Hookworm folliculitis is an atypical manifestation of cutaneous larva migrans (CLM) syndrome with which dermatologists should be familiar given the increase in travel to tropical and subtropical countries, where this entity is endemic. We present a case that was diagnosed in our hospital based on the patient’s clinical history and responded favorably to treatment after other more common potential etiologies were ruled out.
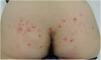
A 33-year-old woman in good general health with no pre-existing lesions was seen for lesions on the buttocks with associated, predominantly nocturnal pruritus. The lesions had appeared 1 month earlier after a trip to Argentina and Brazil. She had received treatment at another care facility with oral corticosteroids, amoxicillin-clavulanic acid, and betamethasone-gentamicin cream, without improvement. Physical examination revealed multiple erythematous papular lesions on the buttocks, some of which were excoriated (Fig. 1). The inguinal lymph nodes were not enlarged.
On suspicion of possible infectious folliculitis, a sample was taken for a herpes polymerase chain reaction test, biopsy, and laboratory tests, including serology for human immunodeficiency and hepatitis B and C viruses. The patient was prescribed valacyclovir (500 mg/12 h) for 5 days, fluconazole (50 mg/d), topical fusidic acid, and bilastine.
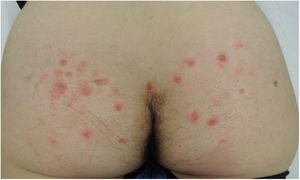
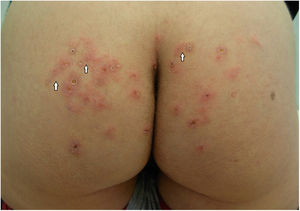
After 5 days the lesions had worsened, and a new lesion, suggestive of a serpiginous track, had appeared. While this new lesion could have developed secondary to scratching, its appearance raised clinical suspicion of CLM (Fig. 2). Histological findings supported the clinical suspicion, showing dermal edema together with a perivascular and periadnexal inflammatory infiltrate with abundant eosinophils and perifolliculitis, without destruction of the follicular epithelium.
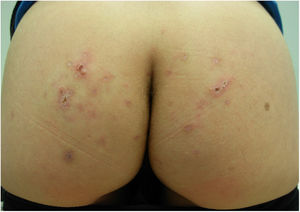
The results of a soft-tissue ultrasound, performed to attempt to visualize the parasite, were normal. However, given the prolonged clinical course of the condition and the clinical suspicion, the patient was prescribed oral albendazole (400 mg/d for 3 days). The lesions and the pruritus improved rapidly over the following weeks, resolving fully after 6 weeks without the need for additional treatment (Fig. 3).
We present a case of hookworm folliculitis, an atypical presentation of CLM syndrome. Hookworm folliculitis is a rare entity (the largest series described in the literature consists of 7 patients),1 and may be due to a hypersensitivity reaction to the presence of the nematode in the follicular canal.2–4
CLM syndrome is caused mainly by larvae of canine or feline nematodes (genus Ancylostoma),1,3–11 especially Ancylostoma brasiliense,1,4–11Ancylostoma ceylanicum,6,7,11 and Ancylostoma caninum.1,8–11 Larvae are expelled in dog or cat feces, contaminate the soil, and subsequently infect the host by transcutaneous penetration.1,3,5–8,11 This most often occurs on beaches in tropical and subtropical countries.1,3,5–8,11
After an incubation period ranging from days to weeks,1,3,8,10 patients who develop hookworm folliculitis present with multiple pruritic follicular papules and pustules, located mainly on the feet6–8 or buttocks.1,5–9 Some patients may present small, characteristically short (<5 cm) furrows1,5,6,8 that give rise to follicular lesions.1,2 Occasionally, vesicles and/or blisters may develop.1,3,6,7,9
Diagnosis of this entity is based on the clinical presentation together with recent travel to a tropical or subtropical country, and does not require additional tests.1,7,11 The differential diagnosis should primarily include folliculitis of other, more common etiologies (e.g. bacterial folliculitis, which tends not to cause such intense pruritus2,7), and scabies,6,7,11 which is associated with predominantly nocturnal pruritus. Laboratory analyses can reveal eosinophilia.1,3 Pathological analysis occasionally enables visualization of the parasites in the follicular ducts, although the most common finding is an eosinophilic infiltrate in the biopsy together with perifolliculitis,2–5,8 as observed in the present case. In a series of 8 cases of CLM published in this journal, parasite remains were detected in only 1 biopsy, and diagnosis was oriented based on the secondary findings described above.11
Ivermectin and albendazole are the first-line treatments.1,5,10,11 For the treatment of CLM syndrome ivermectin is usually administered in a single dose of 12 mg,2 while the albendazole dose is adjusted by weight (400–800 mg/d for 4 days).1 Treatment of hookworm folliculitis may be less effective than that of CLM, 1,2,5,7,9,10 and may require more doses of ivermectin or a combination of the 2 drugs.3,10 Topical albendazole (10%) can be used to treat children or patients for whom oral treatment is contraindicated.1 One case that responded to topical ivermectin treatment has also been described.12 Some cases can self-resolve without treatment within weeks or months.3,5–8,11
In conclusion, although hookworm folliculitis is very rare in Spain, the increase in travel to tropical and subtropical countries necessitates greater knowledge of tropical diseases5 in order to improve the quality of care of affected patients through rapid diagnosis and treatment, avoiding secondary infections and other complications.5,6
The key to diagnosis of this condition is the presence of cutaneous folliculitis-like lesions with intense, predominantly nocturnal pruritus in individuals that recently travelled to a tropical country.
Conflicts of interestThe authors declare that they have no conflicts of interest.
Please cite this article as: Saenz Aguirre A, Martínez de Salinas Quintana A, de la Torre Gomar FJ, Fatsini Blanch V. Foliculitis por larvas de nematodo: una infrecuente causa de foliculitis en viajeros. Actas Dermosifiliogr. 2020;111:275–276.