5th decades of life and the lesions are commonly located on exposed body parts. The diverse clinical spectrum of CL depends upon various factors, such as the specific causative strain, geographic location, parasitic load and host immune response.
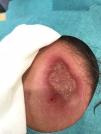
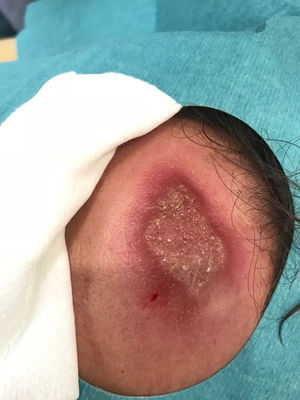
Case ReportA 31-year-old Portuguese male presented with a 4-month history of a solitary, asymptomatic, 4×2cm large, indurated crusty plaque on his forehead (Fig. 1). His medical history was unremarkable, except for early latent syphilis treated 1year ago with good serological response. His family history was unremarkable. He denied any prescribed or over-the-counter medication. His immunization status was up-to-date and his social and travel history were significant for a recent travel to Mexico about 5 months ago.
The skin biopsy revealed a dermal diffuse inflammatory infiltrate composed by lymphocytes and histiocytes. Leishmania amastigotes were identified in the cytoplasm of dermal macrophages.
The physical examination was otherwise normal. Otorhinolaryngologic endoscopy, bone marrow aspirate and abdominal ultrasound were performed to exclude mucous and visceral involvement; a basic blood panel, viral serologies including HIV and HCV disclosed no abnormalities.
Since it was a solitary lesion in a cosmetically-sensitive location, a combined treatment of intralesional meglumine antimoniate and topical photodynamic therapy was started. The protocol consisted of intralesional injection of 1mL of meglumine antimoniate per session followed by photodynamic therapy with topical methylaminolevulinate, a 3-h incubation period and red light irradiation (light emitting diode lamp (Aktilite®, 630nm, 37J/cm2) at weekly intervals on alternate weeks, in a total of 8 sessions. Side effects were minimal and included local erythema and a stinging sensation during the irradiation and immediately afterwards.
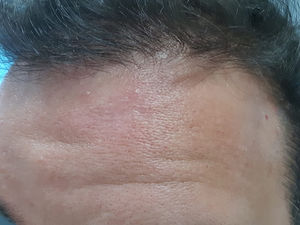
At the end of the treatment, the ulcer had given place to an atrophic scar with post-inflammatory hyperpigmentation (Fig. 2). Although the patient denied a confirmatory biopsy, at 12-month follow-up he remains in clinical remission, corroborated by dermatoscopic absence of vascular structures, yellow follicular "tears" or erythema, displaying only a white central atrophic scar, with resolution of peripheral hyperpigmentation.
DiscussionThe clinical presentation of cutaneous leishmaniasis consists of single or multiple, painless, frequently ulcerated, erythematous plaques with indurated borders, usually on exposed body regions.
The clinical diagnosis can be confirmed by the demonstration of amastigotes on skin biopsy specimens; by the growth of promastigotes in culture medium or molecular testing performed on skin biopsy samples. Dermatoscopy can be a valuable tool as an adjunctive diagnostic and follow-up non-invasive technique for in vivo observation of infectious lesions. In the particular case of cutaneous leishmaniasis, the most commonly described dermatoscopic signs are diffuse erythema and vascular structures; other features include hyperkeratosis, central erosion or ulceration, "yellow tears" and white starburst-like patterns.2
Although up to 50% of cutaneous leishmaniasis lesions are self-limited and self-healing, treatment is generally required in order to reduce the residual scar and to avoid further spread or transmission of the parasite.
In the particular case of cutaneous form, there are two possible therapeutic approaches, systemic or lesion-directed.
Systemic treatment including miltefosine, pentavalent antimonials, liposomal amphotericin B, pentamidine or azole derivatives is usually required when there are multiple (>3), large (>4cm) or lesions localized in cosmetically sensitive areas; when there is evidence of loco-regional spread (lymphangitis) or if the patient is immunosuppressed.3
There are several treatment options available for solitary lesions of cutaneous leishmaniasis, such as cryotherapy, topical paromomycin, intralesional antimony derivatives and photodynamic therapy.
Variables such as Leishmania species, the clinical presentation, host immunity status and the risk of extra-cutaneous involvement dictate the best treatment option.
Intralesional antimony derivatives are a safe and effective treatment and represent a viable alternative for patients with few or small lesions and contraindications to systemic treatment.4,9 It is usually well tolerated and possible side effects are scarring and transient hyperpigmentation. Conversely, the use of photodynamic therapy for the treatment of cutaneous leishmaniasis, is supported by various case reports and case series.6–8
The decision to combine both modalities was based on the attempt to minimise the pain associated with the procedure of intralesional administration since only 4 sessions were performed and the theoretical syngergistic effect of two differente mechanisms of action employed, namely, photodynamic therapy relying on systemic immune response and the antimonial derivative with direct parasiticidal effect.4 Since a total of 8 sessions would most likely result in lesion clearance using either one of the modalities in monotherapy, the lack of further comparative data imposes a substantial limitation to the rationale used in this study.
Although more robust studies are still needed in order to determine the real value of combined approaches vs monotherapy and the optimal treatment modalities, photodynamic therapy and intralesional antimonial derivatives represent convenient options in the setting of localized cutaneous infection in immunocompetent hosts especially in aesthetically sensitive areas.
ConclusionLocal therapy is desirable for patients with uncomplicated localized cutaneous leishmaniasis. We combined two locally-acting effective agents with good tolerability and low risk of side effects achieving a complete clinical response and a good cosmetic outcome.
Please cite this article as: Costin A, Bonito F, Alves J, Barreiros H. Tratamiento de la leishmaniasis localizada mediante el antimoniato de meglumina intralesional y la terapia fotodinámica. Actas Dermosifiliogr. 2020;111:897–899.