Drug rash with eosinophilia and systemic symptoms (DRESS) syndrome, also known as drug-induced hypersensitivity syndrome, is an uncommon severe reaction with a late onset and prolonged course that is sometimes fatal (10%-40%). The pathogenesis of this condition is complex, and various factors are believed to interact, including accumulation of drug metabolites, HLA-associated predisposition, drug-virus interactions, alternating cycles of immunosuppression and immune recovery, and the presence of drug-specific T lymphocytes.1 DRESS syndrome is a type IV hypersensitivity reaction that is mediated by type 2 helper T cells.2
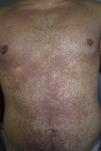
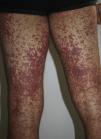
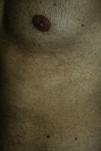
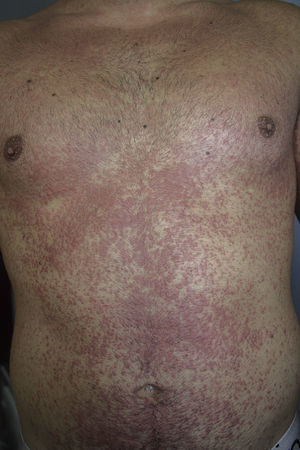
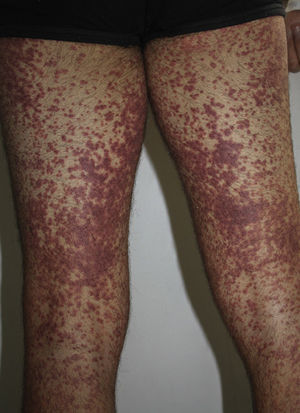
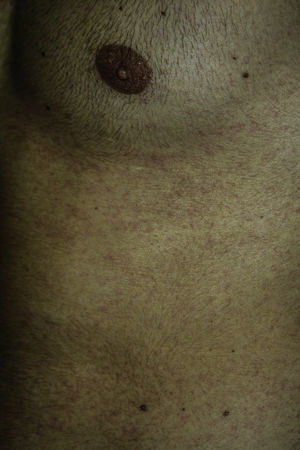
We report the case of a 24-year-old man who attended the emergency department with a 2 to 3–day history of generalized erythematous maculopapular rash (Figs. 1 and 2), fever >39°C, and painful enlarged lymph nodes (>2cm) on both sides of his neck. The mucosa was not involved. The patient had a personal history of asthma, anxiety, and chronic prostatitis and had been receiving montelukast, inhaled salmeterol/fluticasone, and bromazepam for more than a year. In addition to his usual treatment, he had received trimethoprim-sulfamethoxazole during the previous month. The blood workup revealed leukocytosis of up to 21 300cells/μL with 25% eosinophils and acute hepatitis (aspartate aminotransferase, 91U/L; alanine aminotransferase, 599U/L; and γ-glutamyl transpeptidase, 248U/L); the remaining values were within the normal range. The results of serology testing for hepatotropic viruses were negative. Abdominal ultrasound examination revealed moderate splenomegaly. Chest x-ray and electrocardiogram findings were normal. The skin biopsy revealed spongiosis, lymphatic exocytosis, and necrotic keratinocytes in the epidermis, together with a perivascular mononuclear infiltrate in the dermis. The patient was diagnosed with DRESS syndrome, his previous treatment was stopped, and he was prescribed oral prednisone. Given the persistence of the cutaneous lesions and altered laboratory values despite systemic therapy with corticosteroids, treatment with oral ciclosporin was prescribed for 4 months, until symptoms resolved completely. One month after treatment was suspended, the patient underwent patch testing with the standard series of the Spanish Contact Dermatitis and Skin Allergy Research Group, trimethoprim 2% in dimethyl sulfoxide, and sulfamethoxazole 2% in petrolatum. The results were positive for methylchloroisothiazolinone/methylisothiazolinone (no relevance); the results for the remaining allergens were negative at 48 and 96hours and at 7 days. On the eighth day after the patch tests, the patient developed a generalized maculopapular rash on the trunk that was clinically and histologically similar to the previous rash, although less intense (Fig. 3). The rash was interpreted as a reactivation of the rash induced by the patch tests. The lesions resolved completely with oral prednisone. The patient was advised to avoid trimethoprim-sulfamethoxazole and has remained asymptomatic.
Patch testing is considered a useful diagnostic tool in the study of adverse drug reactions,1 especially those caused by type IV hypersensitivity mechanisms. Although positive results are observed with greater frequency in drug-induced maculopapular rash, generalized exanthematic pustulosis, and fixed drug eruptions, patch testing has also been used in the assessment of other types of reaction, even in more severe reactions.2 The technique is simple and relatively harmless for the patient. The risk of triggering a severe reaction with patch tests is low compared with the risk of a reaction with intradermal testing. Although reactivation of cutaneous lesions can occur, it is considered an uncommon finding.3–5 Patch testing after evaluation of the risk-benefit ratio is even recommended in severe drug hypersensitivity reactions, including DRESS syndrome, toxic epidermal necrolysis, and Steven-Johnson syndrome.6
The sensitivity of patch testing in the assessment of DRESS syndrome varies depending on the culprit drug and is greater with anticonvulsant agents, especially carbamazepine. In the case of other drugs involved in the syndrome, the sensitivity of patch testing is considered low.2,6
Despite its limited sensitivity, patch testing is an appropriate way of assessing drug-induced reactions before performing prick tests, intradermal tests, and even drug challenge tests, which carry greater risks for the patient.
We present a case of DRESS syndrome caused by trimethoprim-sulfamethoxazole. The patient developed a reactivation of the skin lesions induced by patch tests. The low concentration of drug in the patches, the poor availability of tests, or the fact that the reaction was triggered by a metabolite and not by the drug itself could explain the negative result in the patch tests. Nevertheless, percutaneous absorption from the patches was sufficient to cause a generalized reaction.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Córdoba S, Navarro-Vidal B, Martínez-Morán C, Borbujo J. Reactivación de las lesiones cutáneas por pruebas epicutáneas en el estudio de un síndrome de DRESS. Actas Dermosifiliogr. 2016;107:781–783.