Poor self-assessed mental health appears to be related to the severity of psoriasis.
ObjectiveTo evaluate the impact of psoriasis severity on mood and anxiety disorders.
MethodsA prospective, observational, multicenter study was conducted by 123 dermatologists in Spain. Patients (n=164; mean [SD] age, 45.11 [13.92] years; 60.8% males) with moderate to severe psoriasis were evaluated at baseline and 4 months later. Psoriasis severity was measured using the Psoriasis Area and Severity Index (PASI), with a score range of 0 (mild) to 72 (severe); body surface area involvement (BSA); and physician global assessment (PGA) scores, with a range of 1 (mild) to 7 (severe). Mental health was assessed using the Hospital Anxiety and Depression Scale (HADS), with a total possible score of 0–42 (higher scores representing worse mental health). Mean first and second visit scores were compared.
ResultsMean (SD) scores improved between the first and second visit as follows: 13.24 (9.50) to 5.07 (6.03) for PASI, 12.52 (7.92) to 10.78 (7.32) for overall HADS, 7.83 (4.55) to 6.85 (4.21) for the HADS anxiety subscale, and 4.72 (4.12) to 3.95 (3.76) for the HADS depression subscale (P<.001 in all cases). Multivariate analyses showed that the main factors related to anxiety were psoriasis severity, sex, and completion of graduate studies. The independent variables included in the model for depression were psoriasis severity, sex, and psoriasis located on the head.
ConclusionsReductions in disease severity improve self-assessed mood and anxiety disorders in patients with moderate to severe psoriasis.
La gravedad de la psoriasis parece estar relacionada con una pobre autoevaluación de la salud mental.
ObjetivosEvaluar el impacto que tiene la gravedad de la psoriasis sobre los trastornos de ansiedad y del estado de ánimo.
MetodologíaEstudio prospectivo, observacional y multicéntrico realizado por 123 dermatólogos en España. Los pacientes con psoriasis moderada a grave (n=164; edad media [DE] 45,11 [13,92] años; 60,8% hombres) fueron valorados al inicio del estudio y 4 meses más tarde. Para medir la gravedad de la psoriasis se usó el Índice de Severidad y Área de Psoriasis (PASI) con un rango de puntuación entre 0 (leve) y 72 (grave); el área de superficie corporal afectada (BSA) y las puntuaciones de la evaluación global del médico (PGA) entre 1 (leve) y 7 (grave). La salud mental se evaluó utilizando la escala hospitalaria de ansiedad y depresión (HADS), con una puntuación total entre 0 y 42 (los valores más altos representan peor salud mental). Se compararon la media de las puntuaciones obtenidas en la primera y segunda visita.
ResultadosLa media (DE) de las puntuaciones mejoraron entre la primera y la segunda visita de la siguiente manera: de 13,24 (9,50) a 5,07 (6,03) para el PASI; de 12,52 (7,92) a 10,78 (7,32) para el HADS global, de 7,83 (4,55) a 6,85 (4,21) para el HADS subescala de ansiedad y de 4,72 (4,12) a 3,95 (3,76) para el HADS subescala de depresión (P<0,001 en todos los casos). El análisis multivariante mostró que los principales factores relacionados con la ansiedad fueron la gravedad de la psoriasis, el género y la finalización de los estudios de licenciatura. Las variables independientes incluidas en el modelo de estudio para la depresión fueron la gravedad de la psoriasis, el género y la psoriasis localizada en la cabeza.
ConclusionesLa reducción en la gravedad de la enfermedad mejora la autoevaluación de los trastornos del estado de ánimo y de la ansiedad en pacientes con psoriasis de moderada a grave.
Psoriasis is a common chronic inflammatory skin disease whose duration and clinical characteristics vary from patient to patient. Its etiology is unknown, but certain genetic and environmental factors that appear to be related to the development of psoriasis have been identified.1 The relationships between these factors are complex because genetic and environmental factors interact in the development of the different forms of the disease.2,3
Several studies have reported impaired health-related quality of life (HRQOL) in patients with psoriasis,4,5 with the greatest impact seen in social relationships and psychological well-being. To understand these effects, it is necessary to consider that plaques (or scales) may cover the entire skin surface and are sometimes difficult to conceal, causing embarrassment, low self-esteem, and body image problems. Therefore, patients with psoriasis may experience difficulty with positive social interactions, and as a consequence, have impaired mental health.
The impairment of psychological well-being in patients with psoriasis and the complex relationship between disease severity and psychological outcomes are well documented.6,7 Symptoms of anxiety and depression are common,5–8 but the severity of psychological outcomes is better correlated with self-assessed severity measures of the disease.9
Self-assessment questionnaires that evaluate psychological comorbidities are commonly administered to assess different diseases, and numerous HRQOL measures include items or dimensions for the assessment of mental health. The EuroQol 5D questionnaire, for instance, has an item that assesses anxiety and depression,10 and the Short Form 36 Health Survey also has dimensions that assess mental and emotional disturbance.11,12 One of the most widely used tools to assess psychological comorbidities, however, is the Hospital Anxiety and Depression Scale (HADS),13 which is a reliable, sensitive, and easily administered instrument14 that has been validated in Spain.15
The purpose of this study was to evaluate the most common psychological symptoms in patients with psoriasis (namely, anxiety and mood symptoms) and to demonstrate the effects of improvements in disease severity on psychological well-being.
MethodsDesignThis was a prospective, observational, multicenter study in which patients were recruited by 123 dermatologists throughout Spain within the VACAP Study (Assessment of the health-related quality of life and resource consumption in patients with moderate to severe plaque psoriasis). The patients were assessed during 2 visits: at baseline and after 4 months. The study was approved by the appropriate ethics and clinical research board. The patients were recruited consecutively at outpatient clinics. At the first visit, they were informed of the main objectives of the study and asked to provide their written informed consent to participation. The case report form comprised 2 sections. The first (completed by the dermatologists) collected demographic and clinical data relating to the patient and the second (completed by the patients) contained the quality of life questionnaire.
PatientsA total of 1217 patients with moderate to severe psoriasis were recruited. The inclusion criteria were a diagnosis of moderate to severe plaque-type psoriasis, an age of over 18 years, and provision of informed consent to participate in the study. Exclusion criteria were a diagnosis of psoriatic arthritis, participation in a clinical trial, and inability to read or understand the questionnaires and thus to fulfill the requirements of the study protocol. A diagnosis of moderate to severe psoriasis was made if the patients fulfilled 1 of the following criteria: (1) a Psoriasis Area and Severity Index (PASI) score of over 10 (range, 0–72), (2) a physician global assessment (PGA) score of 5 or more (range, 1–7), (3) body surface area involvement (BSA) of over 10%, and (4) any clinical indication for systemic treatment.
Assessment of psoriasis severityPsoriasis severity was measured by the participating dermatologists using 3 scores: PASI, PGA, and BSA.
Measures of mental healthThe HADS questionnaire was used for the assessment of mental health. HADS is a self-administered questionnaire designed to detect the presence and severity of mood and anxiety disorders.13 It is composed of 14 items grouped into 2 subscales: the HADS anxiety scale (HADS-A) and the HADS depression scale (HADS-D). Each subscale consists of 7 items with a possible score of 0–3. The final score is the sum of all items, i.e., a maximum of 21 on each subscale and a total possible score of 42. The HADS questionnaire has different cutoff scores to discern the likelihood of a psychiatric disorder. In this study, we used the cutoff of 12 used by Herrero et al.15 in their validation of the scale in Spain as an indicator of psychiatric morbidity on screening. For the screening of depressive and anxiety disorders, the optimal cutoff score was 5 for HADS-D and 8 for HADS-A.
Statistical analysesDatabases were generated and statistical analyses were performed using Predictive Analytics Software 18.0 (PASW Statistics 18.0). Descriptive statistics were calculated as means, variance, SD, range, median, 95% CI, and 5% trimmed mean for all questionnaire and scale scores. Categorical data were calculated as frequency distributions and percentages. Missing values were not included in the statistical analyses. Comparisons between means were performed with the t test or the nonparametric Mann–Whitney U test, and comparisons of frequency distributions were performed with the Pearson X2 test or the Fisher exact test, where a 2×2 contingency table was applicable. The level of statistical significance was set at α=.05.
Linear regression analysis was carried out to evaluate the relationship between demographic and clinical characteristics and psychological comorbidities. The dependent variables were the difference in HADS-A and HADS-D scores between the first and second visit. Independent variables in the model were included in a stepwise, algorithmic fashion, with an inclusion criterion of P=.05 and an exit criterion of P=.10. Categorical variables were transformed into dummy variables.
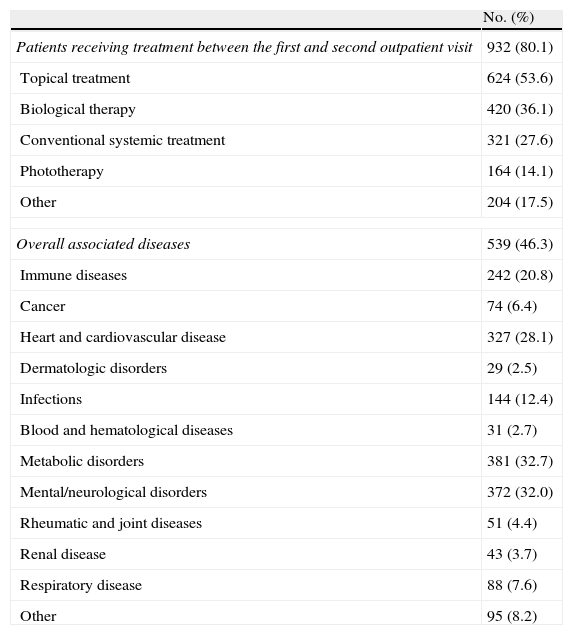
ResultsClinical dataIn total, 1164 patients provided the necessary information for the questionnaires at the 2 outpatient visits. The mean (SD) age of the patients was 45.11 (13.92) years, and a majority were male (60.8%); 68.1% were employed at the time of the study and 36.1% were receiving biological therapy. The most common comorbidities were metabolic disorders (32.7%) and mental (or neurological) disorders (32.0%). The demographic and clinical data are presented in Tables 1 and 2, respectively.
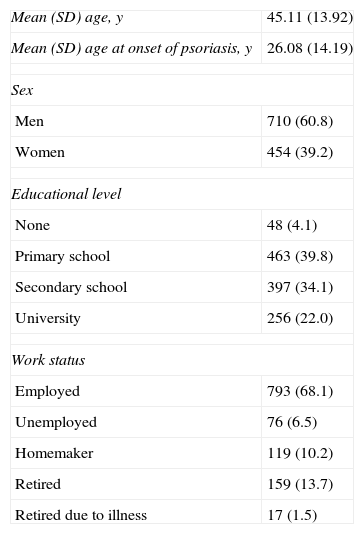
Demographic characteristics of study population.a
| Mean (SD) age, y | 45.11 (13.92) |
| Mean (SD) age at onset of psoriasis, y | 26.08 (14.19) |
| Sex | |
| Men | 710 (60.8) |
| Women | 454 (39.2) |
| Educational level | |
| None | 48 (4.1) |
| Primary school | 463 (39.8) |
| Secondary school | 397 (34.1) |
| University | 256 (22.0) |
| Work status | |
| Employed | 793 (68.1) |
| Unemployed | 76 (6.5) |
| Homemaker | 119 (10.2) |
| Retired | 159 (13.7) |
| Retired due to illness | 17 (1.5) |
Clinical characteristics of study population.
| No. (%) | |
| Patients receiving treatment between the first and second outpatient visit | 932 (80.1) |
| Topical treatment | 624 (53.6) |
| Biological therapy | 420 (36.1) |
| Conventional systemic treatment | 321 (27.6) |
| Phototherapy | 164 (14.1) |
| Other | 204 (17.5) |
| Overall associated diseases | 539 (46.3) |
| Immune diseases | 242 (20.8) |
| Cancer | 74 (6.4) |
| Heart and cardiovascular disease | 327 (28.1) |
| Dermatologic disorders | 29 (2.5) |
| Infections | 144 (12.4) |
| Blood and hematological diseases | 31 (2.7) |
| Metabolic disorders | 381 (32.7) |
| Mental/neurological disorders | 372 (32.0) |
| Rheumatic and joint diseases | 51 (4.4) |
| Renal disease | 43 (3.7) |
| Respiratory disease | 88 (7.6) |
| Other | 95 (8.2) |
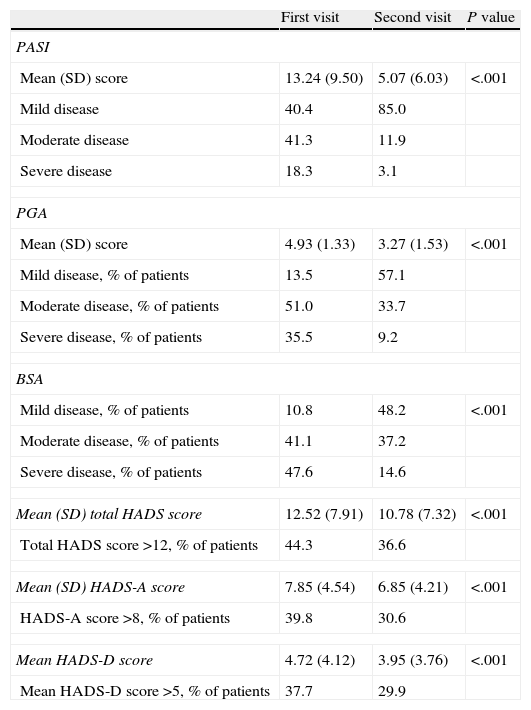
The mean PASI was 13.24 (9.50) at the first visit and 5.07 (6.03) at the second visit (P<.001). The percentage of patients with severe psoriasis decreased from 17.8% at baseline to 3.1% at the end of the study. Similarly, the proportion of patients with moderate to severe psoriasis also decreased (from 41.3% to 11.9%). All these differences were significant (P<.001) and indicate an improvement in the severity of psoriasis. The data are summarized in Table 3.
Results of psoriasis severity assessment tools and the Hospital Anxiety and Depression Scale (HADS).
| First visit | Second visit | P value | |
| PASI | |||
| Mean (SD) score | 13.24 (9.50) | 5.07 (6.03) | <.001 |
| Mild disease | 40.4 | 85.0 | |
| Moderate disease | 41.3 | 11.9 | |
| Severe disease | 18.3 | 3.1 | |
| PGA | |||
| Mean (SD) score | 4.93 (1.33) | 3.27 (1.53) | <.001 |
| Mild disease, % of patients | 13.5 | 57.1 | |
| Moderate disease, % of patients | 51.0 | 33.7 | |
| Severe disease, % of patients | 35.5 | 9.2 | |
| BSA | |||
| Mild disease, % of patients | 10.8 | 48.2 | <.001 |
| Moderate disease, % of patients | 41.1 | 37.2 | |
| Severe disease, % of patients | 47.6 | 14.6 | |
| Mean (SD) total HADS score | 12.52 (7.91) | 10.78 (7.32) | <.001 |
| Total HADS score >12, % of patients | 44.3 | 36.6 | |
| Mean (SD) HADS-A score | 7.85 (4.54) | 6.85 (4.21) | <.001 |
| HADS-A score >8, % of patients | 39.8 | 30.6 | |
| Mean HADS-D score | 4.72 (4.12) | 3.95 (3.76) | <.001 |
| Mean HADS-D score >5, % of patients | 37.7 | 29.9 | |
Abbreviations: BSA, body surface area; HADS-A, HADS anxiety subscale; HADS-D, HADS depression subscale; PASI, Psoriasis Area and Severity Index; PGA; physician global assessment.
There was also an improvement in mean PGA scores between the first and second visit (4.93 [1.32] vs 3.27 [1.53], P<.001). According to BSA scores, 48.1% of patients had over 10% skin surface involvement at the first visit, but this had dropped to 14.6% by the second visit (P<.001).
Between the first and the second visit, 80.1% of patients received treatment for their psoriasis (biological therapy in 35.7% of cases).
Mental health assessmentMean overall mental health scores (HADS) were 12.52 (7.91) at the first visit and 10.78 (7.32) at the second visit. The HADS-A score was higher than the HADS-D score at the first visit, but both scores had decreased by the second visit. The HADS-A score was 7.83 (4.54) at baseline and 6.85 (4.21) at the end of the study, while the HADS-D score was 4.72 (4.12) and 3.95 (3.76), respectively. The differences were significant (P<.001) in all cases. Using the cutoffs established by Herrero et al.,15 at baseline 44.6% of patients had some form of psychiatric comorbidity, 39.8% had scores consistent with depression, and 37.7% had scores consistent with anxiety. These percentages had decreased by the second visit to 36.6%, 29.9%, and 30.6%, respectively (P<.001 in all cases). The HADS scores are summarized in Table 3.
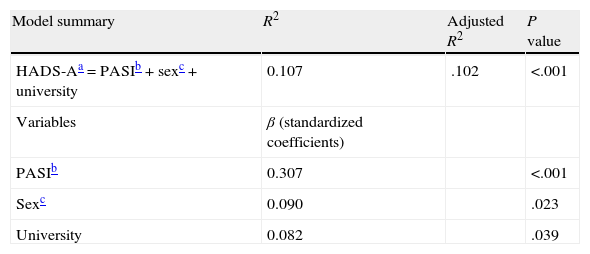
Examination of the independent contribution of variables suggested that the main factors related to anxiety were severity of psoriasis (measured by difference in PASI between visits) (β=.307, P<.001), sex (β=.090, P=.023), and the completion of graduate studies (β=.082, P=.039). The remaining variables were excluded using a stepwise algorithm. The results of the multivariate analysis with HADS-A as the dependent variable are shown in Table 4.
Multivariate linear regression analysis results for HADS anxiety subscale (HADS-A).
| Model summary | R2 | Adjusted R2 | P value |
| HADS-Aa=PASIb+sexc+university | 0.107 | .102 | <.001 |
| Variables | β (standardized coefficients) | ||
| PASIb | 0.307 | <.001 | |
| Sexc | 0.090 | .023 | |
| University | 0.082 | .039 |
Abbreviations: HADS, Hospital Anxiety and Depression Scale; PASI, Psoriasis Area and Severity Index.
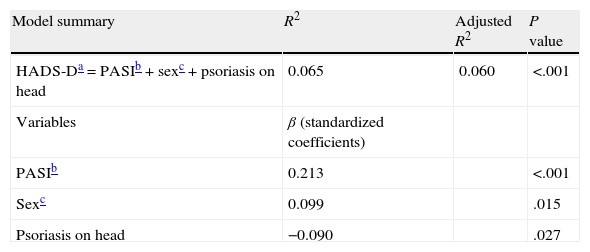
Evaluation of the contribution of variables to depression suggested that the main related factors were severity of psoriasis (β=.217, P<.001), sex (β=.099, P=.015), and psoriasis located on the head (β=−0.090, P=.027). The results of the multivariate analysis with HADS-D as the dependent variable are shown in Table 5.
Multivariate linear regression analysis results for HADS depression subscale (HADS-D).
| Model summary | R2 | Adjusted R2 | P value |
| HADS-Da=PASIb+sexc+psoriasis on head | 0.065 | 0.060 | <.001 |
| Variables | β (standardized coefficients) | ||
| PASIb | 0.213 | <.001 | |
| Sexc | 0.099 | .015 | |
| Psoriasis on head | −0.090 | .027 |
Abbreviations: HADS, Hospital Anxiety and Depression Scale; PASI, Psoriasis Area and Severity Index.
The importance of psychological well-being in outcomes research has garnered interest in recent years, and has been explored in several chronic conditions, including cancer,16,17 diabetes,18 chronic heart failure,19 and chronic pain.20
The results of the current study confirm the presence of psychological symptoms in psoriasis, with an improvement in disease severity being accompanied by an improvement in psychological well-being. The comorbidity of psychological disorders in psoriasis patients was confirmed by 2 sources of data: the clinical data collected and the results of the HADS questionnaire. Our findings support previous reports that anxiety and depression are mental components of severe psoriasis.5,8,21
The complexity of the relationship between skin diseases and psychological disorders was highlighted in a study by Magin et al.9 that examined psychological comorbidities in different skin diseases. The authors concluded that the relationship is complex and should be reanalyzed, and that personality traits may be a factor in this complexity, either as independent or dependent variables. They evaluated both hypotheses using the introversion/extraversion and neuroticism scales of the short form of the Eysenck Personality Inventory.22
An alternative interpretation of personality involvement in psychological disturbance in psoriasis patients is the evaluation of coping strategies and alexithymia traits. The alexithymia trait has an important weighting, and in a study by Fortune et al.23 it is related to a higher anxiety score, as measured by HADS. It is likely that this factor was an important component in explaining the findings of the current study, and it could, at least in part, explain the effect of different psychological outcomes in diseases such as psoriasis. It is likely that alexithymia interacts with psoriasis severity as a moderator factor.
The stigmatization experience is another important factor to consider when interpreting our results. Feelings of stigmatization are primarily related to the management of visible affected regions. As our results suggest, patients with psoriasis in visible areas have an increased level of depression,24 and there have been reports of a positive relationship between the objective severity of psoriasis or visibility of skin lesions and depressive symptoms.21
A multivariate sensitivity analysis showed a sex-specific effect on psoriasis morbidity. Women were more likely to have anxiety and depression problems than men; this might be a fact because they are affected to a greater degree by impaired body image due to psoriasis. A tendency toward a higher rate of mood and anxiety disorders among women has been observed and recorded in previous publications on psoriasis24,25 and other dermatological diseases.26
The current study shows that an improvement in psoriasis severity is accompanied by an improvement in associated psychological disorders. Hence, treatment of psoriasis is important for improving psychological disturbances in psoriasis patients. In our study, we observed an improvement in the patients’ mental health at the second visit. Managing the illness and the patient's personality are important in understanding psychological outcomes. Some patients need psychological or psychiatric assistance, which may be independent of psoriasis treatment. A key factor in evaluating whether or not a patient needs such assistance is the patient's own perception of the severity of their illness.22 Because PASI is generally not a reliable predictor of depression or anxiety,21 it is important to screen psoriatic patients for the presence of psychological comorbidities.
The current study, which is one of the largest of its kind to be published, assesses general health using real-life data in a series of patients with psoriasis. Its main limitation is the lack of a control group at the beginning of treatment. Our results therefore must be interpreted with caution. The improvement in the severity of psoriasis at the second outpatient visit is clear. However, we cannot clearly establish whether this was due to treatment alone. It is also likely that the fact that a high percentage of patients were receiving biological therapy contributed to this improvement. Of further note is the lack of data on psychological status at the beginning of the study. The high comorbidity of mental and neurological disorders in this study supports the proposed relationship between psoriasis severity and mental health. However, we are not able to define when these comorbidities appeared, i.e., before, after, or during the initial onset of psoriasis. Although we cannot confirm a causal relationship between the severity of psoriasis and mental health, our results do indicate a certain relationship. It may be necessary to differentiate the objective clinical severity of disease from the subjective perceptions of patients.
The present study shows that psoriasis has an important impact on mental health and confirms the presence of depressive and anxiety symptomatology in patients. The relationship between the symptoms and the illness is complex; certain personality traits need to be taken into account, and psychological disturbance due to the illness needs to be managed. It is clear that psoriasis impairs mental health, but further studies are needed to investigate whether other variables are involved in the relationship between the severity of disease and psychological disturbance.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that the procedures followed were in accordance with the regulations of the responsible Clinical Research Ethics Committee and in accordance with those of the World Medical Association and the Helsinki Declaration.
Confidentiality of dataThe authors declare that they followed the protocols of their work center on the publication of patient data and that all the patients included in the study received sufficient information and gave their informed consent in writing to participate in that study.
Right to privacy and informed consentThe authors obtained the informed consent of the patients and/or individuals mentioned in the article. The author for correspondence is in possession of these documents.
Conflicts of interestThis study received an unconditional grant from Schering-Plough. The authors confirm independence from the funding body in matters of study design, analysis, and interpretation of the data, report writing, and submission for publication.
The authors thank Covadonga Torres of Pharmacoeconomics and Outcomes Research Iberia (PORIB) for her assistance with the statistical analysis and the writing of this article.
On behalf of the VACAP Study investigators (see Appendix A).