Human immunodeficiency virus (HIV) transmission remains an important health issue, with a high burden that is felt across the world. This work aims to analyze the demographic, clinical, and laboratory characteristics of newly diagnosed patients with HIV in a Department of Dermatology and Venereology. A retrospective observational study was conducted from all health records of newly diagnosed patients with HIV from a Dermatology unit from January 2011 to December 2020. A total of 134 patients with new HIV diagnoses were included in the analysis. Concurrent dermatological or venereal diseases were diagnosed in 91.0% of the patients (n=122), being the most common conditions syphilis (22.4%, n=30) and urethritis (14.9%, n=20). Out of all the patients with diagnoses of concurrent sexually transmitted infection (STI) (41.0%, n=55), syphilis was reported in 81.8% of the patients (n=45), gonorrhea in 9.1% (n=5), and chlamydia in 5.5% (n=3). We present a large patient database on the clinical conditions associated with newly diagnosed HIV, concluding that infectious diseases were the most common conditions associated with newly diagnosed HIV.
La transmisión del virus de la inmunodeficiencia humana (VIH) continúa siendo un importante problema de salud a nivel mundial. En este estudio, se analizaron las características de pacientes recién diagnosticados con VIH en el Departamento de Dermatología y Venereología. Se realizó un estudio observacional retrospectivo de pacientes recién diagnosticados con VIH en un Departamento de Dermatología entre 2011 y 2020. Se incluyeron 134 pacientes con nuevos diagnósticos de VIH. Se diagnosticaron enfermedades dermatológicas o venéreas concurrentes en el 91.0% (n=122) de los pacientes, siendo las condiciones más comunes la sífilis (22.4%, n=30) y la uretritis (14.9%, n=20). De los pacientes con diagnósticos concurrentes de infección de transmisión sexual (ITS) (41.0%, n=55), 81.8% (n=45) fueron diagnosticados con sífilis, 9.1% (n=5) con gonorrea, 5.5% (n=3) con clamidia. Presentamos una amplia base de datos que describe las enfermedades relacionadas con el diagnóstico reciente de VIH, determinando que las enfermedades infecciosas fueron las más comunes asociadas con el VIH recién diagnosticado.
Human immunodeficiency virus (HIV) transmission remains an important health problem, with an impactful burden across the world. In 2020, 14971 cases of HIV were diagnosed in Europe.1 The last available report on HIV diagnosis in Portugal reported 778 new cases back in 2019, 50% of the patients presenting with a CD4+ count<350cells/mm3 (late presenters).2
Dermatologists play an important role in HIV diagnosis, as in many European countries such as Portugal, dermatologists are responsible for providing both dermatological and sexually transmitted infections (STI) care. In Italy, Mandel et al. found a yearly rate of HIV positive tests ranging from 0.1% to 1% in patients attending a Sexually Transmitted Diseases Ambulatory Dermatology Unit without a previous diagnosis.3 A similar work also conducted in Portugal by Mendes-Bastos et al. found a positivity rate of 3% in HIV of the patients who attended a Dermatology unit.4
The most common concomitant diagnosis made in newly diagnosed HIV patients in Dermatology units is syphilis, with an incidence rate ranging from 19% to 39%.4,5 Most newly diagnosed cases of HIV in this setting have a concomitant STI diagnosis (52–61%).4,5 Besides STI, other dermatological conditions previously described associated with HIV diagnosis include prurigo nodularis, psoriasis, shingles, and Kaposi sarcoma.4,5
This work aims to characterize the demographic, clinical, and laboratory characteristics of patients with newly diagnosed HIV infections in the Department of Dermatology and Venereology of a Portuguese hospital.
Materials and methodsStudy populationA retrospective observational study was conducted including all medical records from patients newly diagnosed with HIV in the Dermatology Clinic, Urgent Care Dermatology Clinic, and Dermatology Inpatient Ward of Centro Hospitalar Universitário Lisboa Norte, Lisbon, Portugal from January 2011 to December 2020 (10 years).
HIV screening can be offered to patients with clinical suspicion of infection, undergoing STI screening before ward admission or surgery, or whenever the clinician would think an HIV test could be beneficial. All newly diagnosed HIV infections were referred to an Infectious Disease unit to pursue treatment and follow-up.
Data collectionWe included all newly diagnosed patients with HIV infection in the Dermatology Department. Patients younger than 18 years old were excluded due to ethical considerations. Health records were assessed for age, gender, nationality, sexual orientation, no. of sexual partners in the past 6 months, reason for screening, dermatological diseases, sexually transmitted co-infections, CD4 cell count, and HIV viral load.
Laboratory screening was conducted with an electrochemiluminescence immunoassay for antibodies to HIV-1, HIV-2, and HIV p24 antigen – Elecsys® HIV Duo, Roche. As per our institution protocol, all positive screening results were confirmed by HIV-1 and HIV-2 Geenius™ HIV 1/2 Confirmatory Assay, Bio-Rad. HIV viral load was determined by real-time polymerase chain reaction (PCR) assay on a subsequent plasma sample using cobas® HIV-1 quantitative nucleic acid test to be used on the cobas® 6800/8800 Systems.
Appropriate samples were collected for syphilis, hepatitis B and C testing, and laboratory testing of other STIs, including gonorrhea, chlamydia, and M. genitalium.
Statistical analysisStatistical analysis was performed using the Mann–Whitney test. P values<.05 (2-tailed) were considered statistically significant. The statistical package for social sciences software (IBM® SPSS Statistics® for Macintosh, version 27.0.1.0: IBM Corporation) was used.
Ethical disclosuresThis observational, retrospective study was conducted in full compliance with the principles of the Declaration of Helsinki. Ethics committee approval was obtained (315/21; December 15, 2021).
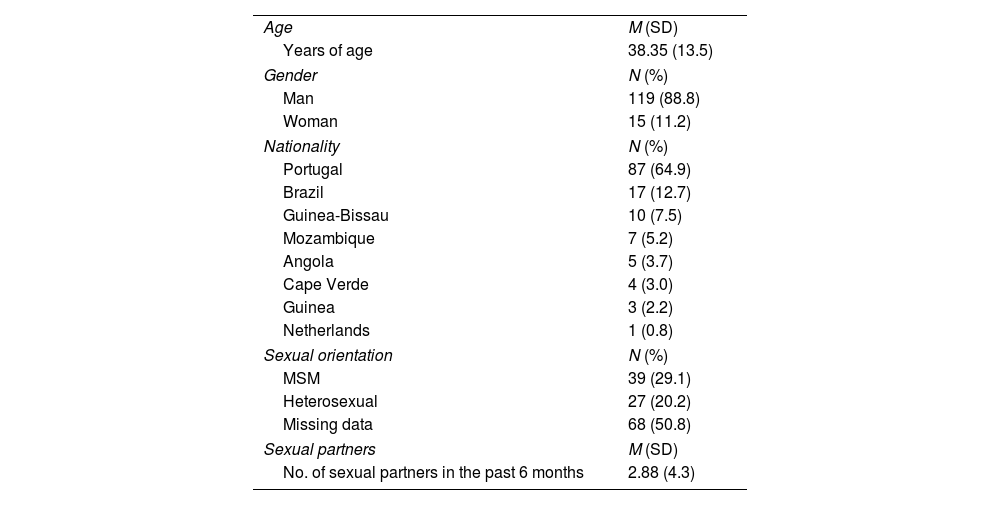
ResultsStudy populationA total of 134 newly diagnosed patients with HIV were included in this study. Men represented 88.8% of the population (n=119), with a mean age of 38.4 years (SD, 13.5). A total of 8 different nationalities were recorded; 64.9% of the patients (n=87) were Portuguese, and 35.1% (n=47) had nationalities different than Portuguese (Table 1). Out of the 49.3% patients with recorded sexual practices (n=66), 59.1% (n=39) were identified as men who had sex with other men, and 40.9% (n=27) as heterosexual.
Study population.
| Age | M (SD) |
| Years of age | 38.35 (13.5) |
| Gender | N (%) |
| Man | 119 (88.8) |
| Woman | 15 (11.2) |
| Nationality | N (%) |
| Portugal | 87 (64.9) |
| Brazil | 17 (12.7) |
| Guinea-Bissau | 10 (7.5) |
| Mozambique | 7 (5.2) |
| Angola | 5 (3.7) |
| Cape Verde | 4 (3.0) |
| Guinea | 3 (2.2) |
| Netherlands | 1 (0.8) |
| Sexual orientation | N (%) |
| MSM | 39 (29.1) |
| Heterosexual | 27 (20.2) |
| Missing data | 68 (50.8) |
| Sexual partners | M (SD) |
| No. of sexual partners in the past 6 months | 2.88 (4.3) |
MSM: men who have sex with men.
A total of 134 new HIV diagnoses were achieved during the 10 years of this study. The mean number of diagnoses per year was 13.4 (SD, 3.9), with a range of 5–17 diagnoses per year. Most cases were diagnosed in the Urgent Care Dermatology Clinic (67.9%), followed by the Dermatology Clinic (28.4%) and the Inpatient Ward (3.7%). The reasons for prescribing a HIV test were STI screening [56.0% (n=75)], clinical suspicion [38.1% (n=51)], and other reasons [6.0% (n=8)].
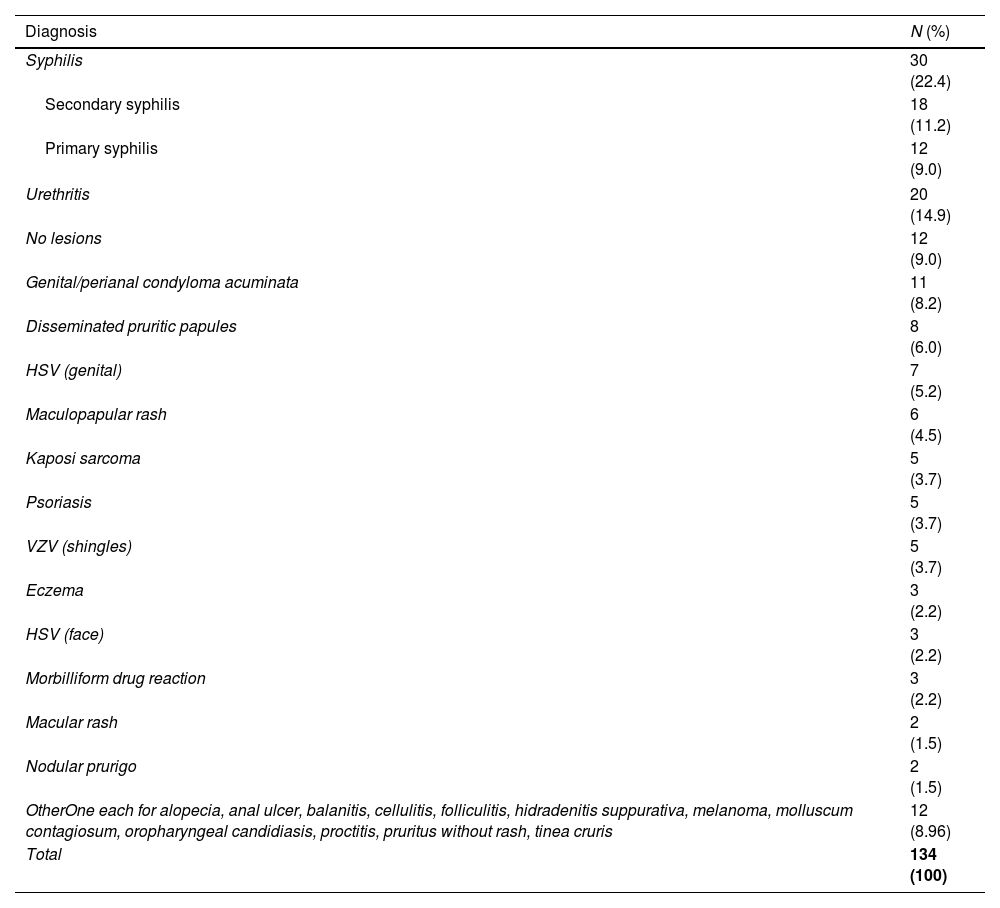
Clinical characteristicsConcurrent dermatological or venereal diseases were diagnosed in 91.0% of the patients (n=122). The dermatological and venereal diseases, which are consistent with newly HIV diagnosed patients are summarized in Table 2, being the most common conditions syphilis (22.4%, n=30), urethritis (14.9%, n=20), and genital/perianal condyloma acuminata (8.2%, n=11).
Concomitant diagnosis in newly diagnosed patients with HIV.
| Diagnosis | N (%) |
|---|---|
| Syphilis | 30 (22.4) |
| Secondary syphilis | 18 (11.2) |
| Primary syphilis | 12 (9.0) |
| Urethritis | 20 (14.9) |
| No lesions | 12 (9.0) |
| Genital/perianal condyloma acuminata | 11 (8.2) |
| Disseminated pruritic papules | 8 (6.0) |
| HSV (genital) | 7 (5.2) |
| Maculopapular rash | 6 (4.5) |
| Kaposi sarcoma | 5 (3.7) |
| Psoriasis | 5 (3.7) |
| VZV (shingles) | 5 (3.7) |
| Eczema | 3 (2.2) |
| HSV (face) | 3 (2.2) |
| Morbilliform drug reaction | 3 (2.2) |
| Macular rash | 2 (1.5) |
| Nodular prurigo | 2 (1.5) |
| OtherOne each for alopecia, anal ulcer, balanitis, cellulitis, folliculitis, hidradenitis suppurativa, melanoma, molluscum contagiosum, oropharyngeal candidiasis, proctitis, pruritus without rash, tinea cruris | 12 (8.96) |
| Total | 134 (100) |
HSV, herpes simplex virus; VZV, varicella-zoster virus.
Out of all the patients with concurrent sexually transmitted infection (STI) diagnoses confirmed through lab testing (41.0%, n=55), syphilis was diagnosed in 81.8% of the patients (n=45), gonorrhea in 9.1% (n=5), chlamydia infection in 5.5% (n=3), hepatitis C virus and Haemophilus parainfluenza each in 1.8% (n=1). Out of all the syphilis diagnosed, 26.7% (n=12) were staged as primary syphilis, 40% (n=18) as secondary, 20% (n=9) as early latent, and 13.3% (n=6) as latent of unknown duration.
HIV stageOut of the 65.7% patients (n=88) with recorded CD4 cell count, 54.5% (n=48) were late presenters (LP) (CD4 count≤350cells/mm3), 35.2% (n=31) presenting with AIDS defining cell counts (CD4 count≤200cells/mm3), while 45.5% (n=40) diagnosed early in their infection were early presenters (EP) (CD4 count>350cells/mm3). HIV viral load was recorded for 28.4% of the patients (n=38), with a median viral load of 70325copies/mL (IQR, 21186–70325).
The mean viral load for EP was 55931.0copies/mL (IQR, 8905–398128) and 77280copies/mL (IQR, 22663–297850) for LP. Patients presenting with an STI had significantly higher CD4 counts (392cells/mm3; IQR, 269–590) compared to those with a negative STI testing (133cells/mm3; IQR, 27–326) (P=.020).
DiscussionHIV diagnosis continues to be a challenging subject amongst health care providers. Dermatology and Venereology Departments are responsible for providing health counseling on STIs, thus having a privileged position to take action on HIV diagnosis. As far as we know, this is the largest published database on newly diagnosed patients with HIV in a dermatological setting.
Our study has important limitations. First, there is a selection bias; patients attending our unit are prone to having more serious, or atypical conditions that require a specialized assessment in a tertiary care center such as ours. Secondly, there is information bias since all data was gathered through previously recorded medical data, with a significant percentage of missing data.
A total of 134 patients were diagnosed in the 10-year period of this study, with a mean no. of diagnoses per year of 13.4, a slightly higher rate compared to previous results.3–5 The high rate of diagnoses could be explained by the unique characteristics of our Department, with an available walk-in Dermatology Urgent Care Clinic available on a daily basis, also corroborated by the elevated rate of cases diagnosed in this clinic (67.9%).
Most HIV diagnoses were matched with a dermatological or venereological diagnosis. Regarding the cases without a diagnosis, the positive HIV testing resulted from STI screening in asymptomatic patients, mostly latent syphilis. The most common associated conditions were infectious, with STI accounting for most diagnoses. STIs cause mucosal inflammation, or ulcers in the oral and anogenital areas and increase the risk of HIV transmission.6 In our study, 41.0% of the patients tested positive for a STI, which is similar to what former studies have reported,4,5 with syphilis, gonorrhea, and chlamydia accounting for most of the cases (96.4% of the patients with a laboratory diagnosis of STI). Syphilis showed an extraordinarily high prevalence, with 1 out of 3 patients newly diagnosed with HIV also testing positive for syphilis (33.6%, n=45). Our results once again reinstate that the syphilis epidemic is still a matter of great interest, with the need for policies on screening, treatment, and prevention.7
Our results showed that several dermatoses usually not associated with HIV diagnosis could be found, once again stating the importance of HIV screening programs among health institutions as an approach to increasing diagnosis.1 Regarding dermatosis – excluding STIs – Kaposi sarcoma, psoriasis, and shingles were some of the most common conditions associated with a diagnosis of HIV, a result similar to previously published data.4,5
Of all the patients with recorded CD4 cell count, most were LP (54.5%), and 35.2% presented with AIDS-defining cell counts. Patients presenting with an STI had significantly higher CD4 counts (392cells/mm3) compared to patients with a negative STI testing (133cells/mm3). We hypothesize that patients with a STI are commonly more symptomatic and seek medical help earlier compared to other dermatoses, resulting in a higher CD4 cell count at diagnosis.
HIV and particularly LP are still a major health concern across Europe, where 48% of newly diagnosed HIV patients are LP.8 In Portugal, the rates of patients with newly diagnosed HIV presenting with AIDS ranged from 14.0% to 21.4% from 2010 to 2019, a lower prevalence than that of our study.2
Patients who present as EP to health care providers with good linkage to care can initiate antiretroviral therapy earlier, resulting in viral suppression, decreased rates of co-morbidities, and prevention of future opportunistic infection acquisitions. Therefore, this database on HIV diagnosis associated with dermatosis is crucial to establish plans and recommendations on testing, improving early diagnosis, and reducing morbidity and onward transmission.
Conflict of interestsThe authors declare that they have no conflict of interest.