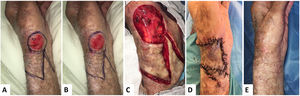
The so-called reading man flap was described by Mutaf et al.1 in 2008 as a new technique for covering circular defects. It takes its name from the form of the defect with the Z-plasties, which is reminiscent of the silhouette of someone reading (Fig. 1A). The technique is based on development of an asymmetric Z-plasty. It has been mainly used for reconstruction of facial defects. Given its most important characteristic is that it guarantees tension-free closure, we believe that it could be of great use for closure of defects at sites subject to flexion and tension movements.
A 102-year-old man, who was partially dependent for basic activities of daily living, but with complete mobility in his arms and who could eat without assistance, underwent a single surgical procedure in regimen of major outpatient surgery, under local anesthetic and sedation, for a circular squamous cell carcinoma in the radial dorsal region of the left wrist (Fig. 1B). The resulting defect measured 4 cm (Fig. 1C). A reading man flap was designed for reconstruction of the defect, which was sutured directly with silk 3/0 stitches (Fig. 1D). Daily dressing changes were done with chlorhexidine and soft bandaging, and the stitches were removed after 10 days. The patient was recommended not to lift weights or make forced movements with the arm for 15 days. No postoperative complications were reported, except for a small superficial necrosis at the vertex of the second flap. However, the esthetic and functional outcome at 3 months was very satisfactory (Fig. 1E).
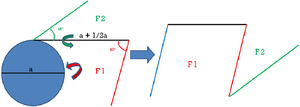
DiscussionThis reading man technique is based on the use of an asymmetric Z-plasty (Fig. 2). The central line, tangential to the defect, and perpendicular to the line of low skin tension, should be 50% longer than the diameter of the defect (black line). At the distal end, a line is designed forming a 60° angle with a length equal to the diameter of the defect (red line) and at the proximal end to the defect, another tracer line opposite to the anterior of equal length is added, forming a 45° angle (green line). Subsequently, a double transposition is performed by which the tumor defect is covered by the first rectangular-shaped flap (F1). This defect is in turn covered by transposition of the second triangular-shaped flap (F2).
In the literature, we encountered 14 articles that reported a total of 147 cases. The main site where this technique was used is the face, specifically the malar region,2,3 followed by the trunk. At the latter of these sites, the reading man flap has been used mainly for covering large defects after myelomeningocele interventions,4 or pressure ulcers.5 In such situations, it is a very useful alternative to myocutaneous or perforating flaps. However, we did not find any publication that highlighted the advantages of this plasty at sites of flexion and tension as was the case in our patient.
The reported rate of complications is relatively low. There have been a few reports of mild dehiscence and cases of dog ears and transient trapdoor effect have been reported due mainly to the first flap being too large.6 Also of note is a case of partial distal necrosis at the vertex of the second plasy.4 Such complications seem to be more frequent when used at an extrafacial site.7
This plasty has been compared with other transposition flaps such as the Limberg flap or the bilobed flap in models of artificial human skin and a lower suture tension; less removal of healthy skin, and a longer scar were demonstrated compared with the Limberg flap but with a similar scar area.1,8
The reconstruction of defects to cover periarticular areas is a therapeutic challenge, and transposition flaps are the most widely used, above all, bilobed flaps or Limberg flaps, as they allow the tension of closure to be reduced compared with other types of reconstruction. Good outcomes have been reported with the keystone-type flap in these areas9; however, most patients were younger and with a much less atrophied skin than was the case in our patient. Other options, such as complete skin graft, have the drawback of subsequent contracture of the graft and therefore a greater risk of functional limitations.
In summary, the reading man flap is a safe plasty that can be performed relatively easily. The main advantage is that it can guarantee closure with low tension. There is therefore a lower risk of necrosis, dehiscence, and poor wound healing, with less distortion and traction of adjacent tissues, and less removal of healthy skin.10
ConclusionAlthough the reading man flap was initially described to cover circular defects on the cheek, and indeed it is a good option for this site, we believe that the advantages mentioned with respect to other local plasties make it a particularly useful option in regions submitted to high tension such as large defects on the trunk or those in body areas with movements of flexion and tension, such as the wrist in the case of our patient. In these regions of flexion and tension in particular, other reconstructive options such as grafts or Limberg plasties can generate more traction with a greater risk of functional deficit.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Martínez de Espronceda Ezquerro Í, Azcona Rodríguez M, Sarriugarte Aldecoa-Otalora J, Iglesias Zamora ME. Colgajo del lector como alternativa reconstructiva en regiones sometidas a movimientos de flexoextensión. Actas Dermosifiliogr. 2021;112:563–565.