Recently, Abarzúa-Araya et al.1 published an article describing a dermatofibroma (DF) with osseous metaplasia. We present the case of a patient with DF with sebaceous induction in order to illustrate the marked histopathological variability of this tumor and the value of dermoscopy in its diagnosis.
The patient was a 68-year-old woman with a past history of hypertension, dyslipidemia, and hypothyroidism. She consulted for a stable, asymptomatic lesion that had arisen on her left shoulder more than 10 years earlier.
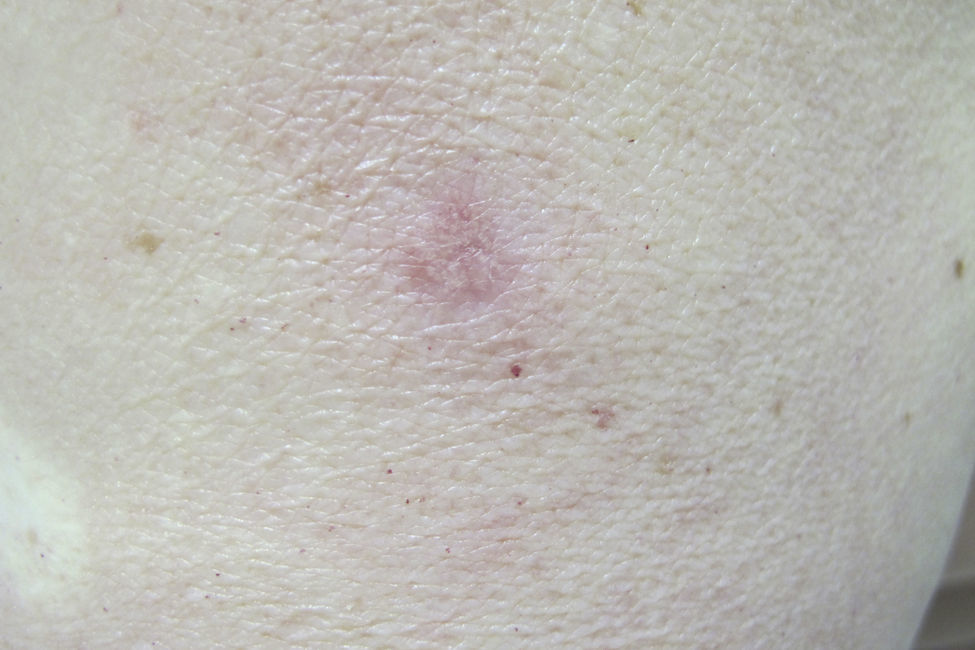
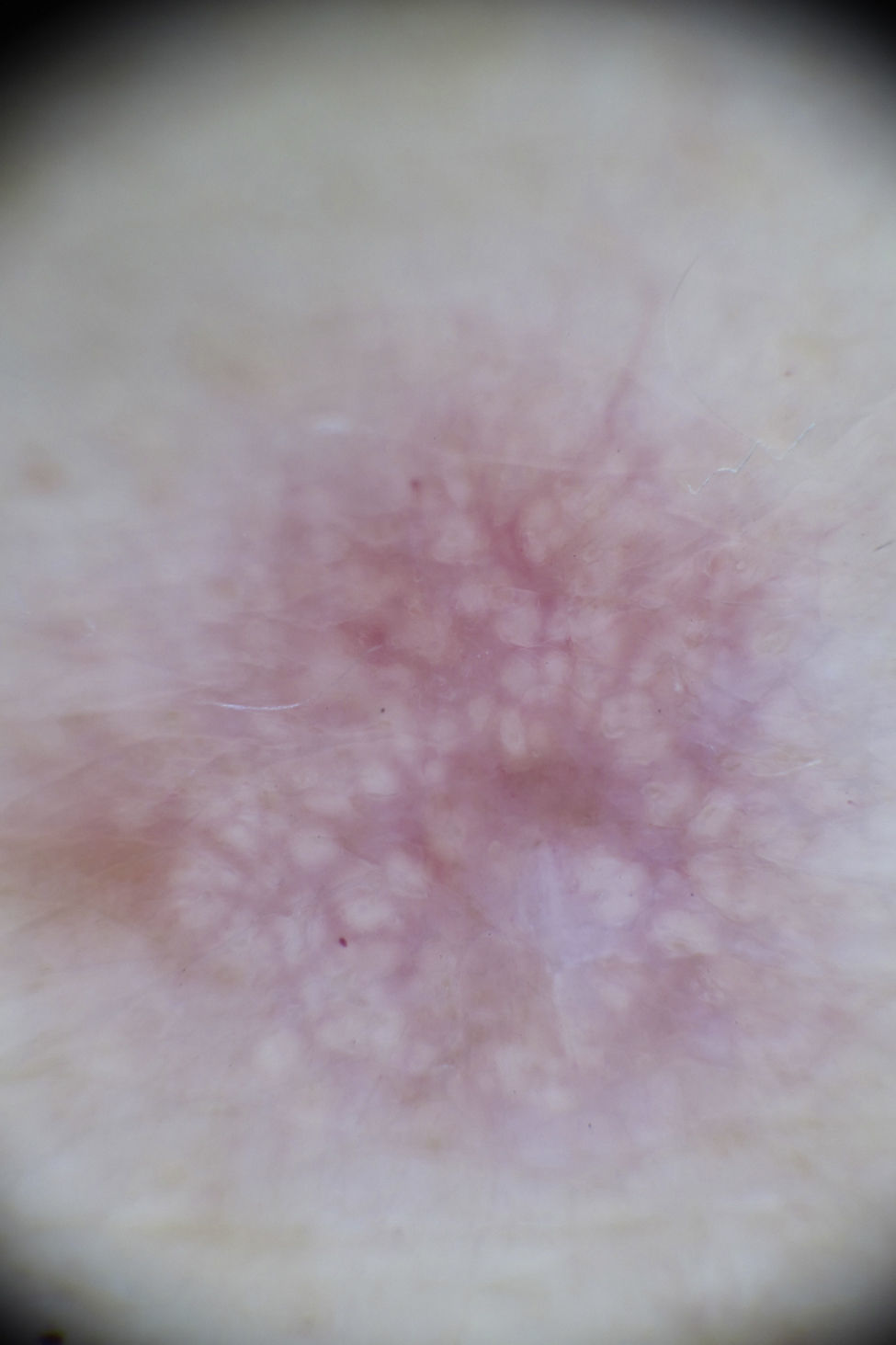
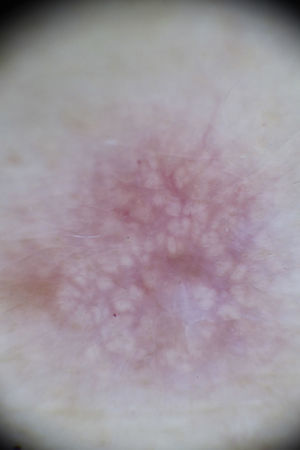
Physical examination revealed a firm pink tumor measuring 1cm in diameter on the lateral aspect of the proximal third of the patient's left arm (Fig. 1). The lesion had a smooth surface and presented the dimple sign. On dermoscopy, yellowish globules were observed in association with vascular erythematous areas. Focally, in some peripheral areas, the lesion presented a delicate pigment network and a white patch (Fig. 2).
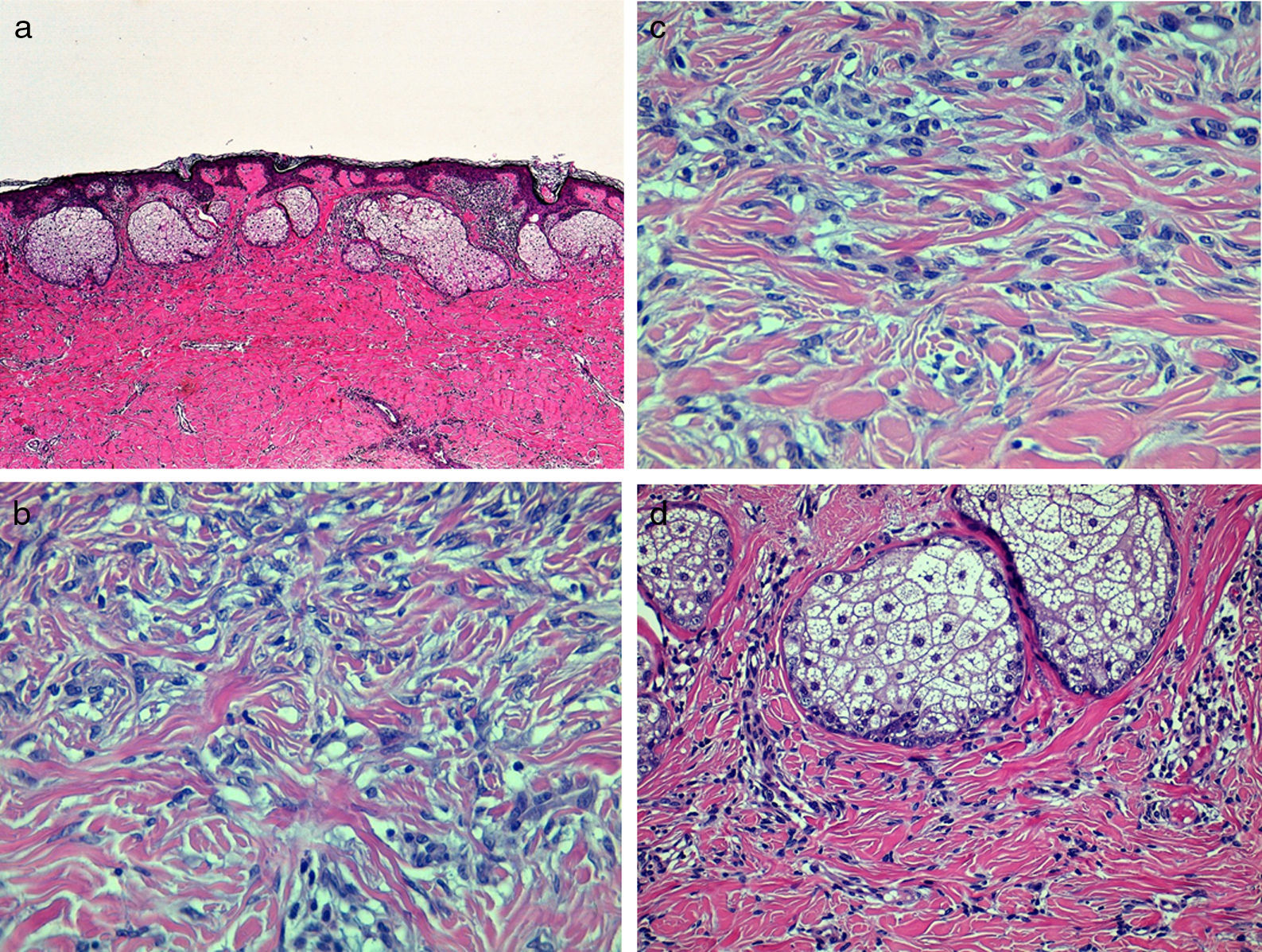
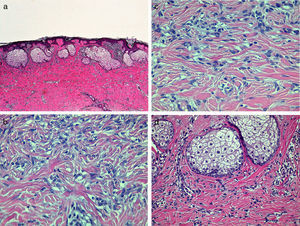
The lesion was excised and histopathology revealed a hyperplastic epidermis with slight hyperpigmentation of the basal layer. A poorly defined nodular proliferation formed of spindle-shaped cells with no cytologic atypia was present in the dermis. Greater cell density was observed in the more superficial areas, while the intermediate level was predominantly sclerotic. Nests of sebaceous cells were present in the upper dermis (Fig. 3). Staining with factor xiiia was strongly positivity in the nuclei of the fibroblastic cells.
A, A poorly defined proliferation of spindle-shaped cells with nests of sebaceous cells in the more superficial region. Hematoxylin and eosin (H&E), original magnification×40. B, At higher magnification, a dermal proliferation formed of spindle-shaped cells with a whorled pattern. H&E, original magnification×200. C, Entrapment of collagen fibers between fibroblastic cells at the periphery of the lesion. H&E, original magnification×200. D, The nests of sebaceous cells at higher magnification. H&E, original magnification×100.
DF is a very common, benign fibrohistiocytic tumor that typically presents as a firm, brownish-pink, dome-shaped lesion measuring less than 1cm in diameter, localized on the lower extremities of adult women. Although the definitive diagnosis requires histopathology, dermoscopy is useful to differentiate DF from other pigmented skin lesions, such as malignant melanoma, Spitz nevus, atypical melanocytic nevus, and seborrheic keratosis.2
Zaballos et al.3 described 10 global dermoscopy patterns for DF. The most common is the delicate peripheral pigment network and central white patch, present in 34.7% of cases. Other patterns are pigment network, pigment network and central white network, white network, homogeneous, total white patch, multiple white patches, homogeneous with central white patch, homogeneous with white network, and atypical (multicomponent). Vascular structures are observed in approximately half of lesions.
Many histopathologic variants of DF exist, such as fibrocollagenous, histiocytic, sclerotic or atrophic, storiform, cellular, deep, hemosiderotic, palisading, myxoid, clear cell, epithelioid, keloid, lipidized, and with presence of granular cells, osseous metaplasia, cholesterol crystals, or atypical cells (pseudosarcomatous).1,4 Acanthosis, hyperkeratosis, and hyperpigmentation are often observed in the overlying epidermis, sometimes mimicking seborrheic keratosis. Adnexal induction has also been reported in the sebaceous and follicular form.4,5 This broad histopathological variability leads to distinct dermoscopic findings, with some variants having certain dermoscopic characteristics that aid in their diagnosis. Examples of these are the hemosiderotic/aneurysmal DF, which has a central area of homogeneous bluish or erythematous-violaceous pigmentation, and the lipidized DF, with a homogeneous yellowish area.3,6
Although initially considered rare, sebaceous structures are identified in more than 15% of DFs,4,5,7 even in multiple forms.8 This finding is typical in lesions localized in the anatomical area of the shoulder (shoulder, proximal region of the arm, upper back and deltoid region), being observed in more than 40% of these cases, particularly in DF with seborrheic keratosis-type epidermal hyperplasia or with a sclerotic pattern.4 The dermoscopic image shows yellowish globular structures due to the sebaceous component.6 Although growth factors and cytokines have been implicated,9 the etiology of sebaceous induction and the reason for its predilection for DF of the shoulder remain unknown.4
In this case, the differential diagnosis should include sebaceous tumors and tumors with sebaceous differentiation, such as sebaceous hyperplasia, sebaceous nevus, sebaceous adenoma, sebaceous carcinoma, and reticulated acanthoma or poroma with sebaceous differentiation, which can include yellowish structures in the dermoscopy image.10 Yellowish globules have also been identified in melanocytic nevi and balloon cell melanomas.
In conclusion, DF is a tumor with a marked variability of its clinical, histopathological, and dermoscopic presentation. A diagnosis of DF with sebaceous induction should be considered in lesions in the shoulder area with yellowish globules visible on dermoscopy.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Monteagudo B, Figueroa-Silva O, Suárez-Amor O, Álvarez JC. Hallazgos clínicos, dermatoscópicos e histopatológicos de un dermatofibroma con inducción sebácea. Actas Dermosifiliogr. 2017;108:874–876.