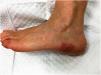
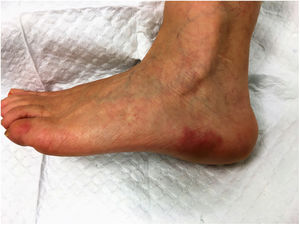
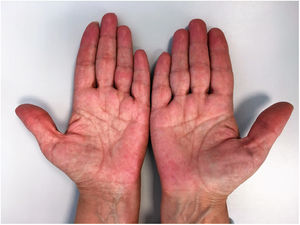
A 56-year-old caucasian female presented to our dermatology department with episodes of erythematoviolaceous dyschromia along the outer side of the left foot. The dermatosis had started 1year before and the patient was having 2-3 episodes per month, each one lasting from hours to a maximum of 2 days, with variable intervals between the crises. The condition was accompanied by a nonspecific local discomfort, although the patient denied manifest pain. Each episode evolved towards total resolution, with no sequelae. At this point, the functional impact caused by the dermatosis was negligible. Previous medical history was unremarkable and there were no new drugs administered. The patient had noticed the complaints were favored by the pending position of the left lower limb and contact with hot water and relieved with ibuprofen and by raising the limb. Physical examination revealed only 2 erythematoviolaceous plaques on the outer side of the left foot, with relatively well defined borders (Fig. 1). An incisional skin biopsy obtained from one of the lesions showed non-specific findings: a capilar proliferation in the dermis, with some ectatic vessels, and a a discrete lymphocytic inflammatory infiltrate. In the following months, thrombocytosis (800×109/L) and a borderline erythrocitosis (15,4g/dL) were detected in routine analyses and the patient was referred to hematology consultation. Concomitantly there was a clinical worsening of the dermatosis, with an increase in the frequency and severity of the episodes, including nocturnal, now inducing local pain, warmth and sensation of burning. The dimensions of the left foot plaque increased and the dermatosis progressed, involving both hands (Fig. 2) and feet, this time markedly limiting the functional capacity of the patient. At this point the patient underwent laboratory studies searching for autoimmunity, which were negative. Meanwhile the investigation performed in the context of hematology, with bone marrow examination findings compatible with a myeloproliferative neoplasm, allowed the diagnosis of polycythemia vera with positive JAK-2 mutation. Conjugating the clinical and histopathological data available with the polycythemia vera detected, the diagnosis of erythromelalgia secondary to the myeloproliferative disorder was established. In collaboration with hematology, the patient was started on hydroxyurea 500mg/day and acetylsalicylic acid 100mg/day and advised to avoid the precipitating factors and comply with resting periods with raised lower limbs. This approach lead to an evident symptomatic improvement: after 6 months the patient had no more episodes of erythematoviolaceous plaques although reported occasional warmth and discomfort on the left foot. Platelet count and hemoglobin normalized.
Erythromelalgia is a rare clinical syndrome characterized by episodes of erythema, increased temperature and burning pain, primarily involving the extremities,1,2 with lower limbs being more commonly affected.3 Physical exercise, dependency of the affected limbs and heat exposure are potential triggers, while cold, rest and elevation relieve symptoms.1–4 The classification of this condition varies among authors, but essentially there are primary forms, which can be further divided into familial or sporadic of early (juvenile) or late (adult) onset, and secondary forms.5 Multiple diseases are associated with this clinical picture, such as myeloproliferative neoplasms, arterial hypertension, venous insufficiency, diabetes mellitus, systemic lupus erythematosus, rheumatoid arthritis, lichen sclerosus, gout, spinal diseases and multiple sclerosis.2,4,6 Associated diseases may precede erythromelalgia, coincide with the beginning of the disease or occur during its evolution.7,8 Ethiopathogenesis of erythromelalgia is not known. Vascular abnormalities, small-fiber neuropathy and arteriovenous shunting are thought to be involved, contributing to the erythema and pain, but is unclear which one is the inciting event or primary abnormality.1,4,5 Histology is usually non-specific and some biopsy specimens don’t show any pathological findings but capillary proliferation, swelling of endotelial cells, perivascular edema and a sparse lymphocytic infiltrate are common.2 There are no established diagnostic criteria, no clinical guidelines of management or large randomised controlled trials of treatment.3,9 Erythema, burning pain and hyperalgesia are features of many conditions. Posttraumatic reflex dystrophies, including causalgia, reflex sympathetic dystrophy and shoulder-hand syndrome, can closely mimic erythromelalgia. Peripheral neuropathies, peripheral vascular disorders, Fabry disease and bacterial cellulitis should also be included in the differential diagnosis.6,10 In the absence of a confirmatory diagnostic test, diagnosis is based on a careful history and supported by physical examination during the episodes and, once a diagnosis is established, potential secondary causes must be excluded.5 There is no universally effective treatment for erythromelalgia and the mainstay of therapy is support and avoidance of triggering factors.1,5 Cases of erythromelalgia that are associated with myeloproliferative disorders usually respond to aspirin.11 Otherwise, drugs acting in the neuropathy (gabapentin, tricyclic antidepressants, selective inhibitors of serotonina reuptake), in vasculopathy (acetylsalicylic acid, calcium channel blockers, prostaglandins) and various nerve blocks have been attempted, with variable success.1,4,5 In our case the patient presented initially with non-specific clinical and histological pictures. The diagnosis of erythromelalgia was only established after the detection of polycythemia vera and the exacerbation of the symptomatology, with the characteristic triad of erythema, hyperthermia and pain with intense burning. Our patient’s complaints were successfuly controled with daily low-dose aspirin. In our case, besides erythromelalgia, which can cause ulcers in severe cases, hydroxyurea, used in the treatment of polycythemia vera, can also induce distal cutaneous ulceration, an association to keep in mind in the follow-up of the patient. Erythromelalgia is a rare heterogeneous disorder with a variable spectrum of severity and should be considered in patients with paroxysmal neuropathic pain. It is probably underdiagnosed and its early recognition is crucial to minimize the impact on patients’ quality of life.
Please cite this article as: Gil F, Luís P, Duarte M, Martins C. Eritromelalgia secundaria: informe de caso. Actas Dermosifiliogr. 2020;111:885–886.