Following the initial waves of the COVID-19 pandemic, an increasing number of case reports and series from around the world reported a potential association between herpes zoster and COVID-19.1,2 We present a new case of herpes zoster ophthalmicus (HZO) associated with this disease. The case also highlights the increased risk of HZO among both immunocompromised and immunocompetent young patients, which is a cause for concern.
A 25-year-old woman presented with a 2-day history of painful papulovesicular skin lesions against an erythematous background. The affected skin was particularly painful to the touch, with an “electric-like” pain accompanied by paresthesia. The patient had experienced some relief from over-the-counter analgesics.
Her medical history was unremarkable except for a recent case of moderate to severe COVID-19, confirmed by spiral computed tomography (CT) of the chest, which showed irregular areas of ground glass opacity in both lungs, compatible with COVID-19 pneumonia. The patient denied similar skin lesions in the past. Her general state of health was good before the onset of symptoms.
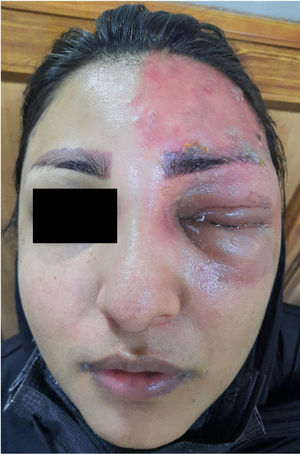
Vital signs were normal during the physical examination. Examination of facial skin showed vesicular papulopustular lesions on the left side of the face, not crossing the midline (Fig. 1). A fluorescein eye stain test showed no signs of corneal involvement. No lesions were observed on the nose or ears, including the external acoustic meatus. The neurologic examination was normal. The patient was diagnosed with HZO and prescribed antiviral therapy and local care for 10 days, which led to a significant improvement in lesions.
Herpes zoster is an opportunistic reactivation of the varicella zoster virus that occurs in patients with a weakened immune system. Older age is one of the main risk factors, particularly in immunocompetent patients.3,4
Our patient was a young woman with no clear or classic risk factors for HZO or associated conditions, except for a moderate to severe COVID-19 infection several weeks earlier.
Although herpes zoster in a patient with a history of COVID-19 may be a coincidence in certain cases, it has been hypothesized that SARS-CoV 2 infection might be linked to reactivation of herpes zoster in immunocompetent patients with a history of moderate to severe COVID-19. Potential mechanisms underlying the pathophysiology of herpes zoster reactivation after acute COVID-19 include T cell immune dysfunction,2 immunological aberrations, and immune dysregulation due to COVID-19.1
This case report highlights the possibility of concurrent herpes reactivation and SARS-CoV-2 infection. More clinical and epidemiological studies are needed to shed light on this link.
FundingNo funding was received for this study.
Conflicts of InterestThe authors declare that they have no conflict of interest.