Distal digital keratoacanthoma (DKA) or subungual keratoacanthoma is a rare and aggressive variant of keratoacanthoma (KA) that typically arises in the distal subungual tissue or affects the proximal nail fold, giving rise to paronychia. It presents as a painful, expanding subungual tumor that frequently recurs.1,2 We present a patient with incontinentia pigmenti who developed DKA.
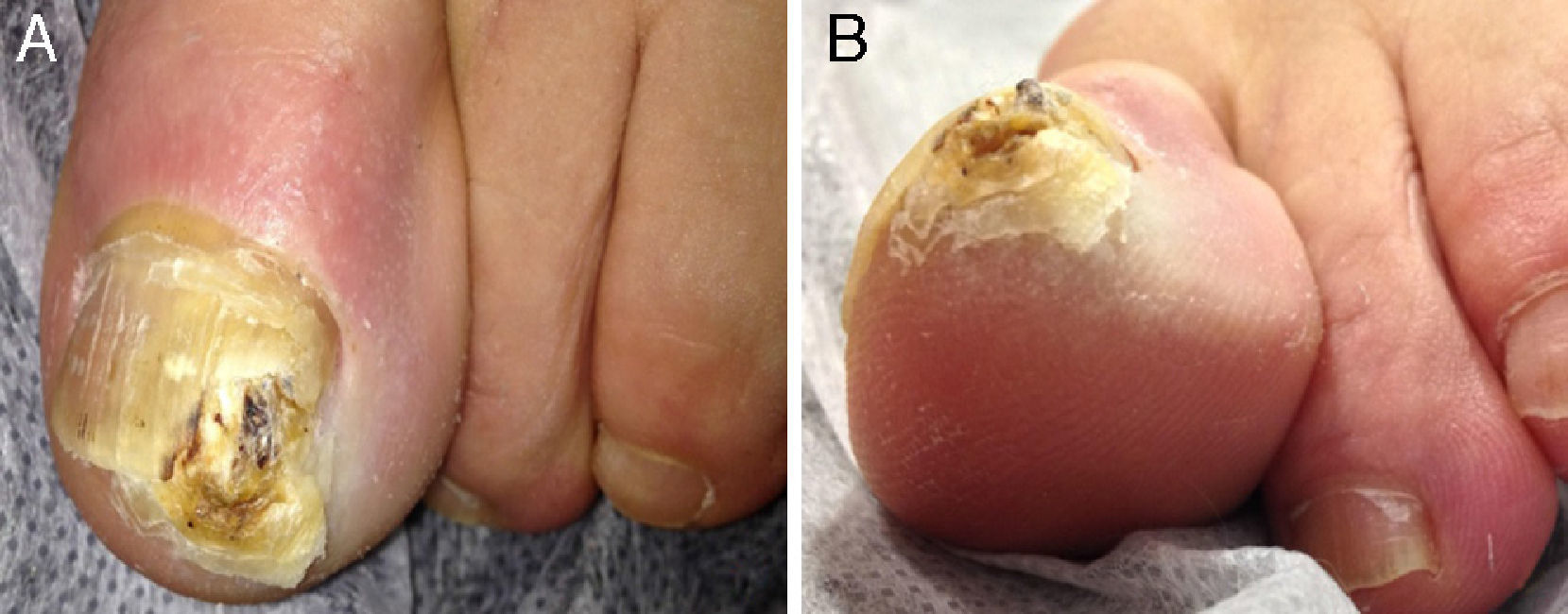
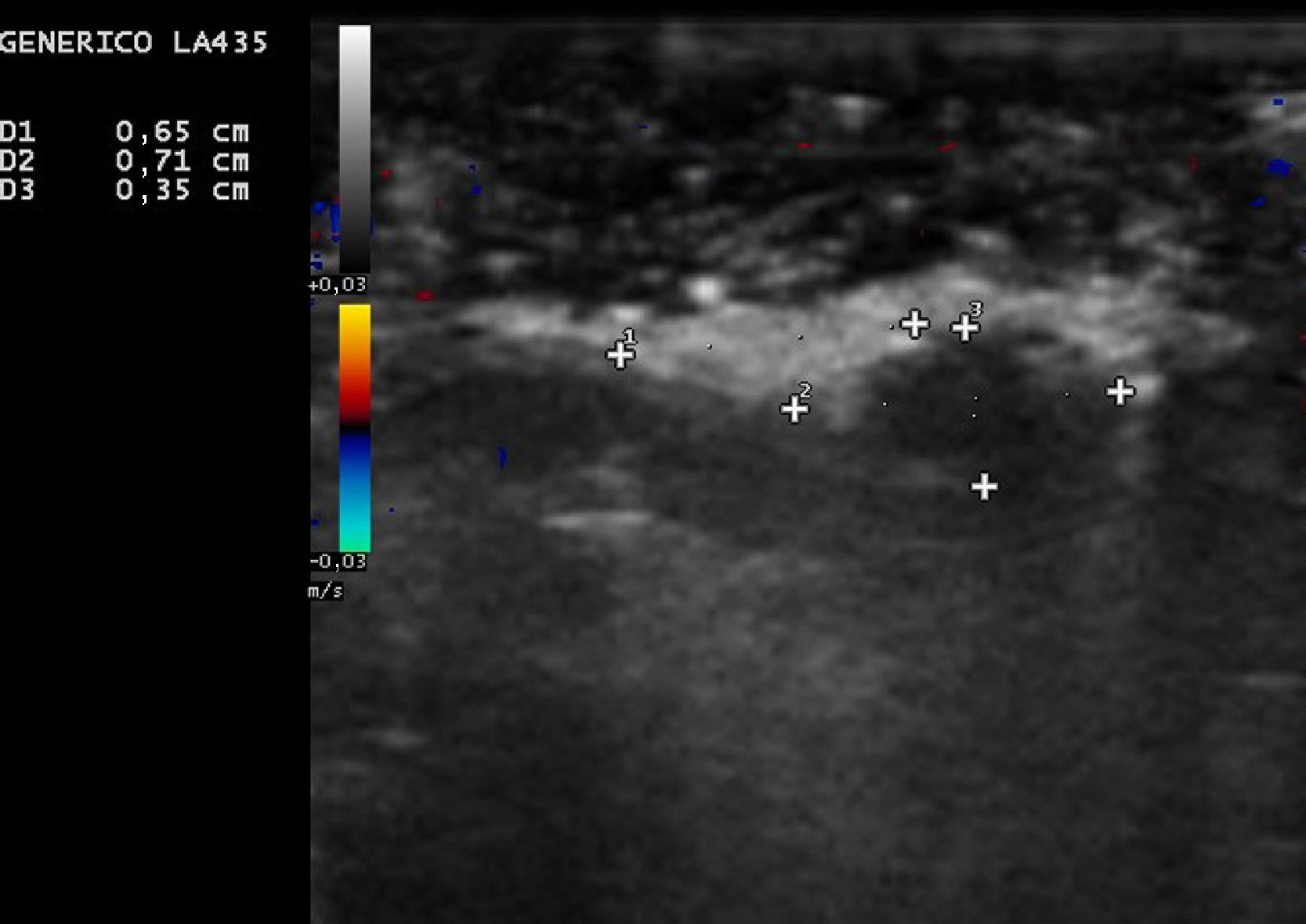
A 59-year-old woman with a past history of incontinentia pigmenti consulted for the appearance 2 months earlier of a very tender lesion under the nail of her left great toe. There was no history of trauma. Physical examination revealed a hyperkeratotic tumor that was destroying the distal lateral border of the nail of the left great toe, with mild inflammation (Fig. 1). Plain x-ray of the foot showed no bone involvement. Histopathology of the lesion after surgical excision showed a hyperplastic epithelium surrounding central cystic areas; there were dyskeratotic keratinocytes with very little atypia. Staining for oncoprotein p53 was negative; staining for Ki-67 revealed occasional cells in division above the basal layer of the epidermis. These findings were compatible with subungual DKA. One-and-a-half months later, the patient returned due to the appearance of a lesion with similar characteristics in the area of the previous surgery, suggestive of tumor recurrence. Nail ultrasound showed thickening of the nail plate, under which was an isoechogenic, oval lesion measuring 0.71cm in its longest axis (Fig. 2), with no increase in central vascularization on Doppler study. Based on these findings, a second surgical excision was performed, with the same diagnosis.
DKA is a rare destructive subtype of KA. It is more common in men, and particularly affects the first 3 digits of the hand.3 DKA typically develops as a rapidly growing and very painful verrucous or hyperkeratotic nodule that arises at the distal digital border of the nail, separating the nail plate from the bed, and it is usually associated with onycholysis.4,5 The rapid growth of DKA often provokes bone erosion by compression; radiographically this appears as a clearly defined cup-shaped defect of the distal phalanx, with no associated sclerosis or periosteal reaction.1,4,5 Ultrasound usually demonstrates a mass of intermediate echogenicity with posterior acoustic enhancement due to the cortical erosion of the distal phalanx.6 The diagnosis is confirmed histologically by the presence of areas of epidermal hyperkeratosis and parakeratosis associated with a central crater full of keratin5; the presence of dyskeratotic eosinophils is very common.1,7 An entity with similar clinical and histologic characteristics is the painful subungual tumor in incontinentia pigmenti, which can occasionally lead to diagnostic error because of its similar clinical appearance, although this latter lesion is more common on the fingers. The painful subungual tumor in incontinentia pigmenti occurs exclusively in women, predominantly between the ages of 15 and 30 years; a hormonal influence has been suggested because these tumors characteristically disappear during pregnancy and reappear postpartum.8
Histologically, subungual tumor in incontinentia pigmenti presents a hyperplastic epidermis with papillomatosis, acanthosis, and prominent dyskeratotic keratinocytes. Immunohistochemistry usually shows mild-to-moderate positivity for p53, Ki-67, and PCNA (proliferating cell nuclear antigen). Although these lesions do not recur after surgical excision, the appearance of multiple subungual lesions at other sites is common.8,9 To avoid this situation, some authors have proposed the use of systemic retinoids, with good results.2,8
In the differential diagnosis it is especially important to exclude squamous cell carcinoma (SCC), because of its therapeutic and prognostic implications. Epidemiologically, DKA usually arises in younger patients than SCC. In addition, DKA is characterized by rapid growth over a few weeks or months until it stabilizes (although, in contrast to KA at other anatomic sites, spontaneous regression is very rare), whereas SCC grows slowly but relentlessly.3,5 The use of immunohistochemistry stains for p53 and Ki-67 is useful for histologic differentiation of the 2 tumors, as these markers are diffusely positive in SCC but are negative in DKA.10 Other diseases that must be included in the differential diagnosis are common warts, subungual epidermal cysts, and onychomycosis. The most widely used initial treatment for DKA is conservative surgery, although recurrence is common, as in our case. Amputation is reserved for cases with multiple recurrences or when histologic differentiation from SCC is not conclusive.
In conclusion, DKA is a rare tumor, but it tends to recur and produce bone erosion. Its relevance derives from the importance of the differential diagnosis with SCC, a neoplasm with a poorer prognosis and that requires a more aggressive treatment than was used in our case.
FundingThe authors declare that they have received no funding for this study.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Martínez-López A, Blasco-Morente G, Pérez-López I, García-Durá E. Queratoacantoma digital distal en paciente con incontinencia pigmenti. Actas Dermosifiliogr. 2016;107:257–258.