Güngör et al.1 recently published the dermoscopic and confocal microscopy findings of an aneurysmal dermatofibroma (ADF). In this paper we describe the usefulness of Doppler in the diagnosis of this entity.
Case 1A 64-year-old man was seen for a 1-year history of an abdominal wall tumor that presented episodes of increase in size, redness, and pain. The patient had undergone surgery 2 years earlier for squamous cell carcinoma of the pharynx; the metastatic work-up had shown no signs of recurrence or distant tumor spread.
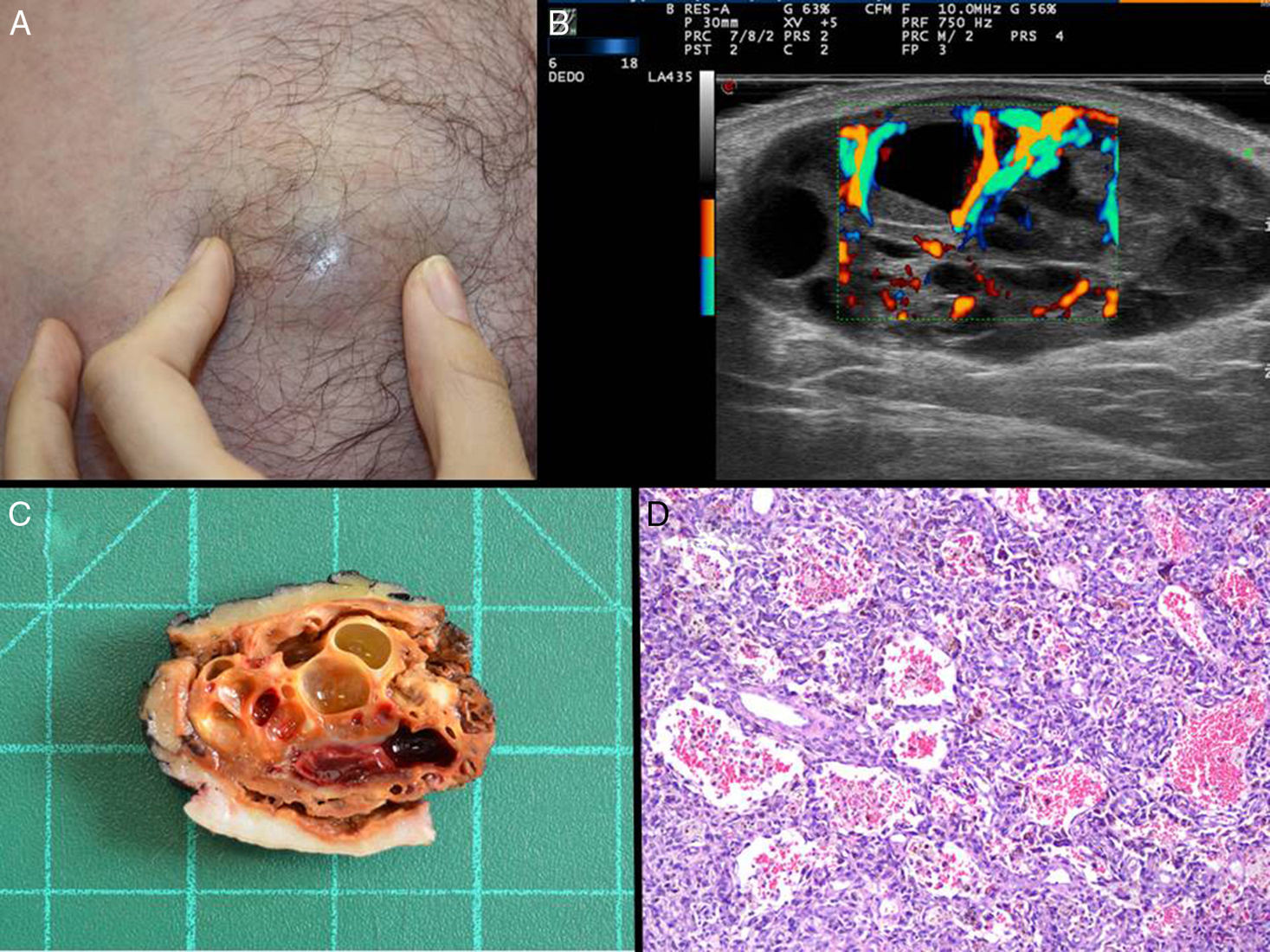
Physical examination revealed a tender violaceous tumor of 3.5cm in diameter in the mesogastric region (Fig. 1A). Ultrasound showed a well-defined lesion measuring 37×15.7mm in the subcutaneous cellular tissue. The lesion was composed of anechoic lacunae separated by hypoechoic septa. These septa were enhanced on color Doppler (Fig. 1B). The histopathologic diagnosis after excision of the lesion was ADF (Fig. 1, C and D).
Case 1. A, Nodule in the mesogastric region. B, Color Doppler, longitudinal axis, 18Mhz. In the subcutaneous cellular tissue, a well-defined tumor formed of anechoic lacunae surrounded by hypoechoic septa with flow in their interior (center and left of the image) and destructured hypoechoic areas (right side of the image). C, Macroscopic appearance of the tumor after surgical excision, showing the lacunar structures visible on ultrasound. D, Ectasias containing red blood cells but with no endothelium, surrounded by cells of fibrohistiocytic appearance. Hematoxylin and eosin, original magnificationx100.
This patient was a woman aged 34 years. She presented a lesion that had arisen on her right arm 2 years earlier and that had become pruritic in the previous 4 months. She had a past history of surgery for ectopic breast tissue and polycystic ovary syndrome on treatment with oral contraceptives.
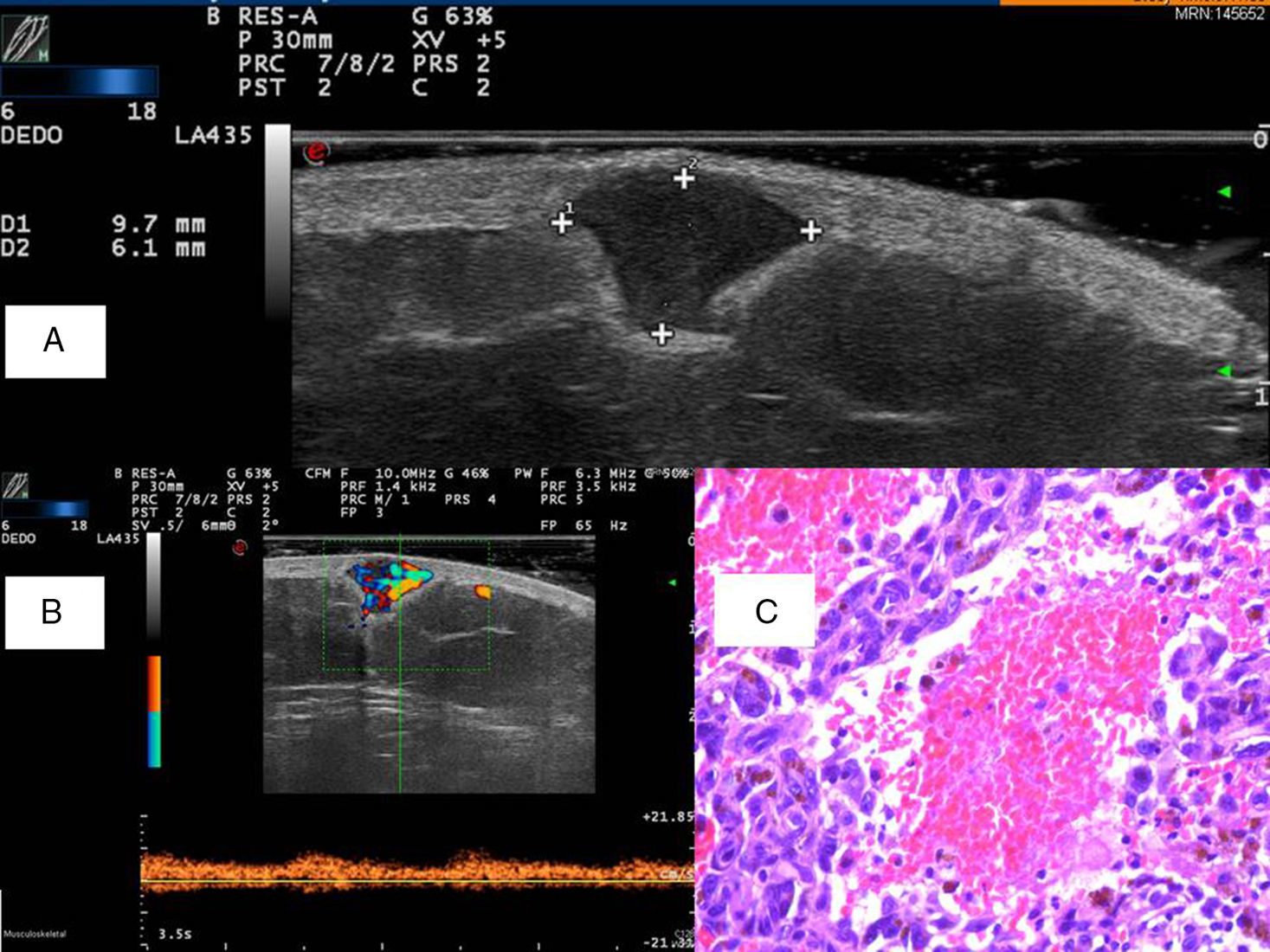
Physical examination revealed a nontender violaceous papule of 5mm in diameter. On ultrasound we observed a well-defined, hypoechoic lesion with a central anechoic area (Fig. 2A). Color Doppler revealed complete filling of the lesion with the exception of a small anechoic area. Pulsed Doppler showed a venous wave (Fig. 2B). The histopathologic diagnosis after excision was ADF (Fig. 2C).
Case 2. A, Gray scale: Well-defined hypoechoic lesion situated in the dermis and in the subcutaneous cellular tissue. B, Pulsed Doppler: Filling of the lesion with a venous wave. C, Ectasia containing red blood cells but with no endothelium, surrounded by fibrohistiocytic cells and extravasated red blood cells. Hematoxylin and eosin, original magnificationx400.
Dermatofibroma is a common benign cutaneous tumor. ADF is a rare clinical-pathologic variant described by Santa Cruz and Kyriakos in 19812; it accounts for less than 1.7% of all dermatofibromas. ADF presents as a violaceous or bluish tumor and is usually larger than the more common variants. It may show a sudden spontaneous increase in size or pain due to intratumoral hemorrhage. These tumors usually arise on the limbs; only 12% are found on the trunk. The postsurgical recurrence rate is 19%, and although the lesions are usually limited to the dermis, they can sometimes extend into the hypodermis and affect lymph nodes or bone.3,4 Histopathology reveals cells with a fibrohistiocytic appearance, blood vessels, and hemosiderin surrounding ectatic blood-filled spaces. These spaces have no endothelial lining.3
Dermoscopically, the lesion has been described as a central homogeneous bluish or reddish area, a peripheral pigment network, and central whitish linear structures.5
Confocal microscopy shows hyporeflective areas, which correspond to the vascular zones, associated with other hyperreflective areas, which correspond to the more dense cellular zones.1
Dermatofibroma has been described on ultrasound as a solid hypoechoic nodule, in the form of a well-defined disc localized in the dermis or hypodermis, usually producing distortion of adjacent hair follicles and occasionally showing peripheral vascularization.6–8 In the literature we have found no descriptions of the ultrasound findings of ADF, though the findings of angiomatoid fibrohistiocytoma have been published.9 Hata et al.9 described a patient aged 77 years with a 4-month history of a lesion in the temporal region that, on ultrasound, presented anechoic structures with no Doppler flow, interpreted as vascular channels filled with blood, and peripheral hypoechoic areas with different degrees of vascularization, which they considered to be more cellular areas with blood vessels. In our first case, we could also make this same ultrasound-histologic correlation, though this was a longer-standing lesion, of larger size, with numerous intratumoral bleeds, and with more ectatic areas. Given the patient's past history, the differential diagnosis included a possible skin metastasis, although the lesion was very homogeneous and of pseudoencapsulated appearance.
In our second case, the marked vascularization present on Doppler led us to consider a differential diagnosis with venous malformations. On ultrasound, venous malformations are seen as tubular structures, occasionally with hyperechoic structures with a posterior shadow (phleboliths), with a venous wave on pulsed Doppler. In this case, as the lesion was small and had not presented episodes of increasing size, we observed a predominance of areas with Doppler flow and a smaller anechoic central region.
In conclusion, Doppler can be a very useful tool for the diagnosis of ADF. The anechoic areas with no flow correspond histologically to the ectatic areas and the regions with Doppler flow correspond to the vascularized and cellular areas.
Conflicts of InterestThe authors declare that they have no conflicts of interest.
Please cite this article as: Echeverría-García B, García-Donoso C, Tardío JC, Borbujo J. Ecografía Doppler en el dermatofibroma aneurismático. Actas Dermosifiliogr. 2017;108:159–161.