Gold sodium thiosulfate (GST) is a common sensitizer that is very prevalent in the environment. It was named allergen of the year by the North American Contact Dermatitis Society in 2001, and in 2012, it was included in the T.R.U.E. TEST allergen panel. T.R.U.E. TEST is a ready-to-use diagnostic test comprising 36 substances in 3 custom-prepared panels that provides the optimal allergen concentration in each of its patches. Consequently, since it first appeared, it has become increasingly used in dermatology departments, to the extent that it is now the standard series in many hospitals. The use of gold in patch tests is controversial. Its results are difficult to interpret, and, like many other metals, it is a common irritant. Consequently, it has been associated with late and persistent reactions (the possibility of active sensitization has even been considered). Furthermore, its relevance is difficult to identify, and the exact mechanisms by which this substance interacts with the human body remain unknown.1–8
The objective of the present study was to determine where GST ranks in the order of frequency of sensitizers causing positive results in patients seen in the contact allergy department. We also aimed to identify the demographic characteristics of patients who tested positive to GST, establish the relevance of the positive results, and define the usefulness of standardized patch testing with the allergen.
We performed an observational retrospective epidemiological study of all patients seen in the contact allergy department of a tertiary hospital from January to June 2015. Of the 234 patients seen, 85 (36.32%) were excluded because either they had not undergone patch testing or the results of their patch tests were negative. The series used was the T.R.U.E. TEST. For all patients, the variables studied were as follows: age, sex, profession, known allergies, intolerance to metals, time since lesions first appeared, symptoms, location, patient's identification of contactant, presence of any other skin complaint, and frequency of positive results in the T.R.U.E. TEST. Data were processed and analyzed using SPSS version 11.5 for Windows (SPSS Inc). Qualitative variables were compared using the chi-square test with a Yates correction or the Fisher exact text when the conditions for applying the chi-square test could not be met.
The 5 most common allergens were nickel sulfate, GST, thiazolinones, fragrance mix, and paraphenylenediamine. A total of 35 patients (23.5%) tested positive for GST, which came second to nickel sulfate (55.7%) in the present series. Dermatitis affected the hands in 57.1% of cases. No significant differences were detected with respect to age, sex, profession, intolerance to metal, and known allergies. Of the patients who tested positive to GST, 82.9% could not identify a contactant (P=.012). In addition, 17.1% were positive for GST only, whereas 99.1% of those who tested negative with GST were sensitized to ≥2 allergens (P=.001). We cannot rule out differences with respect to co-occurrence with other skin complaints (P=.078) (Table 1).
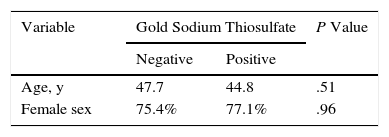
Demographic Characteristics of Patients Who Tested Positive for ≥1 of the Allergens Tested.
| Variable | Gold Sodium Thiosulfate | P Value | |
|---|---|---|---|
| Negative | Positive | ||
| Age, y | 47.7 | 44.8 | .51 |
| Female sex | 75.4% | 77.1% | .96 |
| Profession | Homemaker | 21.1% | Industrial materials | 17.1% | .49 |
| Industrial materials | 18.4% | Homemaker | 14.3% | ||
| Hotel and catering | 8.8% | Hotel and catering | 11.4% | ||
| Health care | 7.9% | Health care | 11.4% | ||
| Construction | 7.0% | Students | 8.6% | ||
| Students | 7.0% | Construction | 5.7% | ||
| Hairdressers | 3.5% | Agriculture | 5.7% | ||
| Long-term retired | 2.6% | Hairdressers | 5.7% | ||
| Agriculture | 0.9% | Long-term retired | 2.9% | ||
| Long-term unemployed | 0.0% | Long-term unemployed | 2.9% | ||
| Other (low-risk) | 17.5% | Other (low-risk) | 11.4% | ||
| Unknown | 5.3% | Unknown | 2.9% |
| Intolerance to metals | 48.2% | 48.6% | .97 |
| Known allergies | None | 62.3% | None | 60.0% | .30 |
| Other | 14.9% | Drugs | 20.0% | ||
| Drugs | 11.4% | Drugs and other | 8.6% | ||
| Foods | 3.5% | Other | 5.7% | ||
| Drugs and other | 3.5% | Foods and other | 2.9% | ||
| Drugs and foods | 2.6% | All | 2.9% | ||
| Foods and other | 0.9% | Foods | 0.0% | ||
| All | 0.9% | Foods and drugs | 0.0% |
| Personal history of atopy | 39.0% | 45.7% | .51 |
| High IgE levels | 22.8% | 28.6% | .49 |
| Positive RAST results | 1: 3.5% | 1: 0.0% | .53 |
| >2: 23.7% | >2: 25.7% | ||
| Course | 39.5 mo | 35.6 mo | .90 |
| Clinical manifestations | Acute eczema | 81.6% | Acute eczema | 74.3% | .35 |
| Pruritus | 64.9% | Pruritus | 68.6% | .69 | |
| Nonspecific lesions | 46.5% | Nonspecific lesions | 45.7% | .94 | |
| Chronic eczema | 35.1% | Chronic eczema | 42.9% | .41 | |
| Urticaria | 11.4% | Urticaria | 2.9% | .11 | |
| Location | Various sites | 37.7% | Upper limbs | 40.0% | .51 |
| Upper limbs | 25.4% | Various sites | 28.6% | ||
| Head and neck | 18.4% | Head and neck | 11.4% | ||
| Trunk | 10.5% | Trunk | 11.4% | ||
| Lower limbs | 7.0% | Lower limbs | 5.7% | ||
| Unknown | 0.9% | Unknown | 2.9% |
| Contactant identified | 40.4% | 17.1% | .01 |
| Other skin complaints | 66.7% | 50.0% | .08 |
| Only 1 positive result in the T.R.U.E. TEST | 0.9% | 17.1% | .00 |
Abbreviation: RAST, radioallergosorbent test.
No contactant was identified in most of the GST-allergic patients. Many studies point to the ability of GST to cause irritation, persistent reaction, or even active sensitization. Although the dose used in the T.R.U.E. TEST series (75μg/cm2) meets the criteria for the minimum concentration for a positive reaction (+ or ++), some patients were seen to react to low concentrations of GST but not to slightly higher concentrations; therefore, reactivity to GST could involve underlying factors other than the concentration (eg, interactions between local amino acids, pressure, friction, skin damage, and eczema). The North American Contact Dermatitis Group recently decided to remove gold from its standard series,1 and the Spanish Contact Dermatitis and Skin Allergy Research Group does not include gold in its standard series. Therefore, we propose withdrawing GST from the widely used T.R.U.E. TEST series. Furthermore, patients who test positive to GST are sensitized to a single allergen more commonly than patients who are sensitized to allergens other than GST, and patients with a positive T.R.U.E. TEST result who test negative for GST were followed more frequently in the dermatology department for other skin complaints. This observation could be associated with the major presence of gold in many areas of our lives. The considerable stability of gold means that it is difficult to find it in its ionic form at concentrations sufficiently high to cause reactions, although concentrations may be sufficiently high to cause sensitization.9
Please cite this article as: Arteaga-Henríquez M, Latour-Álvarez I, García-Peris E, Pérez-Robayna N. Estudio epidemiológico, observacional y retrospectivo de la sensibilización a tiosulfato sódico de oro en la consulta de alergias de contacto de un hospital de tercer nivel. Actas Dermosifiliogr. 2017;108:164–166.