Owing to the information provided in the media about a possible association between skin lesions and SARS-CoV-2, we received many patients with self-limiting purpuric acral lesions during the month of April 2020.1
This situation paves the way for several lines of study, in which laboratory analysis can play an essential role and in which differences in the behavior of the virus in the body can be explained in many settings by cutaneous manifestations, both at diagnosis and during follow-up. We consider that, during the initial stage of the infection, the mucous membrane may play a key role with respect to immunoglobulin (Ig) A antibodies.
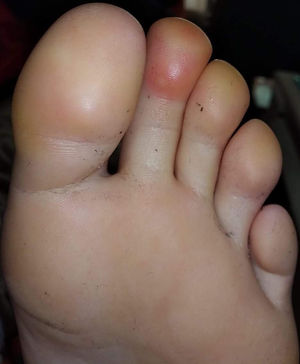
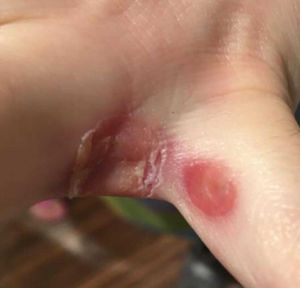
We retrospectively reviewed the cases of 11 patients with chilblain-like lesions2,3 seen at Hospital de Almansa, Albacete, Spain (Fig. 1). Some of the patients had had clinical manifestations associated with SARS-CoV-2 infection up to 2 weeks before the onset of the skin lesions. Patients were aged 2 to 40 years. The lesions comprised acral erythematous purpuric macules and papules4,5 accompanied by edema and occasionally progressing to blisters, vesicles, pseudopustules, and crusts (Fig. 2).
We requested the following analyses: complete blood count, liver enzymes, ferritin, antinuclear antibody, lupus anticoagulant, immunoglobulins, and anticardiolipin IgA, IgG, and IgM.6,7 We also analyzed anti-ß2-glycoprotein antibodies and complement C3 and C4 and ran a lateral-flow immunochromatographic assay (COVID-19 IgG/IgM Rapid Test Cassette, Zhenjiang Orient Gene Biotech Co., Ltd).
The Cov2019 polymerase chain reaction (PCR) assay, which is based on nasopharyngeal swab specimens, was performed in 2 cases where the patients had active symptoms and yielded a positive result in 1. The IgM/IgG rapid test, which was performed in all cases, yielded positive results in only 3 patients, 1 of whom had active disease (PCR+), and 2 asymptomatic patients, who had had self-limiting infection for 2 weeks, after which time they presented with chilblains. Laboratory tests revealed reduced complement C3 in 5 patients. All 5 had increased IgA anticardiolipin antibody; while this increase was slightly high, it was not considered positive according to the reference parameters of the external laboratory.
Analysis of the similarities between SARS CoV-2 infection and dermatologic syndromes involving antibodies enables conclusions to be drawn with respect to the following:
- 1.
The viral etiology of autoimmune diseases,6 as well as genetic and environmental diseases. Infection by SARS-CoV-2 is followed by a first stage of viral infection and a second stage that is similar to acute and transient autoimmune syndrome (in a genetically predisposed patient).
- 2.
Generation of autoantibodies: SARS-CoV-2 takes advantage of the body’s machinery to replicate. Microparticles (i.e., phospholipids such as phosphatidylserine), which are found on the cell membrane, stimulate production of autoantibodies. Exposure in blood vessels can lead to transient antiphospholipid syndrome, as reported in the literature,6 and could account for the skin lesions, as in antiphospholipid syndrome and chilblain lupus.
- 3.
Generation of IgA against the mucous membrane, where the first contact with the virus is made,6,8 thus explaining why the immune response has no memory (self-limiting conditions) and why only a few patients present memory IgG. It would also account for the severe symptoms that affect the mucous membranes, such as odynophagia, dysphagia, anosmia, and loss of taste, all of which are common in autoimmune diseases.
It is important to take into account the role of IgA autoantibodies in resolution of infection, especially in patients with mild symptoms, since SARS-CoV-2 affects the respiratory mucous membranes in the early stages of infection. This analysis could pave the way for early diagnostic and therapeutic strategies.8
The Ministry of Health document9 of April 24 on interpretation of diagnostic tests for SARS-CoV-2, distinguishes between 4 stages:
- 1.
Presymptomatic stage (PCR+).
- 2.
Initial stage (1-7 days). PCR+, with potentially positive IgA/IgM levels. Both symptomatic and asymptomatic individuals can transmit the infection.
- 3.
Second stage (8-14 days). IgA returns to negative values, and PCR may yield a negative result. IgM is positive and IgG may be positive. During this stage, the infection has usually resolved in asymptomatic individuals and in those with mild symptoms, and the risk of infection is minimal.
- 4.
Third stage (> 15 days). The PCR result may be positive and there may be an increase in IgG and IgM antibody levels. The infection has resolved in asymptomatic individuals and in those with mild symptoms. The infection is not considered to have resolved in severely ill patients until after 50 days.
In the patients reviewed here, anticardiolipin antibody tests were performed 4 to 8 weeks after onset of skin conditions owing to the difficulty associated with the pandemic.
In conclusion, the presence of antiphospholipid antibodies, whether in the context of systemic lupus erythematosus or primary antiphospholipid syndrome, has been associated with the development of chilblains. In this case, it would involve antiphospholipid syndrome secondary to acute and transient infection by coronavirus or another virus. This surprising clinical picture is atypical because it has a clear association with infection during the previous days,5 and not with extreme cold temperatures. In addition, although it has a temporal association with the pandemic, clear evidence of SARS-Cov-2 infection was only detected in 3 cases. The transient increases in immunoglobulins highlight the need for laboratory tests in the initial stage (i.e., the most infective stage). Furthermore, microparticles (phospholipids, glycoproteins) generate antibodies/autoantibodies, which disappear rapidly if they are IgA.
FundingNo grants were received from the public, commercial, or nonprofit sectors.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
I am grateful to the Head of the Laboratory at Hospital General de Almansa for showing such a high degree of intrinsic motivation. I am also grateful to the patients and, more than ever, to health professionals for their unceasing willingness to fight the current pandemic.
Please cite this article as: Cuenca Saez MA, Gomez-Biedma SL. Presencia de anticuerpos antifosfolípidos IgA en pacientes con lesiones pernióticas asociadas a COVID-19. Actas Dermosifiliogr. 2021;112:290–292.