A 3-month-old boy was seen for an exudative lesion in the anterior cervical region that had been present since birth. The gestation period had been normal and the child had been born at full term. The patient had no other medical or surgical history of interest.
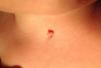
Physical ExaminationPhysical examination revealed a skin-colored pedunculated papule on the anterior midline of the neck. At the caudal end of the lesion, there was an orifice that connected to a small mucosal fistula measuring barely 2mm in length (Fig. 1). The lesion was not adhered to deeper tissues and showed no mobility when the patient swallowed or moved his tongue. A catheter was inserted into the orifice and reached a dead end after penetrating about 3-4mm.
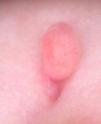
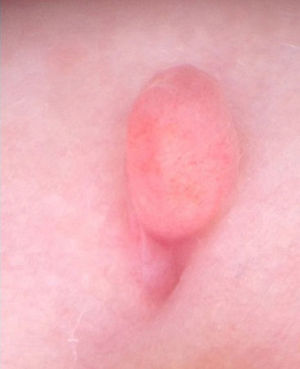
Additional TestsDermoscopic examination revealed a pink pedunculated papule measuring 0.3cm in diameter, at the inferior end of which was a fissure (barely visible to the naked eye) measuring 0.1cm with a mild transparent exudate (Fig. 2). Soft-tissue ultrasound examination revealed a round, well-defined hypoechoic superficial lesion that showed no evidence of a fistulous tract as well as a thyroid with a typical morphology and location. Complete blood count, biochemistry, and hormone panel were normal. An electrocardiogram (ECG) was carried out as a first step to rule out cardiac abnormalities.
What Is Your Diagnosis?
DiagnosisMidline cervical cleft (MCC).
Clinical CourseThe patient was assessed by the pediatric surgery department and an initial attitude of watchful waiting was adopted. Curative surgical treatment will be scheduled for when the boy is around 1 year of age.
CommentMCC is a rare congenital anomaly that causes a visible defect at the midline of the neck. Around 200 cases have been described in the international literature,1 mostly in plastic surgery or otorhinolaryngology journals. MCC appears sporadically and is slightly more common in girls.1,2 The clinical presentation is characterized by a linear vertical deepithelized plaque with a fibroepithelial papule at the cranial end that extends towards the caudal end, terminating in a blind sinus.1,2 The entity has no relationship to the thyroid or to the hyoid bone.3 The lesion is generally limited to the skin, but there have been cases in which it extends to the subcutaneous tissue and underlying muscle.2,3 The size of the lesion can be highly variable and it can be located anywhere along the anterior midline from the lower lip to the suprasternal region.2 The condition is generally detected at birth, but mild forms can go undetected or can be mistaken for remnants of the thyroglossal duct or branchial anomalies.1 The differential diagnosis should include fistulas, sinus cysts of branchial origin, and bronchogenic cysts.1,2 Branchial disease typically appears in the region anterior to the sternocleidomastoid muscle, and bronchogenic cysts tend to be located in the suprasternal notch.2,4 In case of doubt, ultrasound and computed tomography can be very useful in establishing a diagnosis.
The embryopathogenesis of MCC is not yet fully understood, and most authors consider it to be a mild form on the spectrum of congenital branchial anomalies.1,2,5 This would explain the occasional association of MCC with other anomalies such as thyroglossal duct cysts, dermoid cysts, bronchogenic cysts, cleft lip, and congenital cardiac anomalies.1,6 A full hormone panel and an ECG are also recommended as a first step to rule out associated comorbidities.
The clinical course of MCC is benign with spontaneous scarring and the formation of a fibrous cord.1,5,6 However, because there is considerable risk of infection, cervical contracture, and limitation of mobility, MCC should be managed with surgery around the age of 1 year and no later than 2 years.2,3 The preferred technique is complete excision followed by Z-plasty closure4–6 to prevent the recurrence of fibrosis, which can occur following direct closure.4 Finally, periodic follow-up of the patient throughout infancy is recommended because of the risk of retraction and hypertrophic scarring.4,6
In conclusion, we have described a case of mild MCC in which the typical atrophic plaque was not evident and the diagnosis was supported by physical examination, dermoscopy, and ultrasound. Other congenital anomalies are rarely associated with MCC and should be ruled out during the diagnostic process. Treatment of the condition should be mainly surgical.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Arjona-Aguilera C, Blasco-Morente G, Tercedor-Sánchez J. Pápula pediculada y fisura en línea cervical anterior de recién nacido. Actas Dermosifiliogr. 2016;107:681–682.