An otherwise healthy 45-year-old man consulted for an asymptomatic lesion on the middle third of the right sole that had first appeared 18 months earlier. The patient did not recall injury to the area or the presence of a previous lesion.
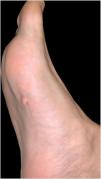
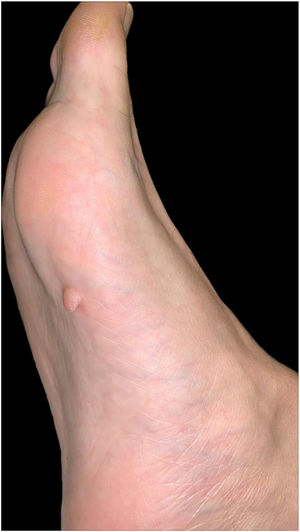
Physical ExaminationPhysical examination revealed a flesh-colored pedunculated tumor measuring 8mm in diameter. The tumor was soft, with a smooth surface, and was located on the middle third of the right sole (Fig. 1).
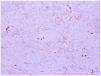
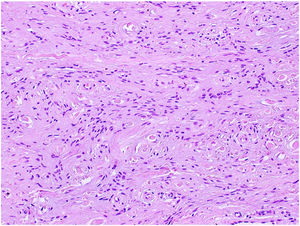
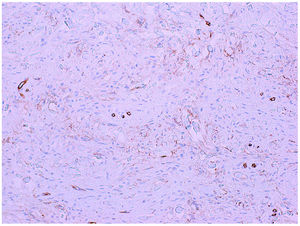
HistopathologyThe tumor was removed using excisional biopsy. Histopathology revealed a proliferation of spindle-shaped homogeneous cells immersed in a myxoid stroma in the dermis (Fig. 2, hematoxylin–eosin, 200×). The results of immunohistochemistry were positive for CD34 and negative for S100 (Fig. 3, immunohistochemistry CD34, 200×).
What is your diagnosis?
DiagnosisSuperficial acral fibromyxoma.
Clinical Course and TreatmentAfter diagnosis, the surgical margins were extended by 0.5mm. Histology revealed no relevant findings. No signs of recurrence have been observed after 10 months of follow-up.
CommentarySuperficial acral fibromyxoma is a benign mesenchymal tumor that mainly affects men in the fifth decade of life. In most published cases, the lesion is found in the periungual and subungual regions.1–3
Clinically, the tumor is usually nonencapsulated, well-circumscribed, polypoid or verrucous, and dome-shaped. It extends throughout the dermis, potentially as far as the subcutaneous tissue, underlying fascia, or periosteal layer.2–4
Radiology findings are nonspecific, although bone erosions or lytic lesions may co-occur in one-third of cases.1–5
Histopathology may reveal hyperkeratosis in the epidermis. Proliferation of spindle-shaped fibroblasts within a myxoid matrix, with nuclear atypia and mast cell infiltration, is a key finding in the dermis. Immunohistochemistry is positive for CD34, CD99, vimentin, and epithelial membrane antigen and negative for neural and muscular differentiation markers (S100, HMB-45, SMA, desmin, and actin).1,3,5
The differential diagnosis includes fibrokeratoma, fibroma, and plantar warts.3 It is also important to bear in mind tumors that are negative for CD34 (glomus tumor, sclerosing perineurioma, acquired digital fibrokeratoma, and periungual fibroma), as well as those that are positive for CD34 (superficial angiomyxoma, dermatofibrosarcoma protuberans, and myxoid neurofibroma).1,3,5
The treatment of choice is surgical resection with free margins, since local recurrence is recorded in approximately 20%–25% of cases. While the natural course of the tumor is benign, the histopathologic spectrum of spindle-shaped fibroblasts is variable, ranging from mild nuclear atypia to major atypia, with transformation to a low-grade malignant tumor being theoretically possible.4,6 However, prognosis is excellent, and, to date, there have been no published reports of malignant transformation or metastases.1,3–5
Conflicts of InterestThe authors declare that they have no financial or personal relationship with other persons or organizations that could give rise to a conflict of interest with respect to the present article.