Pseudomonas aeruginosa is a strictly aerobic, gram-negative, motile bacillus bacterium. It is widely distributed owing to its minimal nutritional requirements, tolerates a wide temperature range (4°C–42°C), and thrives in moist environments. These characteristics allow this bacterium to multiply in hot tubs with low chlorine concentrations, swimming pools, saunas, and hydrotherapy facilities.
P aeruginosa can cause a very broad spectrum of infections, which largely depend on the immune status of the affected individual. The most commonly reported infections include otitis externa, paronychia, intertigo, folliculitis, cellulitis, and abscesses.1 Upon skin contact with contaminated water P aeruginosa colonizes the skin and can enter the hair follicles or skin wounds, infecting the superficial portion of the pilosebaceous unit.
The most common presentation is folliculitis, characterized by the presence of follicular, macular, papular, vesicular, or pustular lesions on the axillae, sides of the thorax, abdomen, groin, perianal area, or any part of the body that has been submerged in contaminated water. P aeruginosa infection can also manifest as hot foot syndrome or hot hand-foot syndrome,2 characterized by the formation of nodules on the palms of the hands and the soles of the feet. In some cases, the release of exotoxins can cause systemic clinical signs including fever, gastrointestinal disorders, otalgia, and odynophagia.3
The clinical presentation is evident within 6 to 48hours after bathing and is usually self-limiting, resolving within 1 to 2 weeks.4
One of the main differential diagnoses is folliculitis caused by Staphylococcus aureus, which is characterized by a circular pattern of laminar desquamation around the infected hair follicle. The differential diagnosis should also include scabies, arthropod bites, and other bacterial skin infections.5
In most cases folliculitis caused by P aeruginosa is managed with topical treatment, although systemic treatment may be required in cases involving fever, constitutional symptoms, extracutaneous involvement, or immunocompromise.
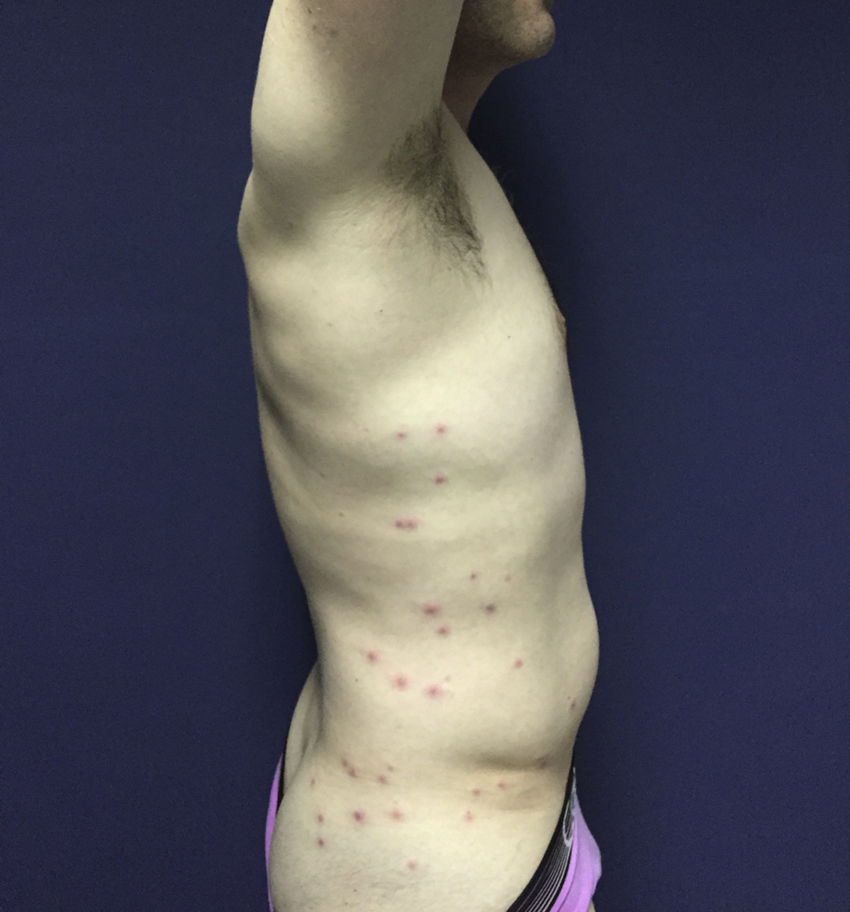
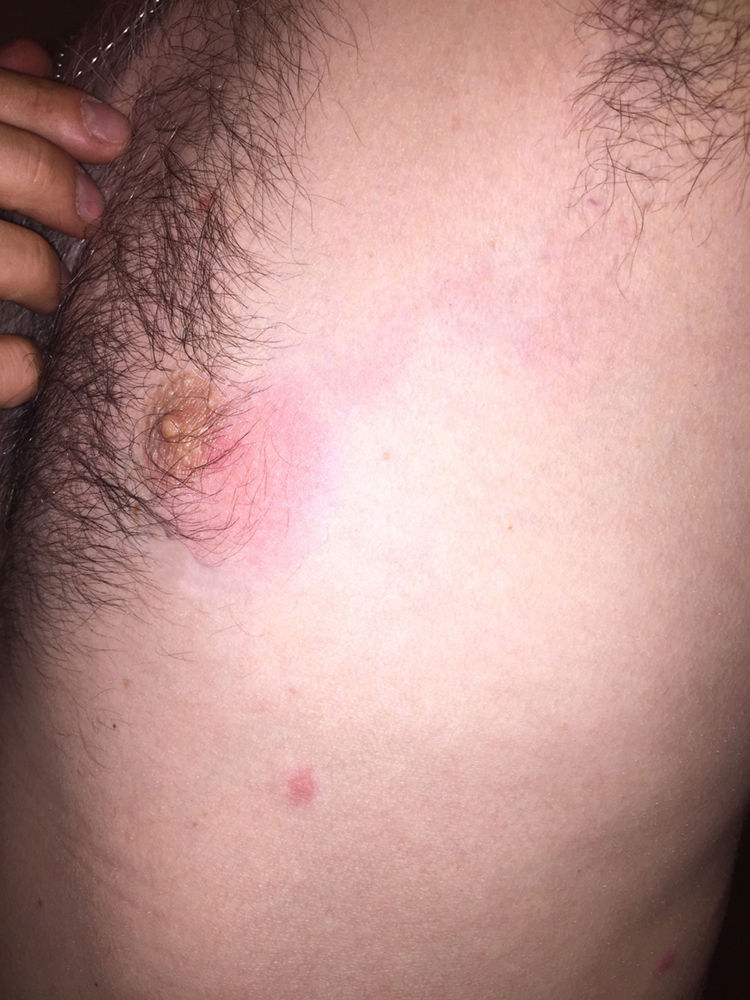
Case DescriptionA healthy, 35-year-old man was seen for follicular pustules and papules with an inflammatory erythematous halo. The lesions were neither painful nor pruritic and were located on the thorax, the side of the abdomen, the gluteus, and lower extremities (Fig. 1). On each breast was an erythematous macular lesion with poorly-defined borders. From the lesion on the left breast a serpiginous, erythematous trail extended from the periareolar region to the left axilla (Fig. 2), where a mobile and sensitive inflammatory lymph node of 1.5 cm in diameter was palpable. All lesions had appeared 48hours after the patient bathed in a hot-water whirlpool bath in his home. The patient showed no signs of general compromise and fever was absent. Upon suspicion of folliculitis due to P aeruginosa complicated by mastitis, pustule samples were collected for culture and the patient began empirical treatment with ciprofloxacin (500 mg/12 h) for 7 days. The affected area was cleaned with antibacterial soap twice per day during the treatment period. The patient progressed favorably, and the lesions resolved completely after 96hours. Bacterial culture revealed the presence of multidrug-sensitive P aeruginosa.
There are several reports in the literature describing hot-tub-associated P aeruginosa infections, including otitis externa, balanitis, omphalitis, green-nail syndrome, and genitourinary tract infections (for which risk factors include sexual activity in whirlpool baths and exposure of the genitals to water jets).6
Diseases that can occur concomitantly with P aeruginosa folliculitis include P aeruginosa pneumonia and hypersensitivity pneumonitis due to Mycobacterium avium.7
The condition of our patient, a man with bilateral mastitis as a complication of P aeruginosa folliculitis associated with whirlpool-bath use, represents an unusual manifestation of this pathology, of which no cases are described in the literature.
We believe it is important to report this case given the significant increase in diseases associated with the bathing in whirlpools, swimming pools, and spas.8
Topical treatment options include polymyxin B, gentamicin, 2% acetic acid, and benzoyl peroxide (which helps avoid the development of resistance). Systemic treatment may be selected for patients who are immunocompromised or have fever, constitutional symptoms, or associated mastitis. Some cases in the literature describe treatment of affected patients with ciprofloxacin (0.5–1 g/d) while awaiting the results of antibiotic sensitivity tests.9 Contamination of water with P aeruginosa can be prevented by changing the water daily, maintaining the pH between 7.2 and 7.8 and chlorine levels above 0.5 mg/L, and ensuring adequate drainage and drying of whirlpool baths after use.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Hott K. Mastitis bilateral como complicación de foliculitis por Pseudomonas aeruginosa, secundaria a uso de bañera de hidromasaje. Actas Dermosifiliogr. 2019;110:501–502.