The term mycoplasma pneumoniae-induced rash and mucositis (MIRM) was proposed to include various types of mucocutaneous rashes associated with Mycoplasma pneumoniae (MP) and differentiate them from drug-induced Stevens-Johnson Syndrome (SJS)/toxic epidermal necrolysis (TEN) and erythema multiforme.1–3 Based on its relationship with other causal infectious agents, in 2019, Ramien and Bruckner4 proposed the term reactive infectious mucocutaneous eruption (RIME) to include these entities.
A previously healthy 3-year-old girl, diagnosed with a 5-day history of gingivostomatitis was admitted to the ER due to worsening lesions and increased fever over the past 24hours, along with refusal to eat and hematemesis.
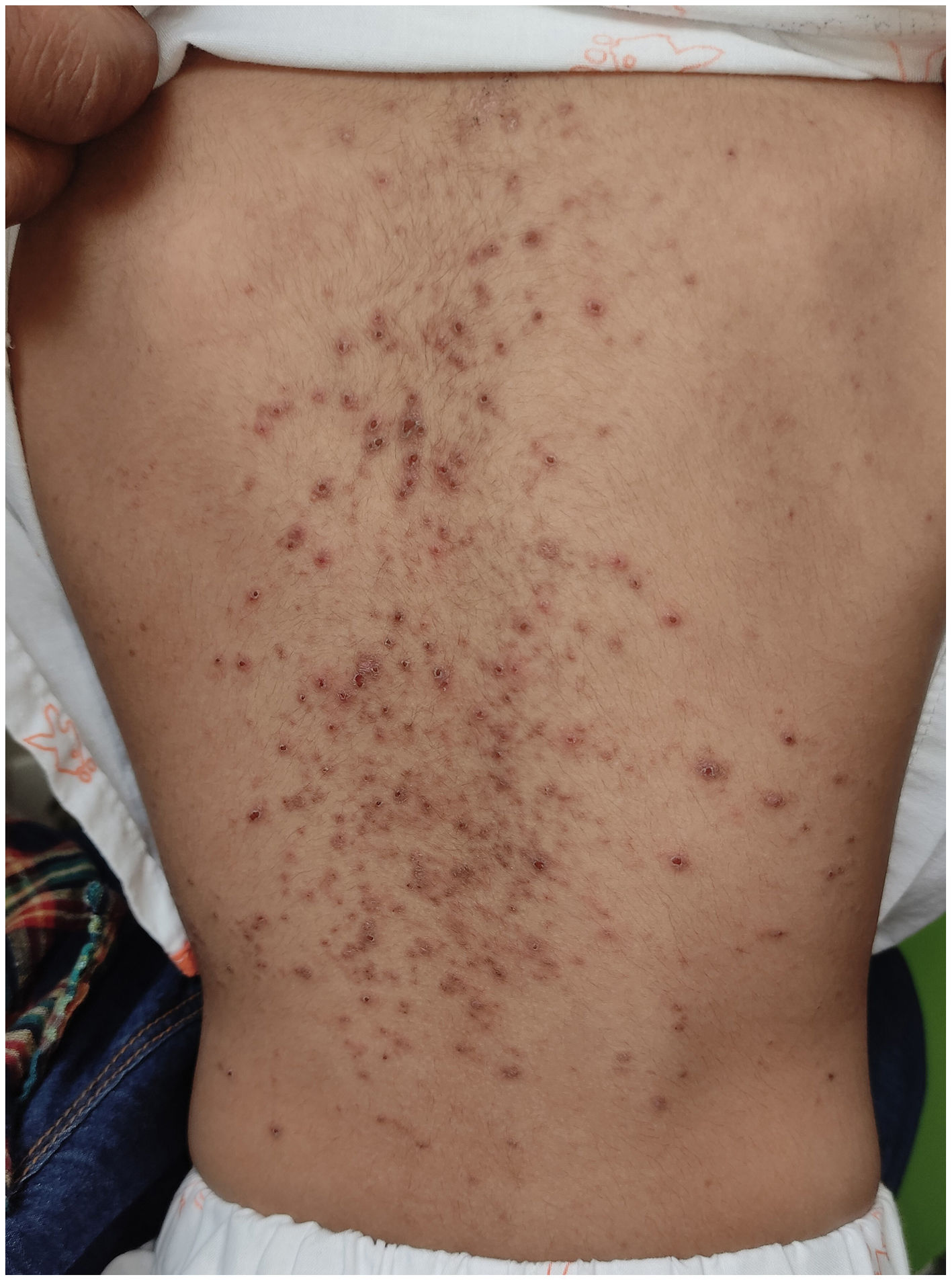
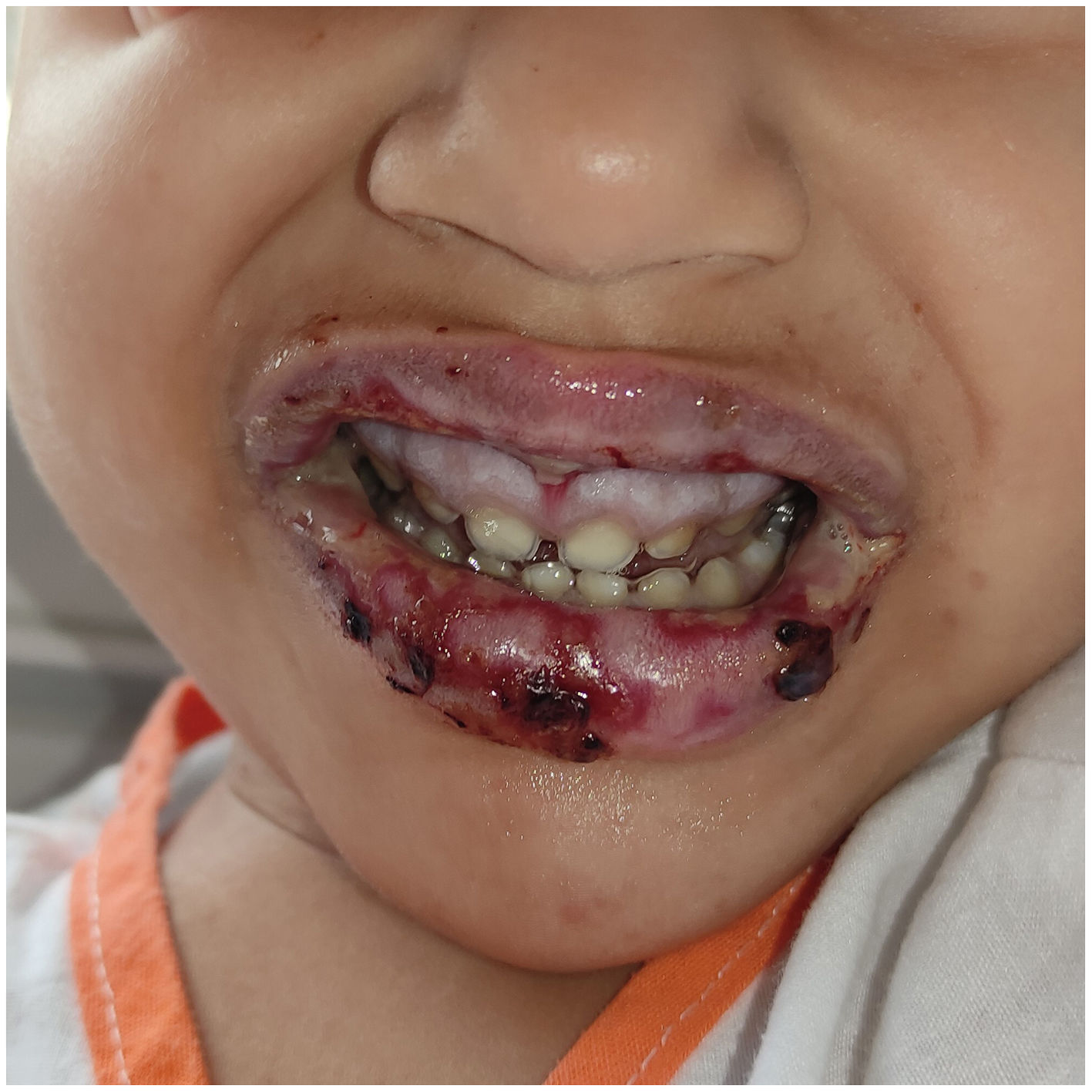
On physical examination, she exhibited edematous and friable lips with black crusts, gingivitis, erosions, ulcers, and whitish membranes on the oral mucosa. Additionally, she exhibited 3 purple lesions on her arms and thighs—which her parents attributed to insect bites—and hyperchromic spots on her thighs that—again according to her parents—had been present since birth. She had a fever of 38.5°C, mild tachycardia—124 bpm—and normal findings for the remaining vital signs. Lab test results revealed metabolic acidosis (pH 7.28; bicarbonate 10 mmol/L) and a C-reactive protein (CRP) levels of 2.16mg/dL.
She was admitted and put on IV amoxicillin-clavulanic acid, fluid therapy, topical nystatin, analgesia, and topical wound care. Small ulcerative lesions were noted on the vulva and papulocrustous lesions on the trunk and palms. Due to significant involvement of the lips and oral mucosa, IV acyclovir was started.
Serologies for cytomegalovirus, herpes simplex virus types 1 and 2, hepatitis C, and HIV tested negative while the varicella-zoster IgG blood test turned out positive. The PCR from an oropharyngeal swab tested positive for human herpesvirus 6 (HHV-6) and Haemophilus influenzae (H. influenzae) while the PCR from the vulvar lesions tested positive for H. influenzae.
A consultation with Dermatology diagnosed RIME due to HHV-6 infection with superinfection by H. influenzae. An IV 1mg/kg/day regimen of corticosteroid therapy was initiated, which led to regression of oral and skin lesions and an improved oral intake. She completed a 10-day regimen of antibiotic therapy and a 6-day course of IV acyclovir and corticosteroids. She was eventually discharged. Follow-up in outpatient clinics revealed residual hyperchromic macular lesions on the trunk and extremities and hypopigmented residual lesions on the lips.
The term RIME includes MIRM and other similar parainfectious mucocutaneous eruptions. Recently, other etiologies have been described besides MP, including Chlamydophila pneumoniae, influenza B, enterovirus/rhinovirus, metapneumovirus, parainfluenza 2, and SARS-CoV-2.5–7 Other possible triggers include varicella-zoster virus, hepatitis A virus, Epstein-Barr virus, cytomegalovirus, adenoviruses, and HHV-6.5
HHV-6 mainly causes asymptomatic infections and, typically in childhood, roseola infantum. The involvement of HHV-6 has been postulated in pityriasis rosea, mononucleosis-like syndromes, and RIME. It exhibits tropism for CD4+ T-lymphocytes, remaining latent and potentially reactivating in immunosuppressive situations, and can activate other potentially oncogenic viruses (Epstein-Barr virus and human herpesvirus 8).8
Patients typically exhibit intense mucositis in 2 or more locations and a prodromal phase (cough, fever, malaise, and headache,4 with possible pulmonary involvement in the form of pneumonia). Skin involvement is usually limited (34%), with vesiculobullous lesions (most common) or target lesions, papules, macules, or morbilliform lesions7 (Fig. 1). Oral involvement (94% up to 100%)5 includes hemorrhagic lip crusts and erosions and ulcerations in the buccal mucosa and tongue (Fig. 2). Ocular involvement (82% up to 92%) shows as bilateral purulent/seromucous conjunctivitis and eyelid edema. Urogenital mucosal involvement occurs in 60% of cases7.
Diagnosis is often clinical. Blood tests are advised and show elevated acute-phase reactants, serology for MP, chest X-ray, and PCR from a nasopharyngeal/oropharyngeal swab for MP, C. pneumoniae, respiratory viruses, and herpes simplex.5 Skin biopsy is not routinely performed.7
Differential diagnosis includes drug-induced SJS/TEN, grouped under the term drug-induced epidermal necrolysis (DEN).9 This condition is triggered by drugs—antibiotics, antiepileptics—presents with extensive skin necrosis, and has less mucosal involvement. It tends to be more severe, requiring admission to intensive care or burn units, and has a higher rate of sequelae (90% skin, 70% up to 93% ocular).
Other entities to consider include erythema multiforme, Kawasaki disease, pemphigus vulgaris or paraneoplastic pemphigus, herpetic gingivostomatitis, autoimmune diseases, and severe hand-foot-mouth disease.5,7
In children and young adults with an acute-onset rash and predominantly mucocutaneous involvement, preceded by a prodrome of an upper respiratory infection and no history of drug use, the initial presumptive diagnosis is RIME/MIRM.4,9
No evidence-based treatment has ever been established, and targeted antimicrobial therapy and supportive measures (analgesia, liquid diet or maintenance fluid therapy [avoiding nasogastric tubes], labial crust cleaning, mouthwash solutions for ulcers, ocular lubricants, and antibiotic/steroid eye drops, if needed) are usually sufficient. Dermatology and ophthalmology evaluation and follow-up are recommended in cases of ocular involvement.
Although targeted antibiotic therapy—macrolides, tetracyclines, or fluoroquinolones—is suggested, it does not appear to influence the course of the mucocutaneous eruption.4,7
In cases of extensive mucosal involvement, systemic corticosteroids—prednisone/methylprednisolone 1mg/kg/day for 5-7 days—can be administered.7 Other potential treatments include IV immunoglobulin, cyclosporine, or TNF-α inhibitors, though there is no supporting evidence.
Further studies are needed to understand the pathogenesis, natural history, and treatment response of RIME, as most current knowledge comes from case reports and clinical series.