Psoriasis is a dermatosis, the pathogenesis of which is characterized by activation of the helper T cell (TH) subpopulations TH1 and TH17 and the expression of inflammatory mediators such as interleukins and antimicrobial peptides involved in fighting infection.1,2 In contrast to atopic dermatitis, the likelihood of superinfection of psoriasis plaques is low.3 However infectious triggers, such as streptococcal pharyngeal infection, are common in certain forms of psoriasis.4
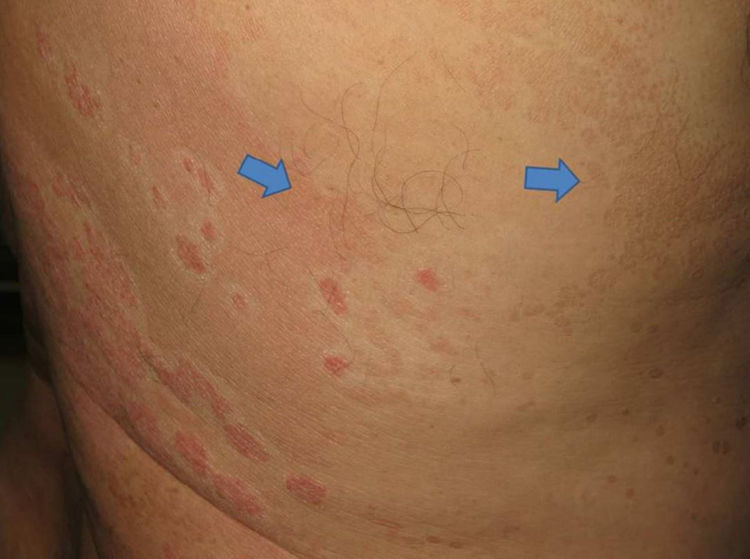
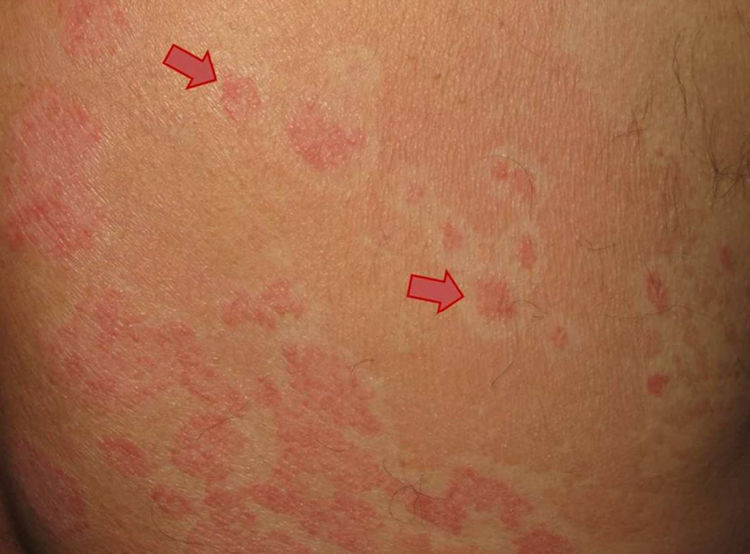
A 50-year-old man with a history of psoriasis vulgaris since youth was seen at our clinic for a rash affecting the trunk and arms. The clinical examination revealed 2 distinct dermatoses: reddish-brown, desquamative, confluent macular plaques that covered large areas of the trunk and were indicative of pityriasis versicolor (Fig. 1, blue arrows); and erythematous, keratotic plaques suggestive of psoriasis vulgaris (Fig. 2, red arrows). As shown in the images, the 2 dermatoses coexisted, but the pityriasis versicolor lesions spared the psoriasis plaques, with a margin of 5mm to 10mm.
The presumptive diagnoses of pityriasis versicolor and psoriasis vulgaris were confirmed by direct microscopic examination of a potassium hydroxide preparation and by histopathology of a skin biopsy of an adjacent keratotic plaque, respectively. Periodic acid–Schiff (PAS) staining revealed no fungal elements in the stratum corneum of the biopsied psoriasis lesion.
The patient was treated with a combination of oral itraconazole (100mg/d for 7 days) and narrowband ultraviolet B phototherapy, and achieved remission of both dermatoses 1 month after treatment.
Reports have described the colonization of psoriasis lesions by Malassezia species, which have been proposed to trigger lymphocyte activation, as described for other microorganisms.4–6 In some reported cases, Malassezia infection appears to trigger psoriasis via the Koebner phenomenon and the 2 dermatoses co-occur,7 albeit without sparing the areas affected by the concomitant dermatosis, as was observed in our patient. It is likely that psoriasis can co-occur with Malassezia colonization, which in some cases acts as a trigger and in others is merely an innocent bystander, depending on the equilibrium between the host's immune response and the microorganism's ability to produce a mycelium and proliferate. Likewise, different Malassezia species may provoke distinct immune responses, and associated Koebner responses of greater or lesser intensity.8 The present case supports the theory that psoriasis is the result of aberrant activation of immunological pathways originally expressed in the human species for the control of infection.9 The TH17/interleukin 17 axis, which is activated in psoriasis, is a component of the immune system that is crucial in the defense against fungal infections.10 Although our patient presented both dermatoses concomitantly, the psoriasis lesions were strikingly separated from the pityriasis versicolor lesions. The interaction between the skin microbiome and the immune system is an attractive theory to account for the appearance of certain dermatoses, including psoriasis.11,12 While dysbiosis can lead to activation of the cutaneous immune system, even in the absence of clinical infection, in our patient the psoriasis was very clearly delimited from the pityriasis versicolor.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Romaní J, Casulleras A. Psoriasis y pitiriasis versicolor: juntas pero no revueltas. Actas Dermosifiliogr. 2019;110:317–318.