In daily clinical practice, the dermatologic surgeon frequently has to excise closely adjacent tumors in the facial region. In such cases, planning of an appropriate reconstruction technique is essential. The aim is to treat all of the lesions in a single surgical intervention, if possible, and to achieve a good functional and cosmetic outcome. We present 5 patients in whom a single flap was used to repair multiple adjacent defects.
En la práctica diaria, es frecuente que el cirujano dermatológico deba extirpar varias lesiones tumorales próximas entre sí en la región facial. Para ello, es importante planificar una técnica reconstructiva adecuada que permita, si es posible, abordar las lesiones en un solo acto quirúrgico, proporcionando buenos resultados funcionales y estéticos. A continuación se presentan 5 casos de pacientes en los que se ha empleado un único colgajo para realizar el cierre de varios defectos próximos.
The incidence of skin cancer is increasing progressively, due mainly to lifestyle changes, greater exposure to sunlight, and a considerable increase in life expectancy.1 A study of nonmelanoma skin cancer in Spain, performed between 1978 and 2002, reported a progressive increase in both sexes, with an almost 3-fold increase in incidence by the end of the study period.2 As the face and scalp are the main areas exposed to the sun, the simultaneous detection of 2 or more adjacent lesions is not uncommon. Although the design for the reconstruction of 2 adjacent defects can sometimes be complicated by the situation of 1 of the lesions within the area of skin potentially useful for reconstruction of the other, the inclusion of the 2 defects in a single-flap design can be an effective solution. We present a series of cases in which we applied this concept to the reconstruction of defects left by the excision of 2 or more adjacent tumors.
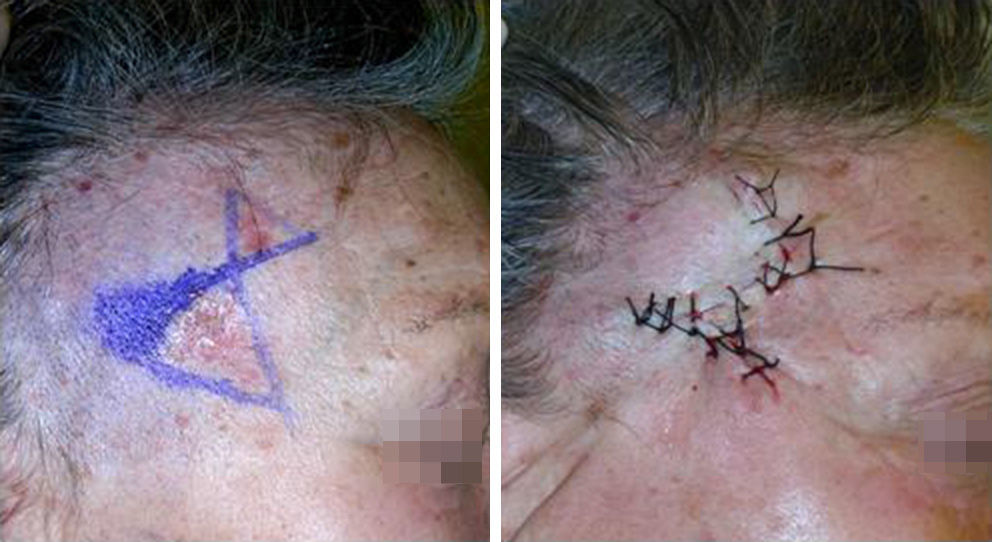
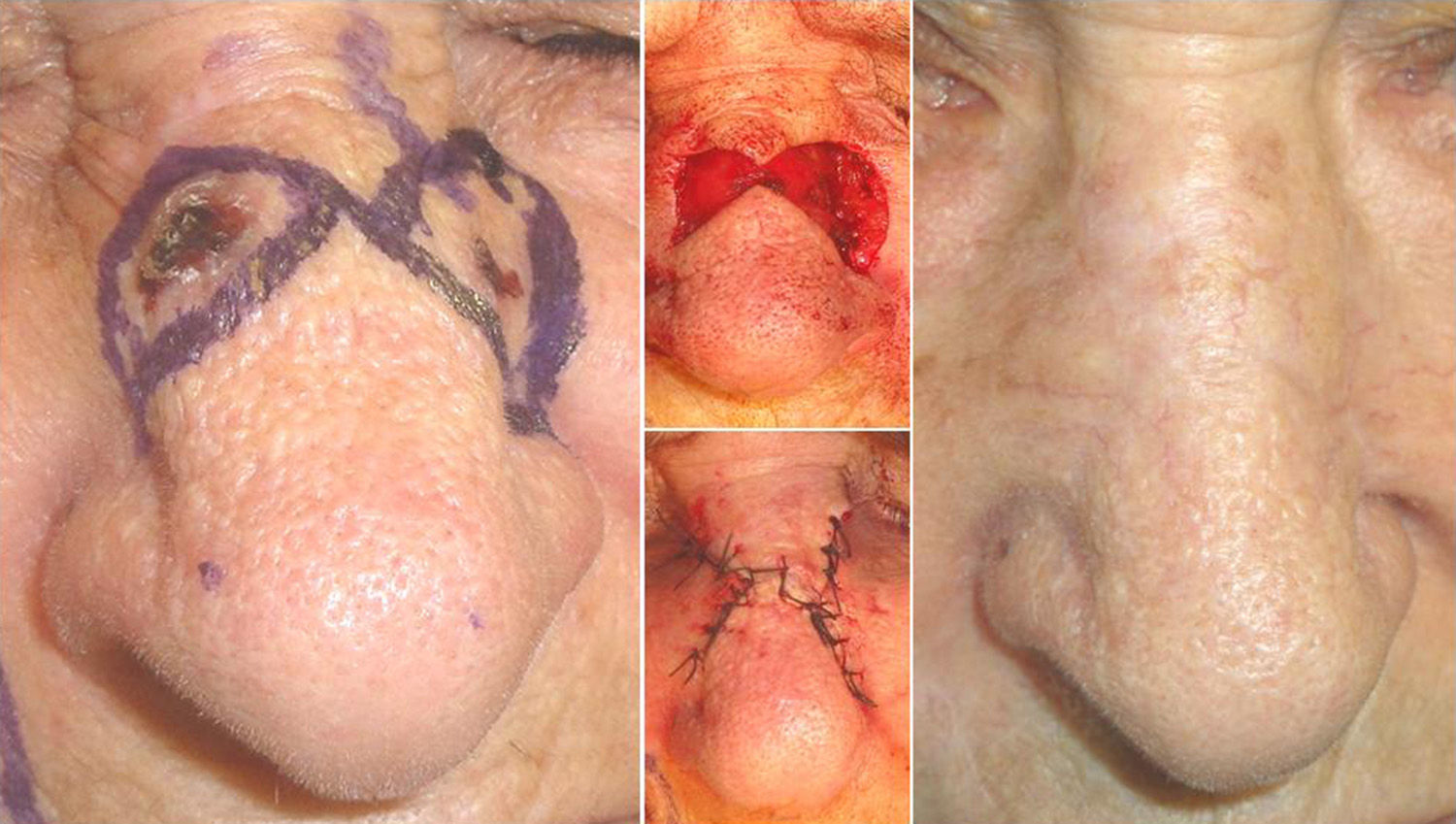
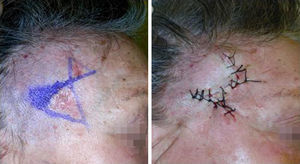
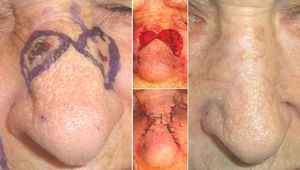
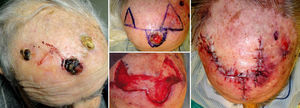
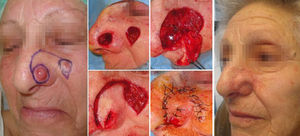
Case DescriptionsPatients 1 and 2 were aged respectively 67 and 74 years. They each had histologically diagnosed adjacent basal cell carcinomas. The lesions were in the right temporal region in the first patient (Fig. 1) and on the dorsum of the nose in the second (Fig. 2). One of the lesions was excised by conventional surgery, with a safety margin, excising a triangle of skin, and a Burow triangle advancement flap was designed for reconstruction. An incision was made to extend the base of the triangle created by the defect of the first tumor towards the second tumor. At the end of this incision, a Burow triangle was created in the opposite direction to the primary defect; this Burow triangle included the second tumor.3 Satisfactory functional and cosmetic results were achieved in both cases.
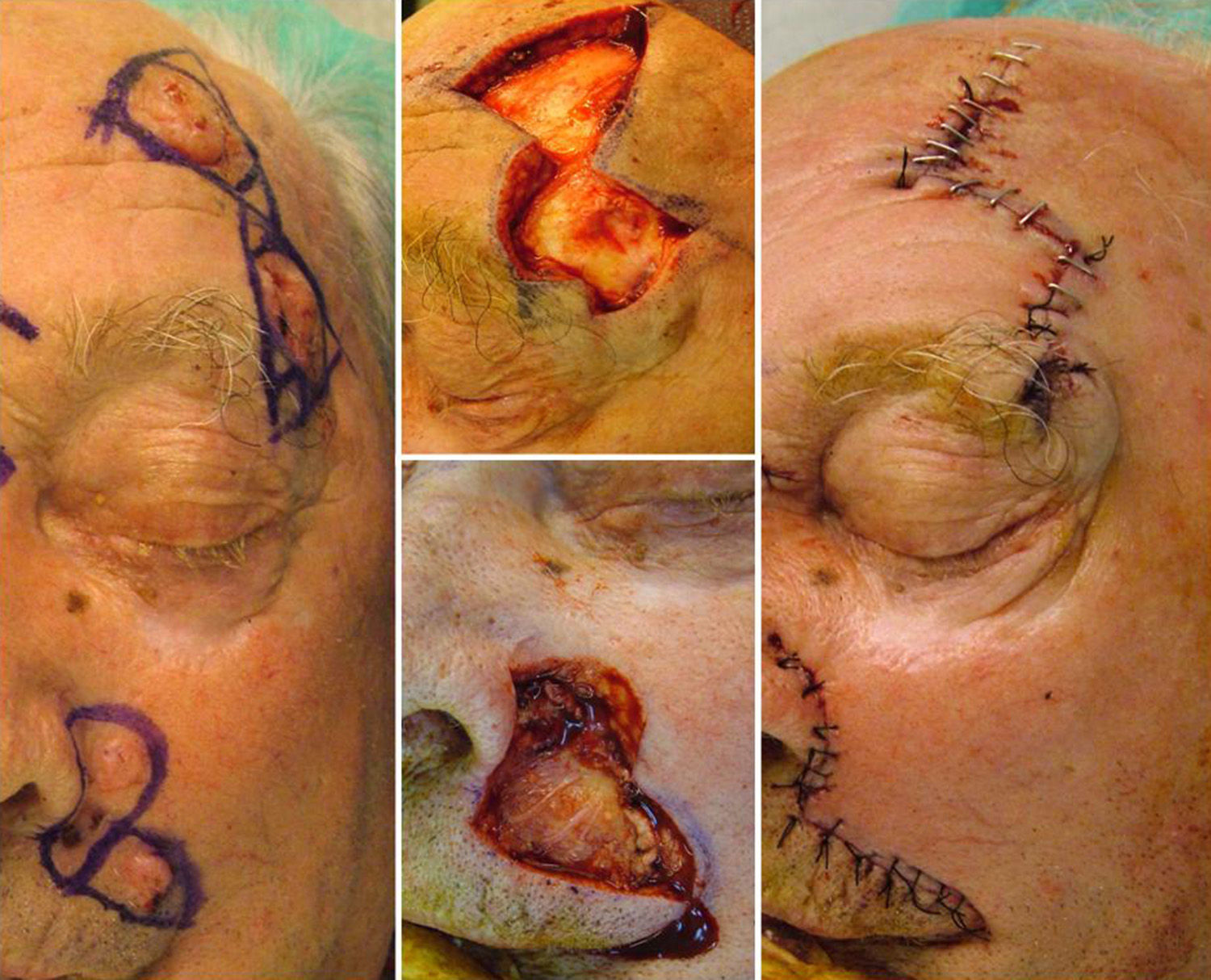
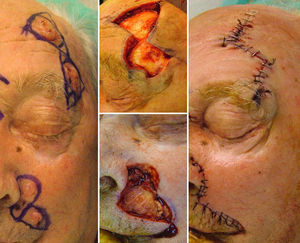
The third case was a 93-year-old man with multiple facial tumors, 2 of which were located in the left frontal region. These lesions were excised by conventional surgery with a margin of 0.5cm. The same technique was used as in cases 1 and 2, with the design of a unilateral triangular advancement flap, with the second tumor included in the Burow triangle (Fig. 3). This patient presented a further 3 basal cell carcinomas on the upper lip and in the left alar fold. The central tumor, situated on the superior border of the nasolabial fold, was excised using a circular incision, and closure of the defect was designed using a crescentic perialar advancement flap. In this case, the superior and inferior crescents included the 2 adjacent tumors, and their excision made flap advancement possible. The superior crescent was created in the alar sulcus, and the inferior one along the nasolabial fold. The concept is similar to the Burow triangle. Finally, the skin of the cheek was liberated until sufficient advancement was achieved to close the defect.
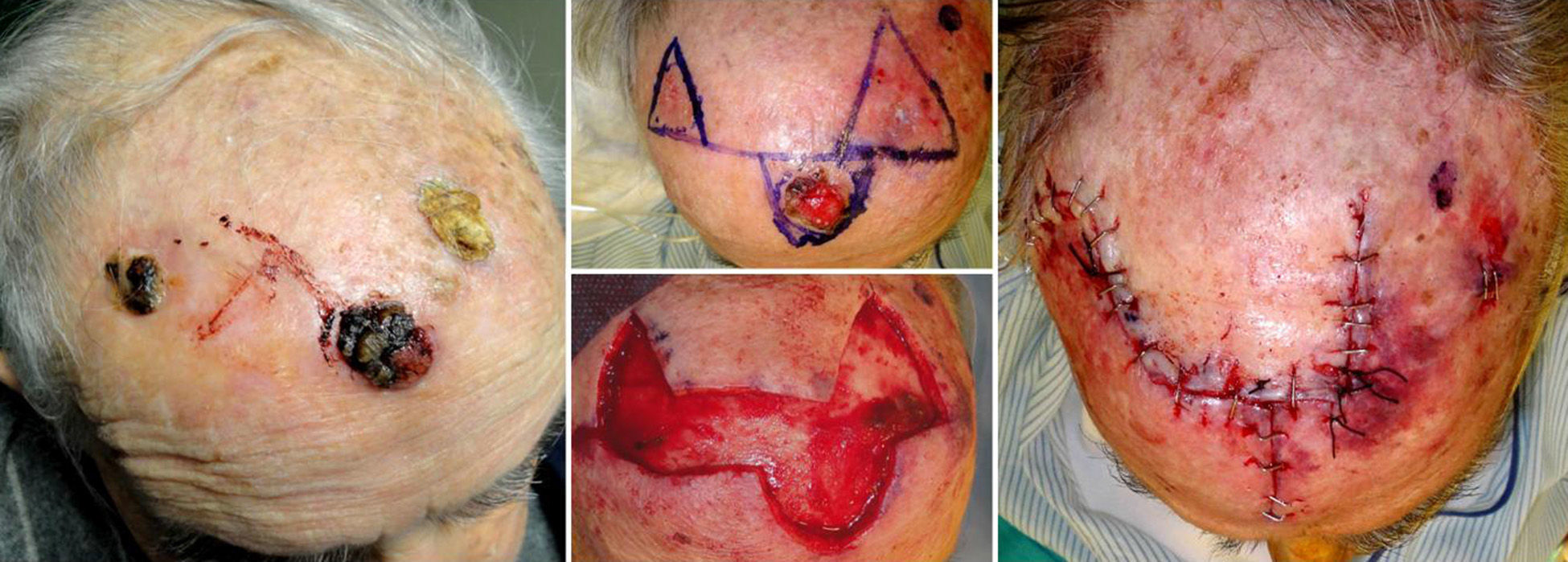
The fourth case was a man aged 85 years with a clinical diagnosis of 3 squamous cell carcinomas on the scalp. The 3 tumors could be excised using a single A-T advancement flap formed by 2 Burow triangle advancement flaps (Fig. 4).
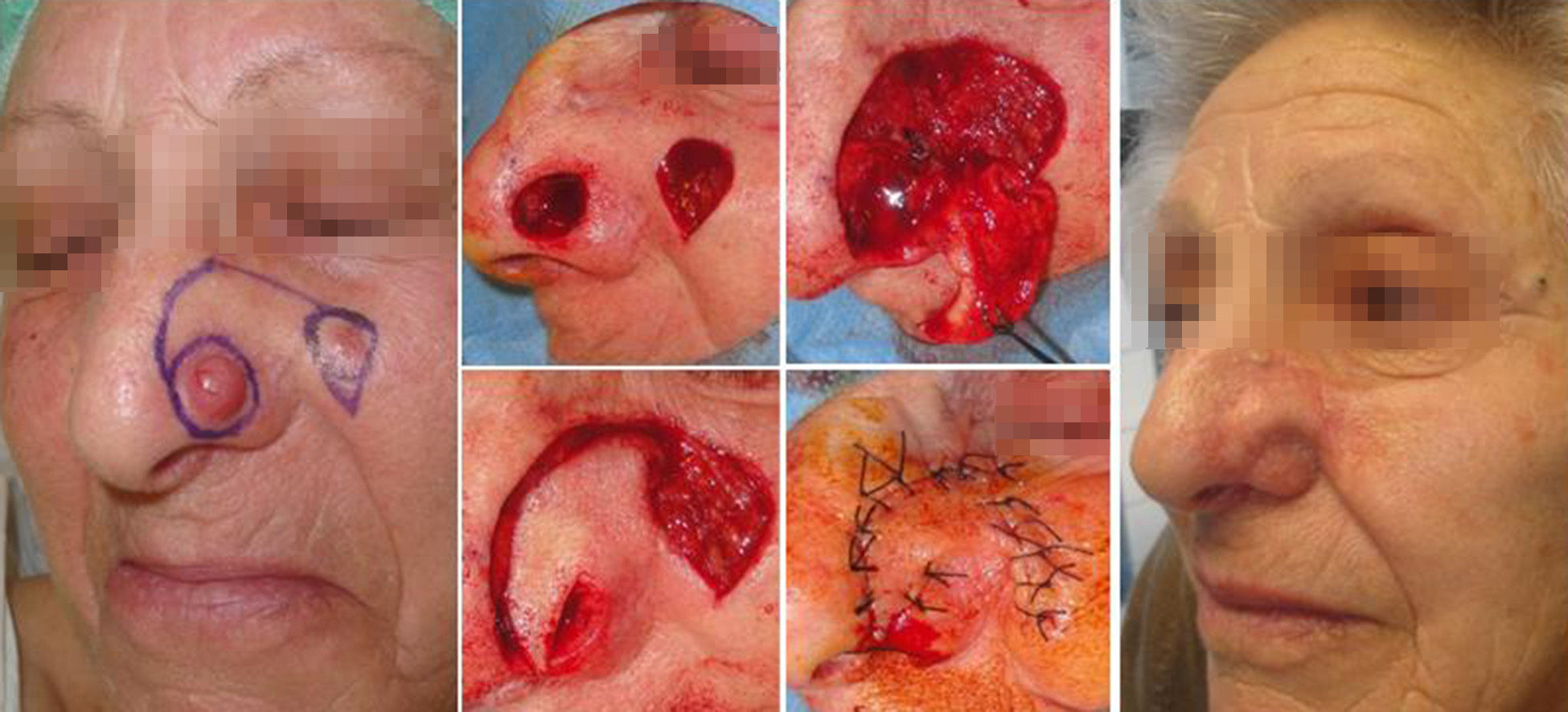
The final case was an 83-year-old woman who presented 2 basal cell carcinomas, 1 at the union of the tip of the nose with the left nasal ala and other on the left cheek (Fig. 5). It was decided to use conventional surgery for combined excision of the carcinomas using a hatchet flap design with a modified distal section. The lesion at the union of the tip of the nose with the nasal ala was excised using a circular incision. A line was then drawn in an arc towards the site of the other tumor on the left cheek, but instead of performing the radial incision of a hatchet flap, we excised a triangle that included the second tumor. The cosmetic and functional results were satisfactory, with no recurrence during 5 years of follow-up.
DiscussionWhen 2 or more adjacent tumors are excised, the defect can often be sutured directly. But if the defects are large, closure can become problematic due to tension in the tissue between the defects. Additionally, the position of 1 of the tumors can interfere with the design of the flap to close the defect left by the other tumor. A good surgical strategy is therefore to plan excision of the 2 tumors to coincide with the design of a single flap.4
The Burow triangle advancement flap is simple to perform and can be readily adapted to each patient's need, depending on the size and shape of the lesions and on the tension in the adjacent skin.5,6 These factors will determine the length of the advancement flaps and the size of the Burow triangle.7 If the tumors are very close, the length should be equal to that of the defect; but if there is greater separation, the triangle can be smaller, depending on tissue elasticity and mobility.8 It is important to orient the incision and suture lines to camouflage the scars in anatomic folds, in skin creases, or following the tension lines of the relaxed skin.9
The perialar crescentic advancement flap requires a crescent to be drawn in the nasolabial fold so that the concave part is in contact with the perialar sulcus. After excision of the crescent and release of the tissues, the flap is moved superiorly to close the primary defect and thus achieve adequate overall closure.10 In the case presented, in which 2 crescents were used, 1 inferior and 1 superior, each crescent took on a role similar to that of a Burow triangle in order to include the adjacent tumors.
Three adjacent tumors may sometimes be found. In this situation, a simple and ingenious surgical option is to treat all 3 in a single operation using a bilateral Burow triangle advancement flap to create the variant known as the A-T advancement flap.3,4 The advantage of this flap is that it allows a large amount of tissue to be moved to close large defects; it is the flap of choice in junctional facial areas, as the longest scar can be concealed above the hairline or in natural facial folds.4 In addition, in this type of flap, as occurs with the unilateral Burow triangle advancement flap, the size of the lateral triangles that include the other tumors can be adjusted to the dimensions necessary for closure; the triangles do not have to be the same size.
The hatchet flap is a mixed rotation advancement flap that allows very considerable tissue movement. Its design is similar to that of a simple rotation flap, but with a distal incision.11 In the case presented, a modification was introduced to this incision, creating a triangle that included the second lesion,6 reducing the pedicle without risk to the blood supply to the flap, achieved in this case by including the angular artery in the pedicle.
ConclusionWith a single, well-designed flap, using advancement or rotation, complex cases of multiple skin tumors can be resolved in a single operation. In the Burow triangle advancement flaps, the tension-releasing triangle is designed to include the site of 1 of the tumors. The surgical technique for these flaps is relatively simple and has major advantages for closure of the defect, including a reduction in tissue tension, decreasing the risk of necrosis and of scar dehiscence while also offering an excellent cosmetic result. Furthermore, as we have demonstrated, the technique allows for considerable variation in its design, depending on each patient's individual needs.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this research.
Confidentiality of dataThe authors declare that they followed their hospital's regulations regarding the publication of patient information.
Right to privacy and informed consentThe authors obtained informed consent from the patients and/or subjects referred to in this article. This document is held by the corresponding author.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Suárez-Valladares MJ, Pérez-Bustillo A, González-Sixto B, Otero-Rivas M, Rodríguez-Prieto MA. Colgajos cutáneos para la resolución de múltiples tumores próximos adyacentes. Actas Dermosifiliogr. 2016;107:e7–e11.