Chronic radiodermatitis is defined as a chronic inflammation of the skin associated with exposure to ionizing radiation. It usually presents in individuals who, because of their profession, have been repeatedly exposed to low doses of radiation over a long period of time without appropriate protection.
Several treatments have been described, including topical 5-fluorouracil, dermabrasion, ablative laser, photodynamic therapy, and surgery.1 In 2006 Sachse et al. described the use of imiquimod in a 60-year-old patient with chronic thoracic radiodermatitis.2
We report the case of a 69-year-old male radiologist referred to our clinic for assessment of skin lesions that had appeared 2 years earlier on the dorsum of the fingers of both hands. The patient had performed fluoroscopy in clinical practice for 25 years without wearing gloves or using other recommended protective measures.
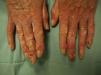
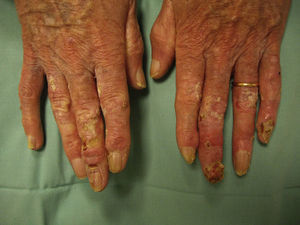
Physical examination revealed skin atrophy, poikiloderma, loss of skin adnexa, ulcerations, and hyperkeratotic lesions on the dorsum of several fingers of both hands with nail involvement (Fig. 1).
Several of the lesions were biopsied. Histologic findings in the specimen taken from the third finger of the left hand were compatible with actinic keratosis, and the changes observed in the specimen taken from the third finger of the right hand were conclusive for squamous cell carcinoma.
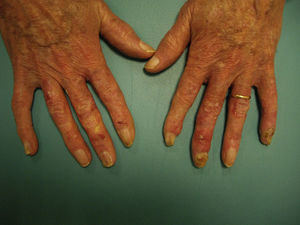
After informing the patient of the treatment options, a 4-week cycle of imiquimod cream, 5% was prescribed to reduce the number of lesions, with application 3 times a week. Tolerance was good and the number of lesions had decreased significantly by the end of the cycle (Fig. 2). Because the lesion on the third finger of his left hand persisted, the patient was referred to the traumatology department, where the distal phalanx of the affected finger was amputated.
Imiquimod (Aldara) is an immune response modulator belonging to the family of imidazoquinolines. Topical imiquimod stimulates the innate and acquired immune responses.3 By binding to toll-like receptor 7, this drug activates immune cells, inducing the secretion of numerous cytokines with a potential antitumor effect, such as interferon α, tumor necrosis factor α, and interleukin 12.4 In vitro studies have shown that, in addition to its antitumor activity, imiquimod also has anti-inflammatory, proapoptotic, and antiangiogenic properties.5
Topical imiquimod has been approved for the treatment of actinic keratosis, some subtypes of basal cell carcinoma, and papillomavirus infections.6 However, in clinical practice it has been reported to be effective in Bowen disease, in situ squamous cell carcinoma, lentigo maligna, Kaposi sarcoma, skin metastases of melanoma, and keloids of the ear.7–10 Recently, Sachse et al. reported the efficacy of imiquimod in a patient with chronic radiodermatitis.2
Chronic radiodermatitis, a chronic inflammation of the skin associated with exposure to ionizing radiation, is most common in patients who have not used the recommended protection measures. The progression and degree of chronic radiodermatitis is determined by the quality and intensity of the radiation. Generally, a dose higher than 12 to 15Gy will cause chronic radiodermatitis2 but repeated exposure to lower doses may also produce lesions of this type.
The first clinical sign of radiodermatitis is skin atrophy: the skin becomes thin, dry, and often hyperkeratotic. Partial or complete loss of skin adnexa may also be observed. However, the most serious problem of chronic exposure to ionizing radiation is the development of precancerous lesions and skin cancers such as squamous cell carcinoma.
Several types of treatment have been described, including topical 5-fluorouracil, dermabrasion, ablative laser therapy, photodynamic therapy, surgery, and topical imiquimod.1,2 Because of the nature of the site, the treatment of the dorsal surfaces of the hands may be problematic. Imiquimod may therefore offer a good alternative for treating or reducing the number of lesions prior to other treatments because it is easy to apply, is well tolerated by patients, and has few adverse effects. In conclusion, we present the case of a patient with chronic radiodermatitis on the dorsum of both hands which responded well to treatment with topical imiquimod.
Please cite this article as: López V, et al. Eficacia de imiquimod tópico al 5% en paciente con radiodermitis crónica en las manos. Actas Dermosifiliogr. 2012;103:441-2.