Decompression sickness is a clinical condition characterized by the formation of bubbles of inert gas in different parts of the body; these bubbles are caused by changes to the solubility of gases triggered by pressure changes during a dive.1
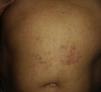
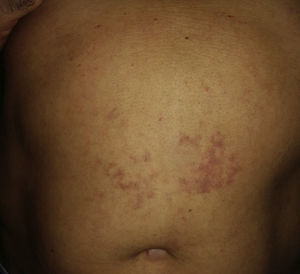
We report the case of a 55-year-old man with no personal or family history of interest who presented with a slightly pruritic rash that had appeared several hours after a recreational dive. The examination revealed a purpuric-violaceous macular rash on the trunk that was more pronounced in the supine decubitus position (Fig. 1). No rales could be heard in the affected area. Cutaneous ultrasound of the area showed no significant findings in the dermis or hypodermis. With a suspected diagnosis of decompression sickness, the patient underwent an echocardiogram, which revealed a patent foramen ovale measuring 9mm in diameter; this defect is one of the predisposing factors for decompression sickness. In view of the ultrasound findings and the absence of other symptoms or significant findings in the patient's history, a diagnosis of mild decompression sickness was established. As the patient was otherwise asymptomatic, refused to undergo further tests, and showed progressive clinical improvement, we decided not to perform a skin biopsy and to administer symptomatic treatment and take a watch-and-wait approach. At the time of writing, 2 weeks after the diagnosis, the patient is free of symptoms.
Decompression sickness is caused by an increase in ambient pressure during submersion that causes an increase in the partial pressure of inhaled gases (Dalton's Law). This increase, in turn, gives rise to a pressure gradient that results in the accumulation of gases, and nitrogen in particular, that remain dissolved in the body.1 When the diver returns to the surface, the pressure gradient is reversed, causing oversaturation with gases. Above a certain level, this oversaturation gives rise to the formation of bubbles in different parts of the body. The bubbles trigger a series of responses, such as increased platelet aggregation, capillary permeability and vasoconstriction, that complicate the elimination of gas even further. Predisposing factors to decompression sickness include intense physical activity before, during, or after the dive; diving in cold water (vasoconstriction); associated malformations, in particular patent foramen ovale,2 which may be asymptomatically present in up to 40% of the population (as it was in our patient); abnormal arteriovenous communications or other cardiocirculatory alterations; successive dives of between 10minutes and 12hours after the first dive; obesity due to increased solubility of nitrogen in adipose tissue; hypobaric exposure after diving; female sex; and repetitive dives in a short period of time.
There are 2 clinical variants of decompression sickness. The first variant, type 1, is the least serious type and is characterized by cutaneous involvement in the form of a purpuric macular-papular rash (which needs to be distinguished from an allergic reaction), joint pain, or edema. Type 2 is a more severe variant characterized by neurological, respiratory, and/or cardiocirculatory involvement. Rapid diagnosis and treatment is essential as it can considerably reduce the risk of complications and death.1,3–6
In more severe cases, basic care consists of treatment in a hyperbaric chamber with delivery of 100% oxygen. Institution of hyperbaric oxygen therapy should not delay the performance of complementary tests (complete blood count, full biochemistry, gasometry, electrocardiogram, chest radiograph).1,6,7 It may also be necessary to administer fluid therapy with saline solution to treat hypovolemia and antiplatelet therapy to counteract platelet aggregation. Associated complications should also be treated.1 In mild cases, such as ours, treatment is symptomatic provided that relevant tests have ruled out the involvement of other organs.
In conclusion, cutaneous manifestations of decompression sickness may be the first sign of a series of events associated with high morbidity and mortality, particularly in cases of delayed diagnosis and treatment. The lack of reports in the literature of cutaneous manifestations of decompression sickness should not lead us to underestimate the potential gravity of this situation.
We thank Rosa Taberner for her advice and guidance.
Please cite this article as: Pérez-López I, Blasco-Morente G, Ruiz-Villaverde R, Tercedor-Sánchez J. Erupción cutánea como única manifestación de enfermedad descompresiva leve. Actas Dermosifiliogr. 2015;106:515–516.