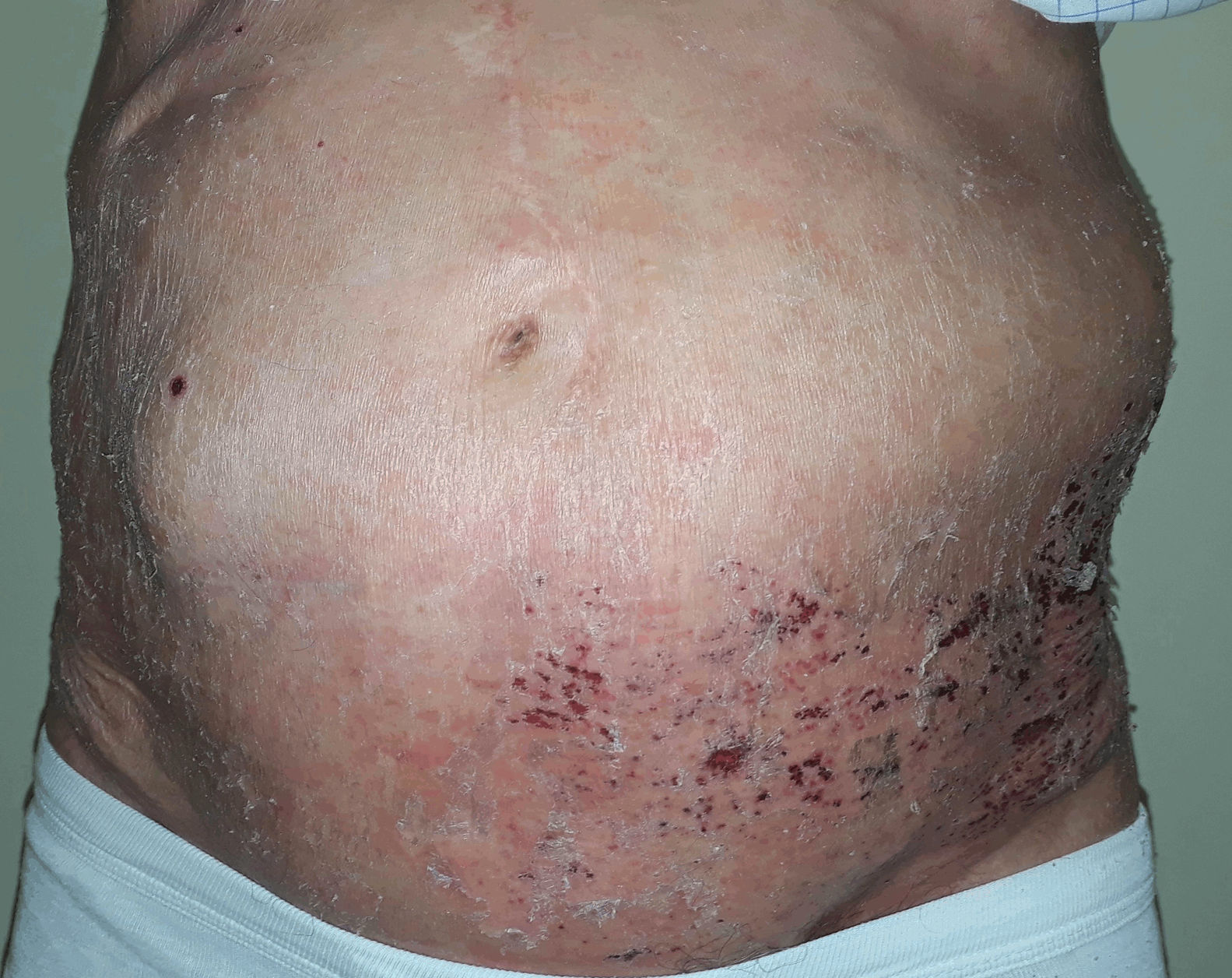
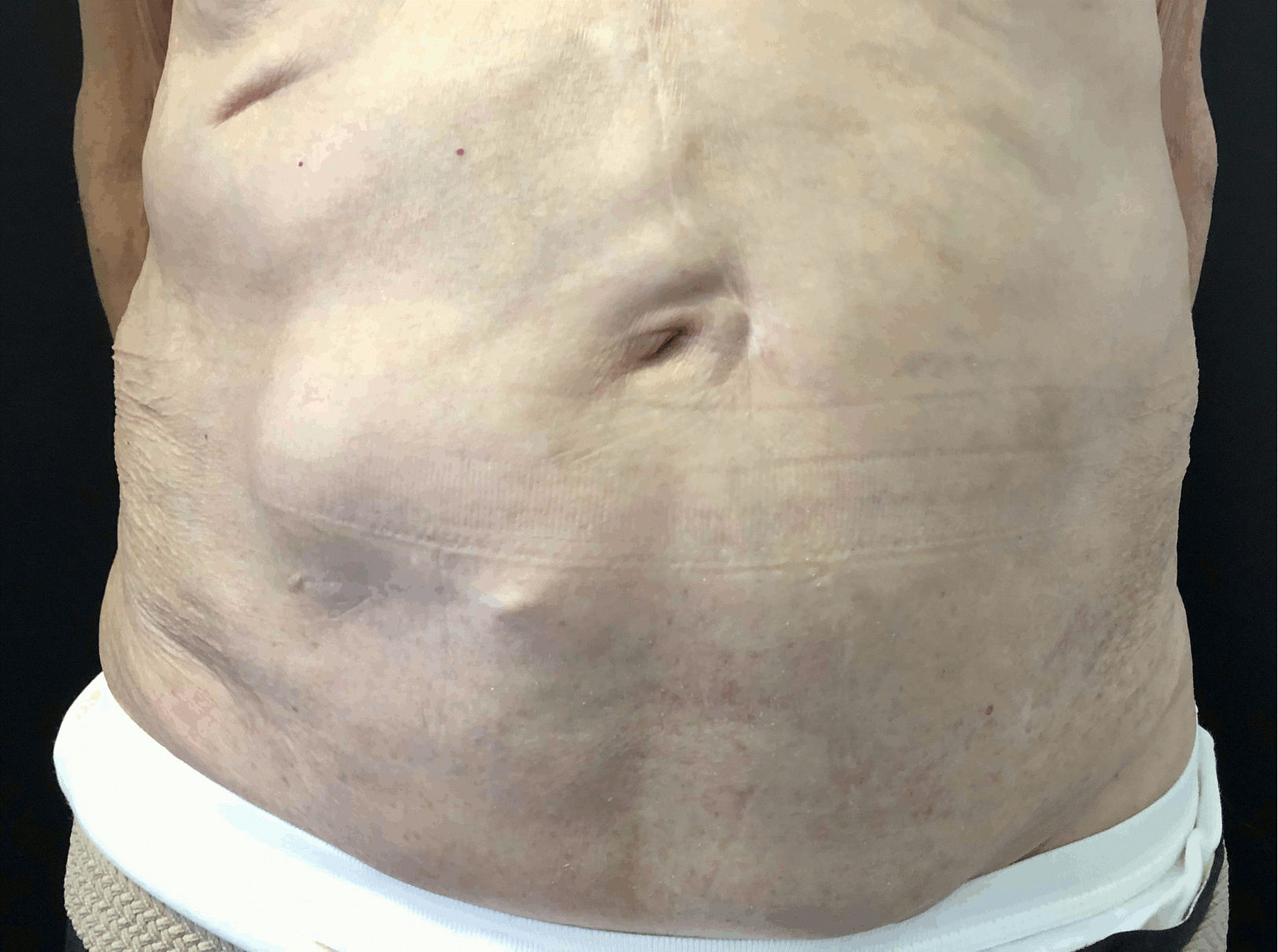
After attending the emergency department of another hospital, an 84-year-old man was diagnosed with left abdominal herpes zoster (HZ). Because clinical signs had developed more than 72 hours earlier, no antiviral treatments were administered. One week later, the patient came to our outpatients due to the sudden appearance of an asymptomatic mass in the area affected by HZ. Five years earlier he had developed a rectal neoplasm that was treated with surgery and radiation therapy. Physical examination revealed hyperesthesia and lesions in the crusting phase on dermatomes T10 to T12. Painless, reducible bulging of the abdominal wall that increased with Valsalva maneuvers was evident in the area affected by HZ (Fig. 1). A midline laparotomy scar showed no signs of complication. An abdominal computed tomography scan was requested to rule out abdominal mass or hernia. The results revealed thinning of the abdominal wall without evidence of hernia. An electroneuromyographic study revealed no alterations. Given the temporal relationship between the appearance of the rash and the protrusion, the case was oriented as abdominal pseudohernia due to HZ. After 8 months, the patient showed a complete clinical recovery (Fig. 2).
While sensory alterations are one of the main neurological complications of HZ, motor nerves can also be affected, resulting in paralysis of the facial muscles, extremities, diaphragm, or abdominal muscles, in some cases with visceral involvement.1
Abdominal pseudohernia is a protrusion limited to the abdominal wall without an actual underlying defect. The first case of paralysis of the abdominal musculature caused by HZ was described in 1886 by Broadbent.2 Despite the high incidence of HZ, this entity is only observed in between 0% and 2% of cases.3 It manifests as abdominal distention with unilateral bulging on the affected side. The T11 dermatome is the most affected, followed by T12 and T10.4 Symptoms can appear 2 to 6 weeks before the rash, but usually develop about 2 weeks after.3 It has been predominantly described in elderly patients and those with hematologic neoplasms, as well as immunocompromised individuals.5
The exact underlying mechanism is not entirely clear, but it is thought to involve viral infection at the level of the anterior horn of the spinal cord as a consequence of neural spread of the varicella-zoster virus from the dorsal root ganglia.6 Pathological studies3,7 have demonstrated ganglion lesions combined with degeneration of the sensory and motor roots together with severe neuritis, which may explain the electrophysiological findings characteristic of the disease.
Diagnosis is primarily clinical, based on temporal correlation of HZ with the appearance of abdominal distension. Physical examination may reveal decreased or absent segmental reflexes.5 An electroneuromyographic study can be useful to confirm diagnosis, although alterations are observed in only 35%3,8 of cases. Abdominal computed tomography shows a thinned abdominal wall and rules out the presence of an abdominal mass or hernia. Gadolinium-diethylenetriamine penta-acetic acid (DTPA) nuclear magnetic resonance imaging can help define the extent of inflammation and exclude compression of the spinal nerve roots.9
The differential diagnosis should include diseases that present with alterations in the innervation of the abdominal wall musculature and can cause pseudohernia, such as lumbar hernia, polyradiculoneuropathy, diabetic neuropathy, and syringomyelia.
Treatment is the same as for HZ, with antiviral drugs and analgesia if required. Short courses of corticosteroids8 have also been used for their anti-inflammatory effects, as well as multiple vitamin preparations,3,7 which can help restore damaged nerve fibers, although there is little evidence to support the use of these treatments.
The prognosis for motor weakness is usually good, with complete or near complete recovery in 55% to 75%10 of cases within a period of 2 to 18 months.3 The most common complication of pseudohernia is constipation,4 although other complications, including paralytic ileus and voiding disorders,1 have been described in 19.4%4 of patients.
In conclusion, abdominal pseudohernia is a rare complication of HZ that usually has a good prognosis. Although the suspected diagnosis is clinical, it is advisable to perform a noninvasive imaging test to rule out a true hernia.
Conflicts of interestThe authors declare no conflict of interest.
Please cite this article as: Setó-Torrent N, Iglesias-Sancho M, Arandes-Marcocci J, Salleras Redonnet M. Pseudohernia abdominal por herpes zóster. Actas Dermosifiliogr. 2020. https://doi.org/10.1016/j.ad.2019.01.029