After carefully reading the letter to the editor, “Genital Warts, Lymphangioma, and Treatment with Imiquimod”, by Monteagudo et al.1 concerning our recently published case report, we would like to respond with several clarifications.
The patient was an adult woman who presented with multiple papular lesions, some pedunculated, in the vulvar region, which had first appeared some years earlier. She reported that she had been assessed 5 years earlier for similar lesions, which were diagnosed as genital warts (condyloma acuminata) and treated with imiquimod cream 5% applied 3 times a week for less than 16 weeks, with apparent complete resolution of the lesions and no local side effects of note. However, since this information was reported to us by the patient when we first recorded her medical history, we do not have the results of any histologic study or molecular diagnostic tests with genotyping of the human papillomavirus that would allow us to confirm the diagnosis definitively.
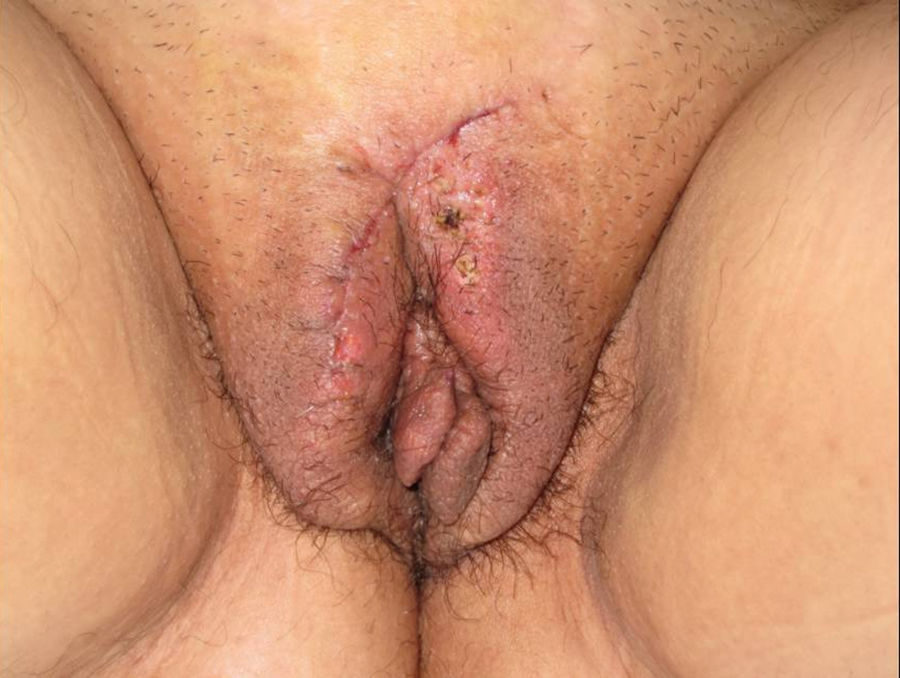
On physical examination, the lesions, which were located on the anterior vulvar fourchette and the labia majora, were observed to be highly monomorphic and composed of multiple papular elements forming a cobblestone pattern. We also observed an increase in the volume of the mons pubis and slight edema of the soft tissue. The patient reported that the edema had been present for a long time and was not related to the application of the imiquimod cream.
Given the complexity of the differential diagnosis, one of the wart-like lesions was biopsied and imaging studies were carried out; the results facilitated a diagnosis of acquired circumscribed vulvar lymphangioma.1
In this case, the treatment option chosen was surgical excision of the larger lesions and curretage and electrodesiccation of the smaller lesions, with a good clinical and cosmetic outcome (Fig. 1). The patient has remained asymptomatic, but is being followed up regularly with cycles of cryotherapy to treat small papular elements that continue to appear.
With respect to the hypothesis suggested by Monteagudo et al. regarding the possible etiologic and pathogenic role of imiquimod in lymphedema, and consequently in the appearance of vulvar lymphangiomas, we consider that it is more likely that the lesions presented by this patient 5 years earlier were also vulvar lymphangiomas and that they responded partially to imiquimod, as described in other cases reported in the literature.2
As has been reported previously, imiquimod can act as an angiogenesis inhibitor through the induction of endothelia cell apoptosis and the inhibition of interleukins and other proangiogenic factors.3 There have been reports of its usefulness, with variable response, in the management of vascular lesions of different types: infantile hemangiomas,4 lymphangioendotheliomas,5 lymphangioma circumscriptum,6 and Kaposi sarcoma7 affecting both genital8 and nongenital areas.
In conclusion, we reported on a case of acquired vulvar lymphangioma circumscriptum, a condition that can, given the site affected, present a diagnostic challenge because of the similarities with genital warts as well as a therapeutic challenge because it tends to recur. With respect to treatment, some authors have reported the usefulness of ablative approaches, including surgical excision, laser therapy, and cryotherapy and of topical antiangiogenic treatments, particularly imiquimod and rapamycin.9
Please cite this article as: Padilla-España L, Repiso-Jiménez JB, Millán-Cayetano JF. Verrugas genitales, linfangioma y tratamiento con imiquimod. Actas Dermosifiliogr. 2018;109:664–665.