Cutaneous hypopigmentation is a common local adverse effect associated with corticosteroid treatment. A much less common effect associated with intralesional corticosteroid injections is linear atrophy and hypopigmentation along the path of the lymphatic channels.1
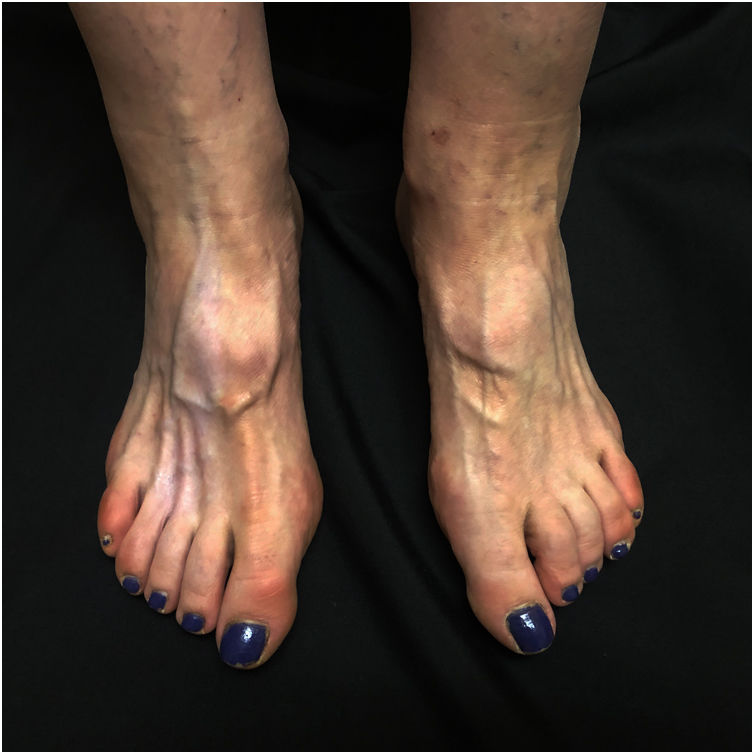
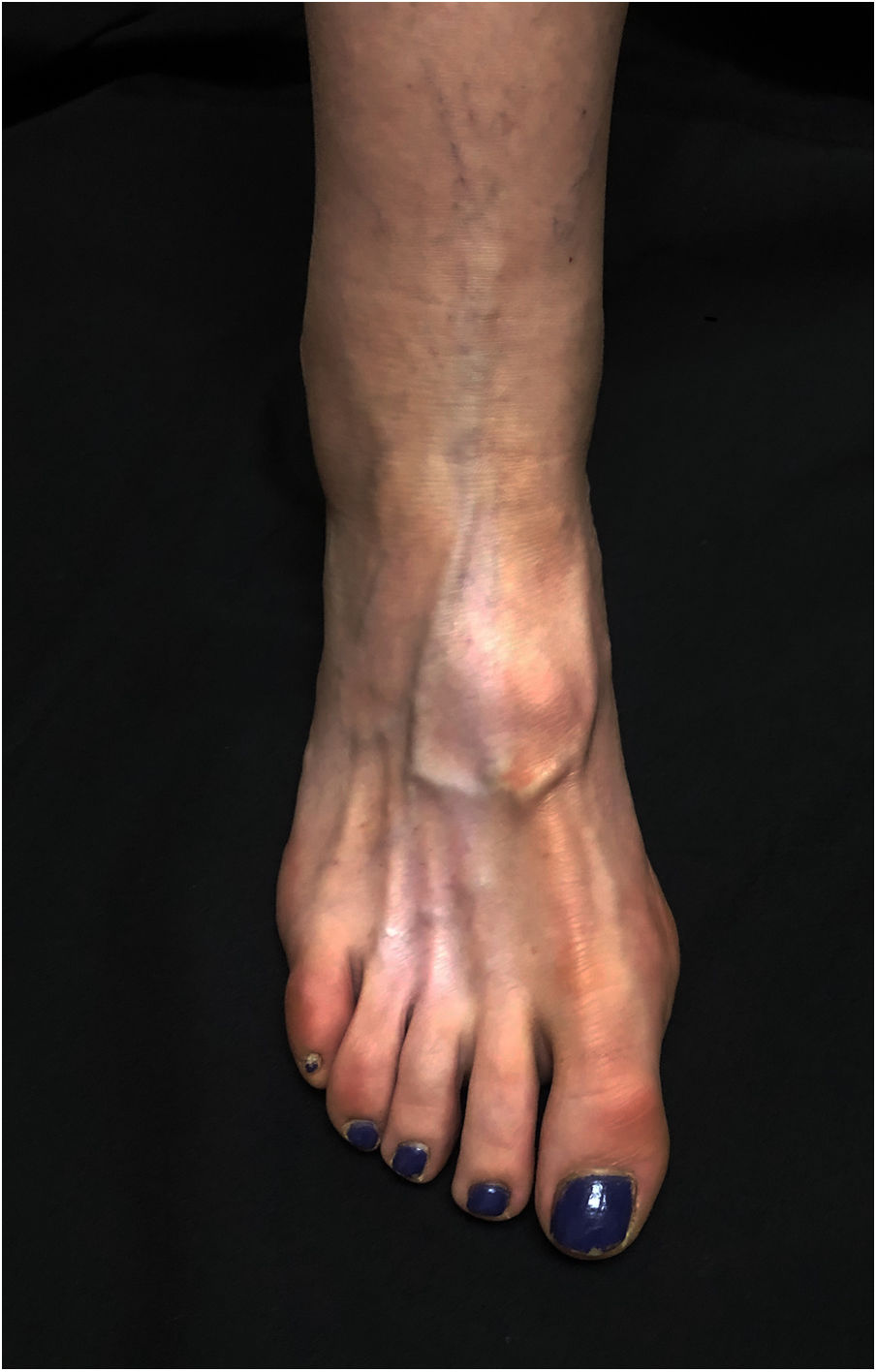
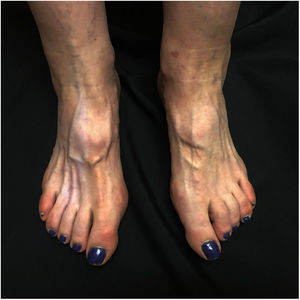
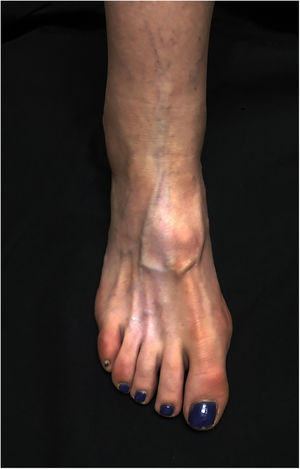
A 60-year-old woman presented with asymptomatic hypopigmentation of 3 months’ duration on the dorsum of the right foot. Three months earlier, she had been diagnosed with a painful interdigital neuroma that was treated with 2mL of triamcinolone acetonide (40mg/mL) injected into the third interdigital space of the right foot. The treatment relieved the pain. Physical examination showed a hypopigmented, atrophic patch on the dorsum of the foot and atrophy of the underlying muscles. The patch was triangular in shape and had well-defined borders; its base was located between the second and fourth metatarsals and ascended toward the ankle, running parallel to the lymphatic channels (Figs. 1 and 2). The local temperature and pedal pulses were normal. Based on the patient's medical history and the clinical findings, a diagnosis of perilymphatic atrophy and hypopigmentation secondary to intralesional corticosteroid injections was made.
Intralesional corticosteroids are an effective, widely used treatment in dermatology and rheumatology. They can, however, cause local adverse effects, such as pain, bleeding, infection, hair loss, local calcification, cutaneous hypopigmentation or hyperpigmentation, and atrophy.1,2 Atrophy and hypopigmentation typically occur at the site of injection,2 unlike perilesional/perilymphatic atrophy and hypopigmentation, which form a linear pattern and are less common.1 Clinical findings include a linear or branch-shaped pattern, although the final morphology varies according to the distribution of the lymphatic channels in the injection area. Perilesional/perilymphatic atrophy and hypopigmentation can occur after the administration of both intralesional2,3 and topical4 corticosteroids, with a time to onset of several weeks or even months. There have been some reports of this adverse effect following the treatment of epicondylitis,5 keloid scars,2 and tenosynovitis6 with intralesional corticosteroids. Cases such as ours (interdigital neuroma treated with intralesional triamcinolone acetonide) have been described less frequently. The main pathogenic factor involved is probably lymphatic spread of the corticosteroid suspension.1,3 Using Evans blue dye, the authors of a 1975 report linked atrophic lesions secondary to triamcinolone acetonide injections to the distribution of the lymph vessels.1 These lesions have only been described after triamcinolone acetonide injections. Triamcinolone acetonide is a macromolecule that dissolves slowly in order to achieve a prolonged effect. The lymph vessels could play an important role in the appearance of hypopigmentation along the course of the vessels by removing excess fractions of the molecule in its free state.3 Another explanation could be that intralesional triamcinolone acetonide is more widely used than other corticosteroid injections. Diagnosis is clinical. Histology shows atrophy of the epidermis and reduced melanin content without a loss of melanocytes,2 although a reduction in melanocyte numbers has been described.4 Treatment options are limited, and spontaneous repigmentation has been described between 6 and 12 months after diagnosis.2,3
In conclusion, we have described a rare adverse effect associated with the treatment of interdigital neuroma with intralesional corticosteroid injections. Familiarity with the characteristic morphologic features of this effect is important, as it helps avoid unnecessary tests. It is also important to inform patients of the risk of hypopigmentation, especially those with darker skin types.
Conflicts of InterestThe authors declare that they have no conflicts of interest.